TBW & Fluid Spaces - Aqua Realms
- TBW: ~60% body weight (♂), ~50% (♀); ↓ age/obesity.
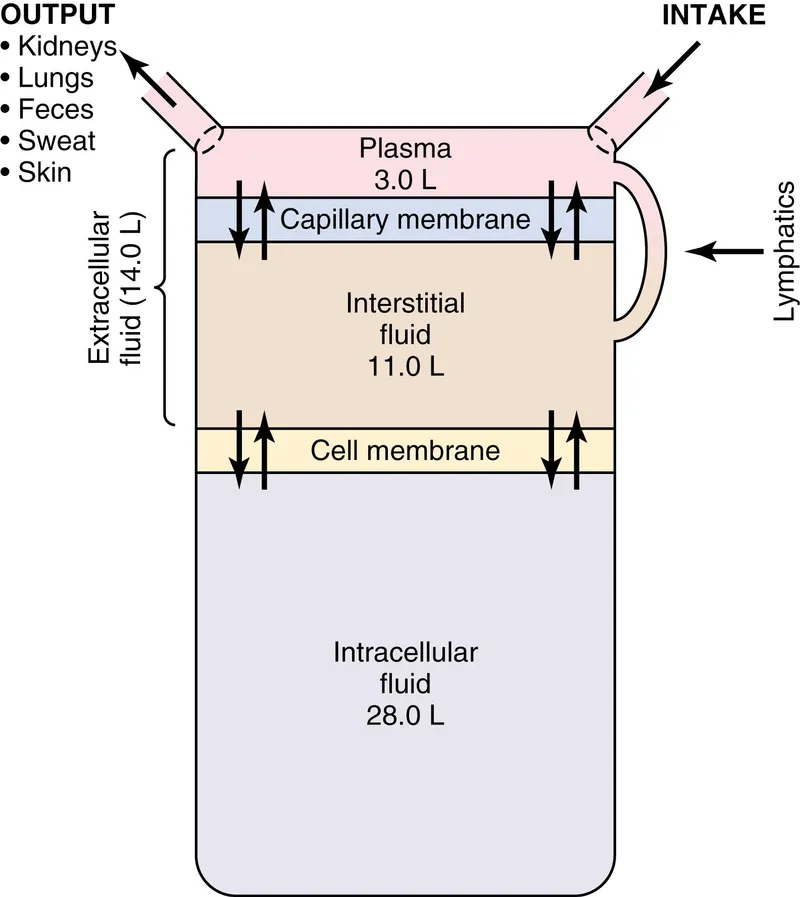
- 📌 60-40-20 Rule (% body wt): TBW 60%, ICF 40%, ECF 20%.
- ICF (2/3 TBW): $K^+$, $PO_4^{3-}$ main ions.
- ECF (1/3 TBW): $Na^+$, $Cl^-$ main ions.
- Plasma: 1/4 ECF.
- ISF: 3/4 ECF.
- Markers: TBW ($D_2O$); ECF (Inulin); Plasma Vol (Evans Blue, $^{131}I$-Alb).
- Derived: ICF = TBW - ECF; ISF = ECF - Plasma.
- Plasma Osmolality: $2[Na^+] + \frac{[Glucose]}{18} + \frac{[BUN]}{2.8}$.
⭐ Normal: 280-295 mOsm/kg $H_2O$. $Na^+$ salts are main ECF osmoles.
Nephron Na$^+$ Handling - Salty Segments
- Proximal Convoluted Tubule (PCT):
- Major site: Reabsorbs ~65-70% filtered Na$^+$.
- Apical: Na$^+$/H$^+$ exchanger (NHE3), SGLT, Na$^+$-Amino Acid, Na$^+$-PO$_4^{3-}$ cotransporters.
- Basolateral: Na$^+$/K$^+$ ATPase.
- Isosmotic reabsorption (water follows Na$^+$).
- Thick Ascending Limb (TAL) - Loop of Henle: Key Diluting Segment
- Reabsorbs ~20-25% filtered Na$^+$.
- Apical: Na$^+$-K$^+$-2Cl$^-$ cotransporter (NKCC2). 📌 NKCC2: "Na K Cl Comes 2gether".
- Basolateral: Na$^+$/K$^+$ ATPase.
- Impermeable to water $ ightarrow$ tubular fluid becomes dilute.
- Generates corticomedullary osmotic gradient.
- Target for Loop Diuretics (e.g., Furosemide).
⭐ Loop diuretics (e.g., Furosemide) inhibit the NKCC2 cotransporter in the TAL, leading to potent natriuresis.
- Distal Convoluted Tubule (DCT) - Early: Diluting Segment
- Reabsorbs ~5-8% filtered Na$^+$.
- Apical: Na$^+$-Cl$^-$ cotransporter (NCC).
- Basolateral: Na$^+$/K$^+$ ATPase.
- Largely impermeable to water.
- Target for Thiazide Diuretics.
- Collecting Duct (Principal Cells):
- Fine-tunes Na$^+$ reabsorption (~2-3%).
- Apical: Epithelial Na$^+$ Channel (ENaC).
- Aldosterone sensitive: $\uparrow$ ENaC & Na$^+$/K$^+$ ATPase activity.
Nephron H₂O Handling & Osmoregulation - Water Works

- Segmental $H_2O$ Reabsorption:
- PCT: ~65-70%; obligatory, iso-osmotic (AQP1). Follows Na⁺.
- Descending LOH: ~15%; freely permeable (AQP1); concentrates tubular fluid.
- Ascending LOH: Impermeable to $H_2O$; diluting segment.
- Late DCT & CD: ~10-20%; facultative, ADH-regulated (AQP2).
- Antidiuretic Hormone (ADH/AVP):
- Source: Hypothalamus (SON/PVN) → Posterior Pituitary.
- Stimuli: ↑ Plasma osmolality (main), ↓ ECF volume.
- Action: V₂ receptors (principal cells) → ↑cAMP → AQP2 insertion (apical) → ↑$H_2O$ reabsorption. 📌 ADH = Adds Da $H_2O$.
- Osmoregulation:
- Maintains plasma osmolality (280-295 mOsm/kg).
- ADH enables urine concentration (max 1200 mOsm/kg) or dilution (min 50 mOsm/kg).
- Requires medullary hypertonicity (countercurrent mechanism).
⭐ Central Diabetes Insipidus (↓ADH) causes excretion of large volumes of dilute urine (Urine Osm < 100-200 mOsm/kg, Sp. Gr. < 1.005), leading to hypernatremia if water intake is inadequate.
Integrated Regulation & Imbalances - Hormonal Harmony & Havoc
Regulators: RAAS, ADH, ANP, SNS.
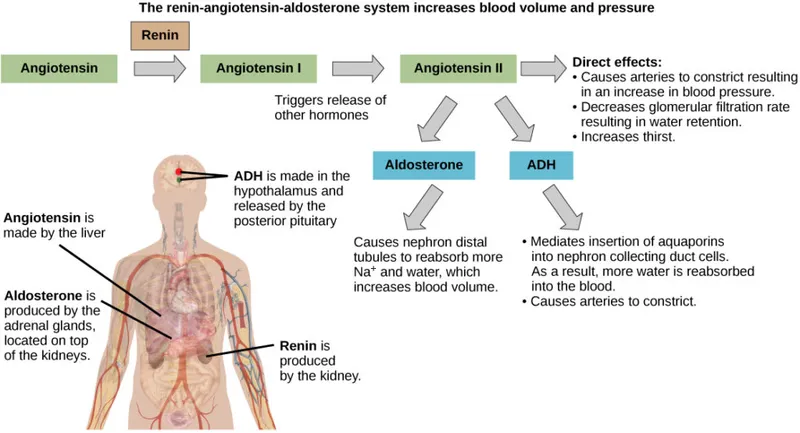
- RAAS: From ↓renal perfusion/↓$Na^+$. AngII (vasoconstriction, ↑$Na^+$ reabsorption) & Aldosterone (↑$Na^+$ reabsorb, $K^+$ secrete).
- ADH (Vasopressin): From ↑Posm/↓volume. ↑$H_2O$ reabsorption (collecting ducts via aquaporins).
- ANP/BNP: From ↑atrial/ventricular stretch. Promotes natriuresis (↑$Na^+$ excretion), diuresis, ↓RAAS.
- SNS: ↑Renin, ↑$Na^+$ reabsorption, renal vasoconstriction.
Imbalances:
- SIADH: ↑ADH → hyponatremia (↓$Na^+$), concentrated urine.
- Diabetes Insipidus (DI): ↓ADH action → hypernatremia (↑$Na^+$), dilute urine.
- Edema: Pathological fluid accumulation.
⭐ SIADH: Urine Osm >100 mOsm/kg & Urine Na+ >40 mEq/L with plasma hyponatremia.
High‑Yield Points - ⚡ Biggest Takeaways
- ADH (Vasopressin) primarily regulates water reabsorption in collecting ducts via aquaporin-2 channels.
- Aldosterone controls sodium reabsorption and K+ secretion in the distal nephron (DCT & CD).
- RAAS activation (due to ↓ renal perfusion) leads to increased Na+ and water retention.
- ANP, released with atrial stretch, promotes natriuresis and diuresis, opposing RAAS.
- Hypothalamic osmoreceptors sense plasma osmolality, influencing ADH release and thirst.
- Effective Circulating Volume (ECV) is the key determinant of RAAS activity, not total body water.
- SIADH causes euvolemic hyponatremia due to excessive water retention and ADH activity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

