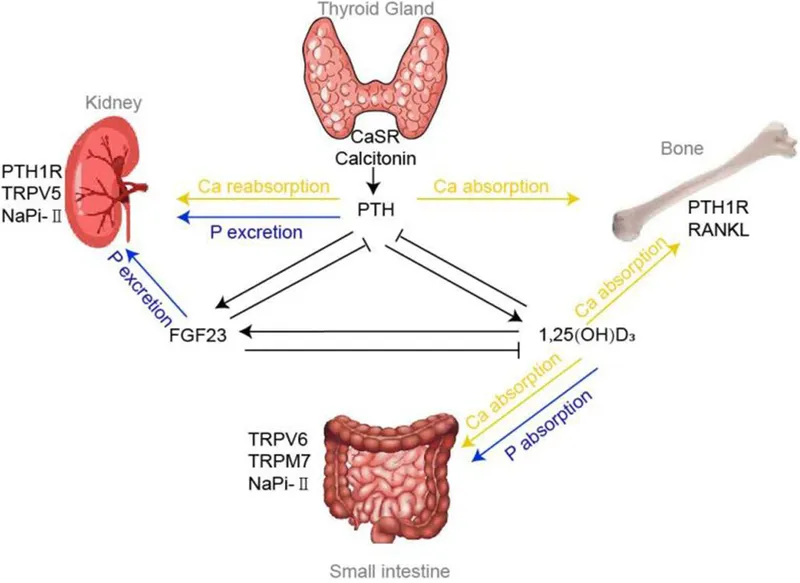
Ca/P Overview - Mineral Dance
- Calcium (Ca²⁺): Total serum ~8.5-10.5 mg/dL (2.1-2.6 mmol/L).
- Forms: Ionized (active, ~50%), protein-bound (~40%), complexed (~10%).
- Functions: Bone, muscle contraction, nerve transmission, clotting.
- Phosphate (PO₄³⁻): Serum ~2.5-4.5 mg/dL (0.8-1.45 mmol/L).
- Functions: Bone, ATP, DNA/RNA, cell membranes, acid-base buffer.
- Key Regulators: PTH, Vitamin D, Calcitonin. FGF-23 (phosphate).
- 📌 Mnemonic: "Calcium Contracts, Phosphate Powers".
- Corrected Ca (low albumin): $Ca_{corrected} = Ca_{measured} + \mathbf{0.8} \times (\mathbf{4} - Albumin)$.
⭐ Ionized Ca²⁺ is biologically active; critical for neuromuscular excitability.
PTH Deep Dive - Bone's Boss
- Source: Parathyroid chief cells.
- Regulation:
- Primary trigger: ↓ Serum Ca²⁺ → ↑ PTH.
- Also: ↑ Serum PO₄³⁻ (indirectly), ↓ Active Vit D → ↑ PTH.
- Mg²⁺: Severe ↓ inhibits; mild ↓ stimulates PTH.
- Actions (Goal: ↑ Serum Ca²⁺, ↓ Serum PO₄³⁻):
- Bone: ↑ Osteoclast activity (via osteoblast RANKL) → ↑ resorption.
- Chronic ↑PTH: catabolic; Intermittent/low dose: anabolic.
- Kidney:
- ↑ Ca²⁺ reabsorption (DCT).
- ↓ PO₄³⁻ reabsorption (PCT) → Phosphaturia (📌 PTH = Phosphate Trashing Hormone).
- ↑ 1α-hydroxylase → ↑ Active Vitamin D.
- Intestine (via ↑ Active Vit D): ↑ Ca²⁺ & PO₄³⁻ absorption.
- Bone: ↑ Osteoclast activity (via osteoblast RANKL) → ↑ resorption.
mechanism of action on bone and kidney)
⭐ PTH significantly decreases phosphate reabsorption in the proximal convoluted tubule (PCT), leading to phosphaturia.
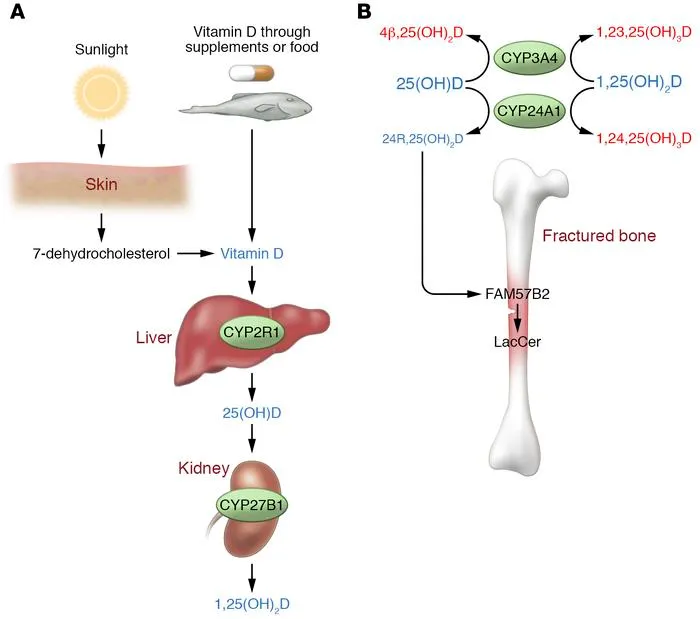
Vitamin D Path - Sunny Side Up
- Sources:
- Skin (UVB): 7-DHC → Vit D3 (Cholecalciferol)
- Diet: Vit D2 (Ergocalciferol), Vit D3 (Cholecalciferol)
- Activation Pathway:
- 1α-hydroxylase Regulation:
- Stimulators: ↑ PTH, ↓ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$
- Inhibitors: ↑ Calcitriol (feedback), ↑ FGF-23, ↑ Serum $Ca^{2+}$, ↑ Serum $PO_4^{3-}$
- Actions of Calcitriol ($1,25-(OH)_2D$):
- Intestine: ↑ $Ca^{2+}$, $PO_4^{3-}$ absorption (primary site)
- Bone: ↑ Mineralization (indirectly), ↑ Resorption (with PTH)
- Kidney: ↑ $Ca^{2+}$, $PO_4^{3-}$ reabsorption
- Parathyroid Gland: ↓ PTH synthesis, secretion
⭐ Calcitriol (1,25-(OH)2D) is the most potent stimulator of intestinal calcium absorption.
Calcitonin & Integration - Cool Down Crew
- Calcitonin: (📌 Calci-TONE-in TONES down $Ca^{2+}$)
- Source: Thyroid parafollicular (C) cells.
- Trigger: ↑ Serum $Ca^{2+}$.
- Actions: Rapidly ↓ serum $Ca^{2+}$ & $PO_4^{3-}$.
- Bone: Inhibits osteoclast activity (↓ resorption).
- Kidney: ↑ $Ca^{2+}$ & $PO_4^{3-}$ excretion.
- Integrated Homeostasis:
- PTH & Vitamin D: Dominant; ↑ $Ca^{2+}$ when levels are low.
- Calcitonin: Opposes PTH; ↓ $Ca^{2+}$ when levels are high. Protects skeleton during $Ca^{2+}$ stress.
⭐ Calcitonin is a useful tumor marker for Medullary Thyroid Carcinoma (MTC).
High‑Yield Points - ⚡ Biggest Takeaways
- PTH ↑ serum Ca²⁺ & ↓ serum PO₄³⁻; stimulates bone resorption, renal Ca²⁺ reabsorption, & 1,25-(OH)₂D₃ synthesis.
- Calcitriol (Active Vitamin D) ↑ intestinal Ca²⁺ & PO₄³⁻ absorption; synergizes with PTH for bone resorption.
- Calcitonin ↓ serum Ca²⁺ by inhibiting osteoclast activity; its physiological role in humans is minor.
- Primary hyperparathyroidism features ↑ PTH, ↑ Ca²⁺, ↓ PO₄³⁻; remember "stones, bones, groans, psychiatric overtones".
- Hypoparathyroidism shows ↓ PTH, ↓ Ca²⁺, ↑ PO₄³⁻; presents with neuromuscular excitability (tetany).
- Vitamin D deficiency leads to ↓ Ca²⁺, ↓ PO₄³⁻, causing secondary hyperparathyroidism (↑ PTH).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more