Magnesium: Basics & Distribution - Mighty Mineral Intro
- Total body Mg:
25g (1000 mmol). - Distribution:
- Bone: ~60%
- Intracellular (muscle, soft tissues): ~39%
- Extracellular Fluid (ECF): ~1%
- Dietary sources: Green leafy vegetables, nuts, whole grains.
- Daily requirement: ~300-400 mg.
⭐ Magnesium is the second most abundant intracellular cation after potassium, with normal serum levels around 1.7-2.2 mg/dL (0.7-0.9 mmol/L).
Magnesium: Absorption & Excretion - In, Out, Regulated
- Absorption (Intestine):
- Jejunum & ileum (main sites).
- Paracellular (passive, major) & transcellular (active, TRPM6/7).
- ↑ by Vit D; ↓ by phytates, high Ca/PO4.
- Excretion (Kidneys):
- Filtered, then reabsorbed.
- Proximal Convoluted Tubule (PCT): 15-20%.
- Thick Ascending Limb (TAL): 60-70% (major).
- Distal Convoluted Tubule (DCT): 5-10% (active, TRPM6).
- ↑ excretion: Loop/thiazide diuretics, hypercalcemia.
⭐ The thick ascending limb (TAL) of the loop of Henle is the major site for renal magnesium reabsorption (60-70%), followed by the proximal convoluted tubule (15-20%).
oka
Magnesium: Key Functions - Cellular Powerhouse
- Vital intracellular cation.
- Cofactor for >300 enzymes:
- Energy (ATP) metabolism: Kinases, ATPases.
- DNA/RNA synthesis & stability.
- Nerve conduction, muscle function (Ca²⁺ channel blocker).
- Maintains cardiac rhythm.
- Blood glucose control.
⭐ Magnesium is a crucial cofactor for over 300 enzymes, particularly those involving ATP metabolism (e.g., kinases) and nucleic acid synthesis.
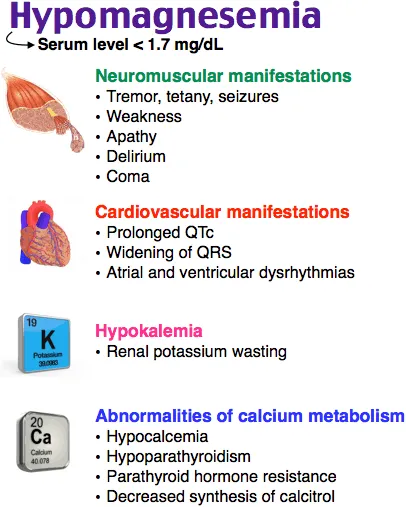
Hypomagnesemia: Causes & Care - Deficiency Dangers
- Definition: Serum Mg < 1.8 mg/dL (or < 0.7 mmol/L).
- Causes:
- ↓ Intake/Absorption: Malnutrition, alcoholism, PPIs, malabsorption (Crohn's).
- ↑ Renal Loss: Diuretics (loop/thiazide), Gitelman/Bartter, nephrotoxins.
- GI Losses: Diarrhea, vomiting.
- Redistribution: Refeeding syndrome.
- Clinical Features (Dangers):
- Neuromuscular: Weakness, tremors, tetany (Chvostek's/Trousseau's +ve), seizures.
- Cardiac: Arrhythmias (Torsades de Pointes), ECG: ↑PR, ↑QT intervals.
- ⭐ > Hypomagnesemia is a critical cause of refractory hypokalemia (due to increased renal potassium wasting via ROMK channels) and hypocalcemia (due to impaired PTH secretion and end-organ resistance).
- Management (Care):
- Treat underlying cause.
- Oral Mg (mild/asymptomatic).
- IV MgSO₄ (severe/symptomatic): Torsades 1-2g IV; Seizures 1-2g IV.
- Monitor DTRs, respiratory rate, urine output.
Hypermagnesemia: Causes & Care - Toxicity Troubles
Causes:
- ↓ Renal Excretion: Acute Kidney Injury (AKI), Chronic Kidney Disease (CKD) (most common).
- ↑ Exogenous Intake:
- Iatrogenic: IV MgSO₄ (eclampsia, asthma).
- Oral: Mg-antacids/laxatives (esp. with CKD).
- Other: Lithium, hypothyroidism, Addison's, tumor lysis.
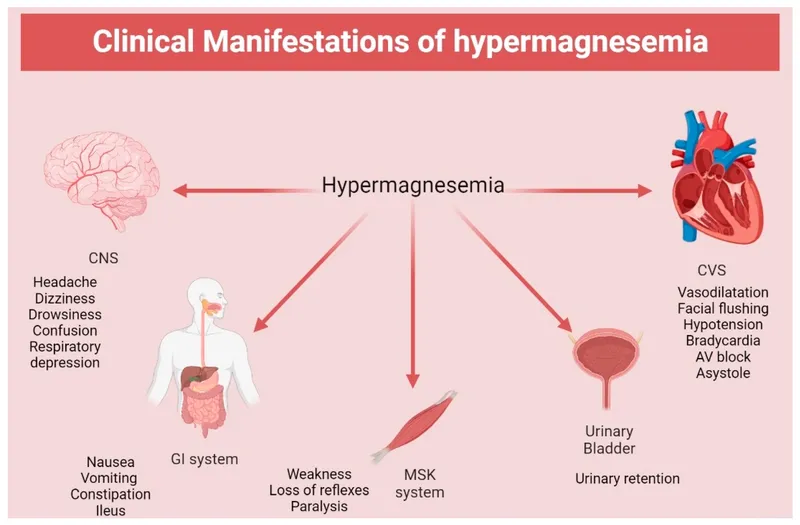
Clinical Manifestations:
- Neuromuscular:
- 4-7 mEq/L: ↓DTRs (earliest sign), muscle weakness, lethargy.
⭐ The earliest sign of hypermagnesemia is often the loss of deep tendon reflexes (DTRs), typically occurring at Mg levels of 4-7 mEq/L.
- 7-10 mEq/L: Areflexia, somnolence.
- >10-12 mEq/L: Flaccid paralysis, respiratory depression.
- Cardiovascular:
- Hypotension, bradycardia.
- ECG: ↑PR interval, ↑QRS duration, ↑QT interval, AV block.
- Cardiac arrest (>15 mEq/L).
- Other: Nausea, vomiting, flushing.
Management:
- Stop all Mg intake.
- Antagonism: IV Calcium Gluconate (10-20ml of 10% solution).
- Enhance Elimination:
- IV Saline + Furosemide.
- Hemodialysis (HD) for severe cases or renal failure.
- Supportive: Mechanical ventilation.
High‑Yield Points - ⚡ Biggest Takeaways
- Normal serum Mg²⁺: 1.7-2.2 mg/dL.
- Crucial cofactor for ATP-dependent enzymes; modulates neuromuscular excitability and cardiac function.
- Absorption: Jejunum & ileum; Excretion: Renal, mainly via TAL & DCT reabsorption.
- Hypomagnesemia: Neuromuscular hyperexcitability (tetany, Torsades), hypokalemia, hypocalcemia. Caused by diuretics, PPIs, alcohol.
- Hypermagnesemia: Due to renal failure or excess intake. Leads to neuromuscular depression (↓DTRs), hypotension, bradycardia.
- Treat severe hypermagnesemia with IV Calcium gluconate for cardiac protection.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

