Body Water & Compartments - Fluid Foundations
- Total Body Water (TBW):
- Adult males: 60%; Females: 50-55%; Infants: 70-75%.
- $TBW (L) \approx \text{Body Wt (kg)} \times 0.6$ (adult male).
- Compartments:
- ICF: 2/3 TBW ($K^+$ major cation).
- ECF: 1/3 TBW ($Na^+$ major cation).
- ISF: 3/4 ECF.
- Plasma: 1/4 ECF.

⭐ TBW measured with D2O, 3H2O; ECF with Inulin; Plasma with Evans Blue. ISF = ECF - Plasma; ICF = TBW - ECF.
Osmolality & Tonicity - Concentration Counts
- Osmolality: Measure of total solute concentration in a fluid.
- Plasma Osmolality $≈ 2 \times [Na⁺] + [Glucose]/18 + [BUN]/2.8$
- Normal range: 280‑295 mOsm/kg.
- Tonicity: Effective osmolality; determines water movement across cell membranes due to impermeable solutes.
- Isotonic: No net water movement; cell volume unchanged.
- Hypotonic: Water enters cell → cell swells.
- Hypertonic: Water exits cell → cell shrinks.
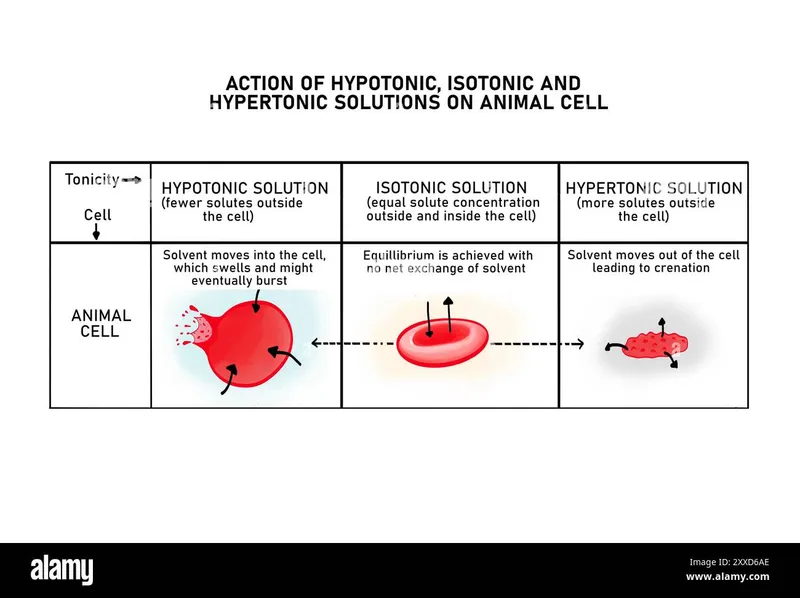
⭐ Sodium and its accompanying anions (Cl⁻, HCO₃⁻) account for ~90% of ECF osmolality, making it the primary determinant of ECF volume and water distribution between ECF and ICF.
Sodium Homeostasis - Salty Sovereignty
- $Na^+$: Primary ECF cation; dictates ECF volume & osmolality. Daily intake: 3-5g.
- Regulation: Kidneys precisely manage $Na^+$ excretion.
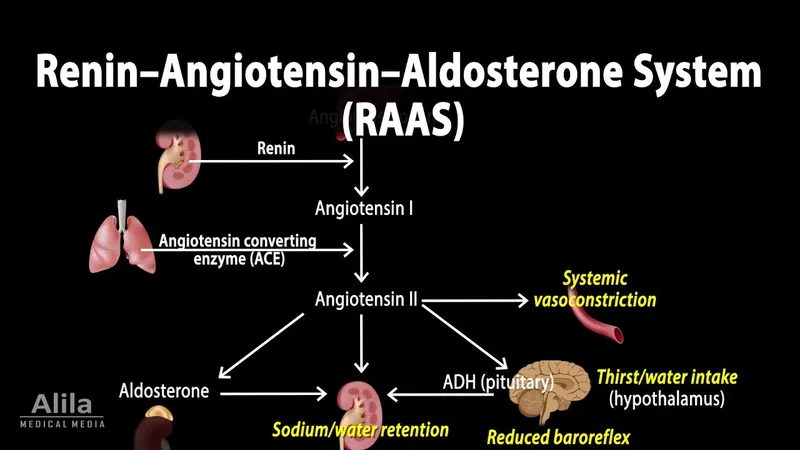
- RAAS: Renin → Ang I → Ang II (ACE) → Aldosterone. 📌 (Remember: R-A-A-A sequence)
- Angiotensin II: Vasoconstriction, ↑Aldosterone, ↑ADH, ↑Thirst.
- Aldosterone: ↑$Na^+$ reabsorption (late Distal Tubule & Collecting Duct), ↑$K^+$ excretion. Water passively follows $Na^+$.
- Natriuretic Peptides (ANP, BNP): Counter RAAS; promote $Na^+$ excretion.
- RAAS: Renin → Ang I → Ang II (ACE) → Aldosterone. 📌 (Remember: R-A-A-A sequence)
- ECV sensors: Carotid/aortic baroreceptors, juxtaglomerular apparatus (macula densa).
⭐ Aldosterone primarily acts on the principal cells of the late distal tubule and collecting duct, increasing ENaC and $Na^+$/$K^+$-ATPase activity.
Water Homeostasis - Aqua Guardians
- Key regulator: Antidiuretic Hormone (ADH)/Vasopressin.
- ADH release stimuli:
- ↑Plasma osmolality (osmoreceptors; threshold ~280 mOsm/kg).
- ↓Blood volume/pressure (baroreceptors).
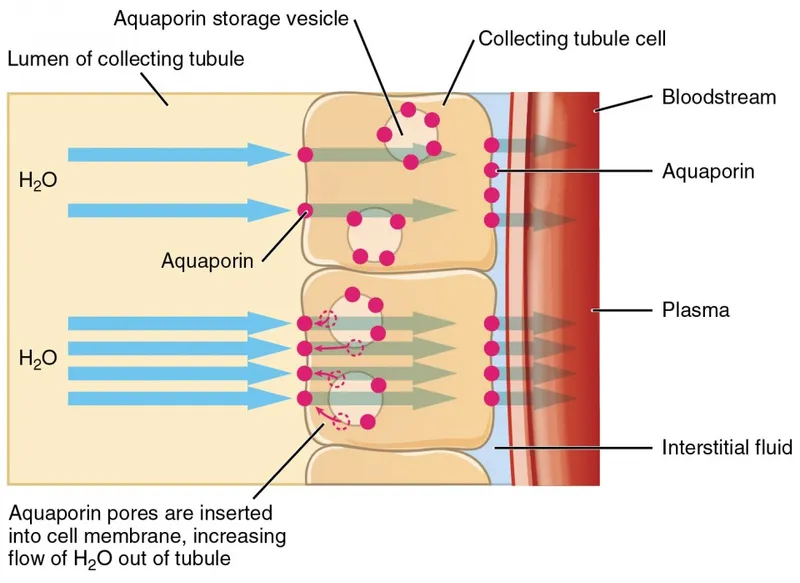
- ADH action: ↑Water permeability in renal collecting ducts (AQP2 insertion) → ↑Water reabsorption → Concentrated urine.
- 📌 ADH: "Adds Da H₂O" (to body).
⭐ Osmoreceptors for ADH release are in the supraoptic & paraventricular nuclei of the hypothalamus.
Sodium Imbalances - Na‑sty Situations
Hyponatremia: Na+ <135. Severe: <125 mEq/L. Max correction 8-10 mEq/L/24h. Na+ Deficit: $TBW \times (Desired Na^+ - Measured Na^+)$.
⭐ Rapid correction of chronic hyponatremia (<125 mEq/L) can lead to osmotic demyelination syndrome (ODS).
Hyponatremia Types:
| Type | Vol | Key (UNa) |
|---|---|---|
| Hypovolemic | ↓ | Losses (<20/>20) |
| Euvolemic | ↔ | SIADH (>20) |
| Hypervolemic | ↑ | Overload (CHF, Cirrhosis; <20) |
Hypernatremia (>145 mEq/L): Water loss/Na+ gain. 📌 6 D's (Diuresis, Dehydration, DI).
Water Imbalances - H2O Woes
- 📌 SIADH: Sodium Is Always Down Here.
- 📌 DI: Dry Inside (polyuria, polydipsia).
| Condition | ADH | $S_{Na+}$ | $U_{Osm}$ vs $P_{Osm}$ | $P_{Osm}$ | Desmopressin Effect |
|---|---|---|---|---|---|
| SIADH | ↑ | ↓ | ↑(>100) despite ↓$P_{Osm}$ | ↓ | Worsens hypoNa+ |
| Central DI | ↓ | N/↑ | ↓(<300) | ↑ | $U_{Osm}$ ↑ >50% |
| Nephrogenic DI | N/↑(R) | N/↑ | ↓(<300) | ↑ | No/Min $U_{Osm}$ ↑ |
Diagnostic Approach to Polyuria:
High‑Yield Points - ⚡ Biggest Takeaways
- TBW is ~60% body weight; ICF 2/3, ECF 1/3. Na+ is main ECF cation.
- Plasma osmolality (280-295 mOsm/kg) reflects Na+; regulated by ADH (water balance).
- Aldosterone (RAAS) ↑Na+ reabsorption (water follows), ↑K+ secretion; regulates ECF volume.
- Hyponatremia: classify by volume. SIADH → euvolemic hyponatremia.
- Hypernatremia: usually free water deficit (impaired thirst, Diabetes Insipidus).
- Effective Circulating Volume (ECV), not total ECF, drives Na+ and volume regulation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

