Biomarker Fundamentals - Decoding Disease
- Definition: An objectively measured characteristic indicating normal biological processes, pathogenic processes, or therapeutic responses.
- Classification:
- Diagnostic: Detects or confirms disease.
- Prognostic: Predicts disease course/outcome.
- Predictive: Identifies likelihood of response to a specific therapy.
- Pharmacodynamic (PD): Shows a drug's effect on the body.
- Susceptibility/Risk: Indicates predisposition to disease.
- Ideal Characteristics: Sensitive, specific, non-invasive, cost-effective, reproducible, easily measurable. 📌 SNOUT, SPIN.
⭐ An ideal biomarker should be highly sensitive (correctly identifying those with the disease) and highly specific (correctly identifying those without the disease).
Cardiac Biomarkers - Heart's SOS Signals
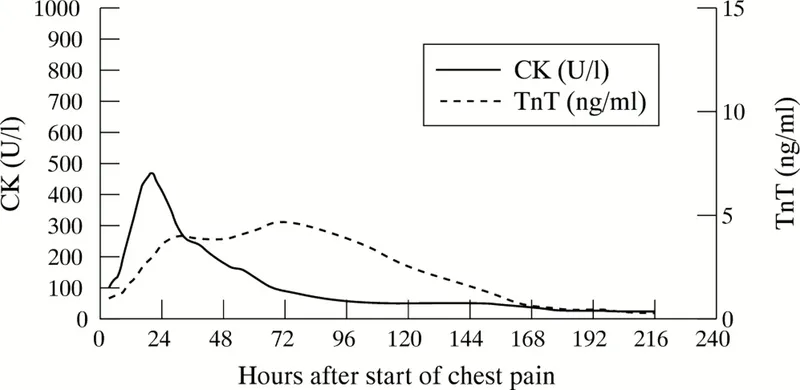
⭐ Cardiac Troponin (cTnI or cTnT) is preferred for MI diagnosis due to high sensitivity/specificity for myocardial injury.
-
Key Biomarkers & Kinetics:
Biomarker Rises (hr) Peaks (hr) Lasts (days) Specificity Troponin I/T 2-4 12-24 7-14 High CK-MB 3-6 12-24 2-3 Moderate 📌 Order of rise (earliest first): Myoglobin, CK-MB, Troponin - "My Cat Trots". -
BNP/NT-proBNP: Heart Failure (HF) diagnosis & prognosis.
- BNP <100 pg/mL: HF unlikely.
- BNP >400 pg/mL: HF likely.
-
hs-CRP (High-sensitivity C-reactive protein): Cardiovascular risk stratification.
- <1 mg/L: Low risk.
- 1-3 mg/L: Average risk.
-
3 mg/L: High risk.
Renal & Hepatic Markers - Filter & Factory Checks
Renal Function (Filter)
| Marker | Significance & Key Values |
|---|---|
| Creatinine | ↓ GFR; 0.6-1.2 mg/dL |
| BUN | ↓ GFR, dehydration; 7-20 mg/dL |
| BUN/Cr Ratio | Prerenal (>20:1), Intrinsic (<10:1) |
| eGFR | GFR (calc. $CKD-EPI, MDRD$); >90 mL/min |
| Cystatin C | GFR (no muscle bias) |
| Microalbuminuria | Diabetic nephropathy (early); 30-300 mg/d |
Hepatic Function (Factory)
| Marker | Significance / Pattern & Key Values/Ratios |
|---|---|
| ALT, AST | Hepatocyte injury. 📌 ALT (Liver), AST (Liver+). Ratio >2 (Alc.) |
| ALP, GGT | Cholestasis |
| Bilirubin | Jaundice (T/D/I). D↑ Obstructive; I↑ Hemolysis |
| Albumin | Synth. fn (↓ chronic); 3.5-5.5 g/dL |
| PT/INR | Synth. fn (↑ severe); INR 0.8-1.2 |
⭐ AST/ALT ratio >2 in alcoholic liver disease; <1 in viral hepatitis/NAFLD.
Metabolic & Inflammatory Markers - Systemic Sentinels
Diabetes Mellitus: Diagnosis (ADA/WHO) 📌 FPG ≥126, HbA1c ≥6.5%, 2-hr PPG/Random ≥200 mg/dL.
| Marker | Value | Notes (Key Info) |
|---|---|---|
| FPG | ≥126 mg/dL | Fasting (≥8-hr) |
| PPG | ≥200 mg/dL | Post 75g OGTT (2-hr) |
| HbA1c | ≥6.5% | ~3-month avg. glucose |
| Random | ≥200 mg/dL | With hyperglycemia sx. |
Inflammatory Markers
- CRP (C-Reactive Protein): Acute-phase reactant, non-specific for inflammation/infection.
- ESR (Erythrocyte Sedimentation Rate): Non-specific; ↑ chronic inflammation, infections, autoimmune.
- Procalcitonin: Differentiates bacterial (>0.5 ng/mL) vs. viral.
- Ferritin: Acute-phase reactant, iron storage. ↑ inflammation, infection.
⭐
HbA1c reflects the average blood glucose concentration over the preceding 2-3 months and is a key marker for long-term glycemic control in diabetic patients.
 টাকেjson
টাকেjson
Tumor Markers - Cancer's Calling Cards
- Tumor markers: Substances indicating cancer.
- Limitations: Not for standalone screening. Used for prognosis, monitoring, recurrence detection.
| Marker | Associated Cancer(s) | Clinical Use |
|---|---|---|
| AFP | HCC, Germ cell | Diagnosis aid, Prognosis, Monitor |
| CEA | Colorectal, Pancreatic, Lung, Breast | Prognosis, Monitor |
| PSA | Prostate | Screening, Monitor |
| CA-125 | Ovarian | Diagnosis aid, Monitor |
| CA 19-9 | Pancreatic, Biliary tract | Diagnosis aid, Prognosis, Monitor |
| hCG | Germ cell, Choriocarcinoma | Diagnosis aid, Prognosis, Monitor |
| CA 15-3 | Breast | Monitoring |
High‑Yield Points - ⚡ Biggest Takeaways
- Biomarkers are objectively measured indicators of biological states or processes.
- Cardiac Troponins (cTnI, cTnT) are gold standard for Myocardial Infarction diagnosis.
- BNP and NT-proBNP are key markers for Heart Failure diagnosis and prognosis.
- HbA1c reflects long-term glycemic control (2-3 months) in diabetes mellitus.
- C-Reactive Protein (CRP) is a highly sensitive marker of acute inflammation and infection.
- Tumor markers like PSA (prostate) and CA-125 (ovarian) aid in cancer management.
- Ideal biomarkers are highly sensitive, specific, non-invasive, and easily measurable.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

