Overview of Tubular Transport - The Kidney's Sorting Hat
Tubular fluid modified by reabsorption & secretion. $Excretion = Filtration - Reabsorption + Secretion$.
- Reabsorption: Tubule lumen → peritubular capillary.
- Secretion: Peritubular capillary → tubule lumen.
- Pathways:
- Transcellular: Through epithelial cells.
- Paracellular: Between cells via tight junctions.

| Feature | Active Transport | Passive Transport |
|---|---|---|
| Energy | Requires ATP (direct/indirect) | No direct ATP needed |
| Gradient | Can move against concentration gradient | Moves down electrochemical gradient |
| Examples | Primary: Na+/K+ ATPase; Secondary: SGLT | Diffusion, Osmosis |
- Renal Threshold: Plasma concentration at which a substance first appears in urine.
- Glucose: ~180-200 mg/dL.
⭐ Transport maximum (Tm) is a critical concept for substances like glucose, where reabsorptive capacity is limited by carrier saturation.
Proximal Tubule Powerhouse - The Heavy Lifter
Dominant site for reabsorption/secretion; brush border & Na+/K+ ATPase are key.
- Major Reabsorption:
- ~65-70% Na+ & H2O.
- 100% Glucose (SGLT2), Amino Acids.
- ~80-90% $HCO_3^-$ (via $H^+ + HCO_3^- \leftrightarrow H_2CO_3 \leftrightarrow H_2O + CO_2$).
- ~50% Urea; also K+, Cl-, PO43-, Ca2+.
- 📌 Mnemonic: 'GlAm Bicarb Water Sodi Potass Urea'.
- Key Secretion:
- H+ (via NHE3).
- Organic Acids (e.g., PAH, urate) via OATs.
- Organic Bases (e.g., creatinine) via OCTs.
- Drugs (e.g., penicillin).
⭐ Para-aminohippuric acid (PAH) is actively secreted in PCT; used to measure renal plasma flow as it's almost completely cleared per pass (at low concentrations).
Loop of Henle Hustle - Making Concentrated Gold
The Loop of Henle creates concentrated urine via countercurrent multiplication, establishing medullary hypertonicity. The vasa recta act as countercurrent exchangers, maintaining this gradient.
- Descending Limb:
- Highly permeable to $H_2O$.
- Impermeable to solutes.
- Fluid becomes hypertonic.
- Ascending Limb:
- Impermeable to $H_2O$.
- Solute reabsorption.
- Thin Ascending: Passive $Na^+$ reabsorption.
- Thick Ascending Limb (TAL):
- Reabsorbs ~25% filtered $Na^+$ via $Na^+-K^+-2Cl^-$ (NKCC2) cotransporter.
- 📌 Loop diuretics (Furosemide) act here. 'Loops Lose $Ca^{2+}$'.
- Paracellular $Ca^{2+}/Mg^{2+}$ reabsorption (lumen +ve potential).
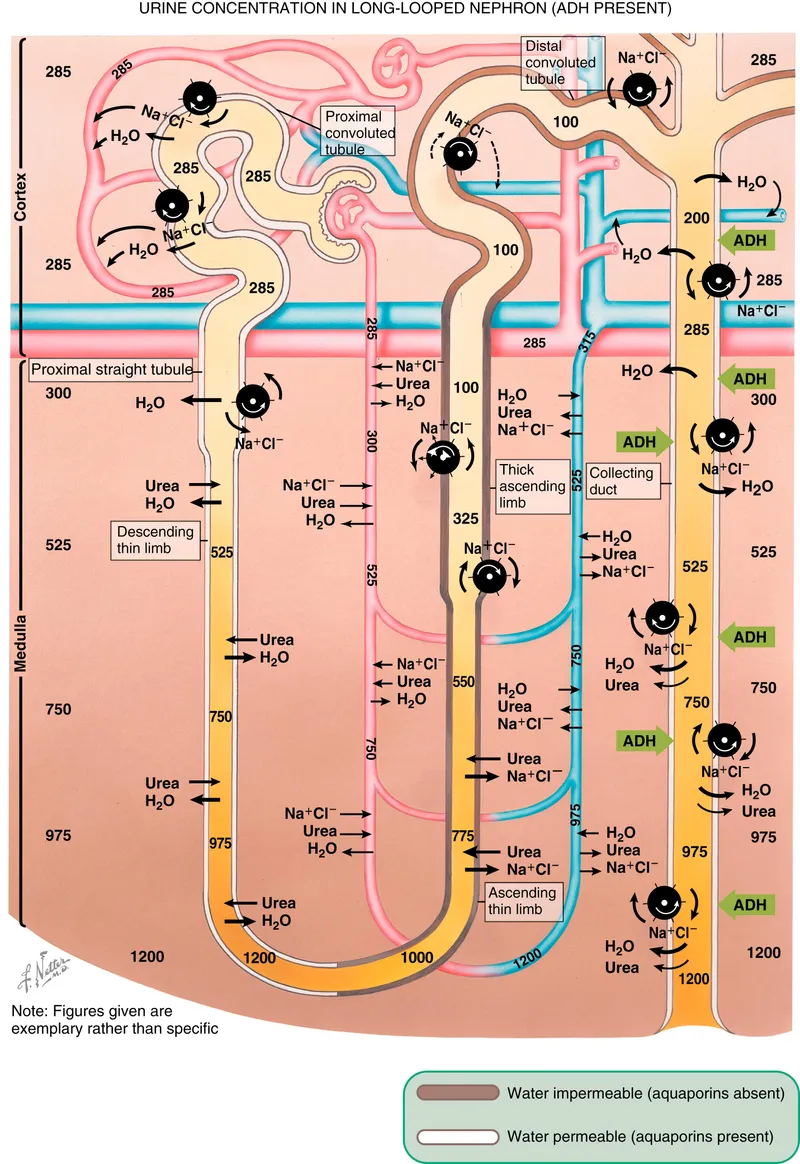
⭐ The thick ascending limb of the Loop of Henle is known as the 'diluting segment' because it reabsorbs solutes without water, making the tubular fluid hypotonic.
Distal Tubule & Collecting Duct - The Fine Tuners
Fine tunes ~5-10% Na+ reabsorption; final urine osmolality 50-1200 mOsm/kg.
- Early Distal Convoluted Tubule (DCT):
- Na+-Cl- cotransporter (NCC): Thiazide sensitive. 📌 Thiazides act on Early DCT.
- Ca2+ reabsorption: TRPV5 (PTH, Vit D regulated).
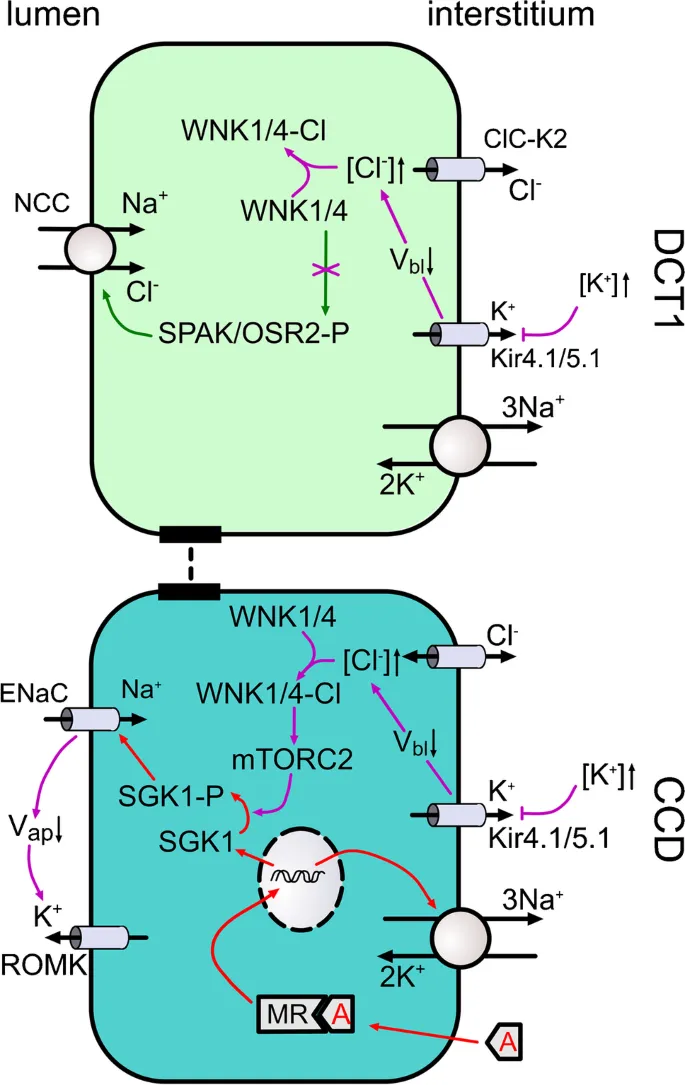
- Late DCT & Collecting Duct (CD):
- Principal Cells:
- Na+ reabsorption: ENaC (Aldosterone ↑). 📌 Aldo saves Sodium, Pushes Potassium out.
- K+ secretion: ROMK/BK (Aldosterone ↑).
- H2O reabsorption: Aquaporin-2 (ADH ↑).
- Intercalated Cells:
- Type A: H+ secretion (H+-ATPase, H+/K+-ATPase), HCO3- & K+ reabsorption.
- Type B: HCO3- secretion, H+ reabsorption.
- Principal Cells:
| Hormone | Target | Action on DCT/CD |
|---|---|---|
| Aldosterone | Principal cells | ↑Na+ reabsorb (ENaC), ↑K+ secrete (ROMK/BK) |
| ADH | Principal cells | ↑H2O reabsorb (Aquaporin-2) |
| ANP | DCT/CD | ↓Na+ reabsorb (inhibits ENaC & Aldo) |
| PTH | Early DCT | ↑Ca2+ reabsorb (TRPV5) |
High‑Yield Points - ⚡ Biggest Takeaways
- PCT is the major site for reabsorption of glucose, amino acids, and HCO3-; it secretes H+ and organic acids/bases.
- The Loop of Henle creates the corticomedullary gradient; its descending limb reabsorbs water, while the ascending limb reabsorbs Na+-K+-2Cl-.
- DCT fine-tunes Na+ and Ca2+ reabsorption; thiazide diuretics act here.
- Collecting Ducts regulate water reabsorption via ADH and Na+/K+ balance via aldosterone.
- Glucose Transport Maximum (Tm) is approximately 375 mg/min; exceeding this leads to glucosuria.
- PAH secretion in the PCT is used to measure Renal Plasma Flow (RPF).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

