Overview & Protein Types - Gatekeepers Galore
Integral proteins regulating solute passage across membranes. Crucial for cell function. 📌 Channels, Carriers, Pumps: Key transport mechanisms.
- Main Types:
- Channels: Pores for rapid, passive ion/water flow. E.g., aquaporins, ion channels (Na+, K+).
- Gating: Voltage, ligand, mechanical.
- Carriers: Bind solute, conformational change. Slower.
- Uniporters, Symporters, Antiporters.
- Pumps: Active transport via ATP hydrolysis. E.g., Na+/K+ ATPase.
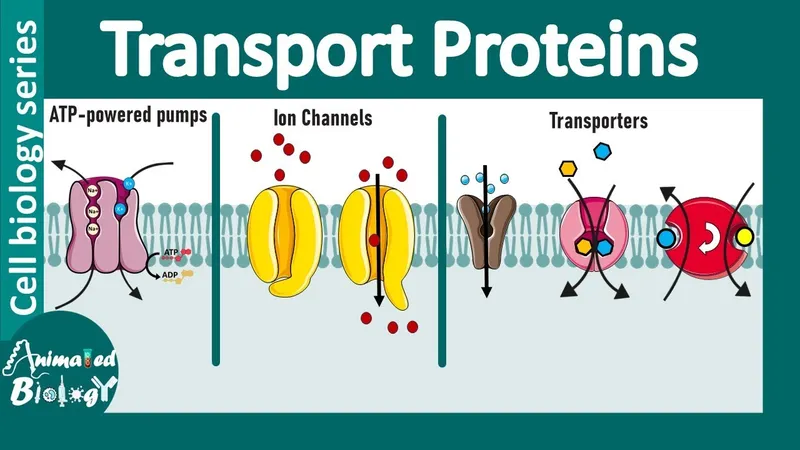
- Channels: Pores for rapid, passive ion/water flow. E.g., aquaporins, ion channels (Na+, K+).
⭐ Carrier proteins, like GLUTs, show saturation kinetics, a key feature distinguishing them from simple diffusion and channel-mediated transport_api.json(markdown=
Channel Proteins - Speedy Tunnels
- Form selective, hydrophilic pores for rapid passive transport.
- Move ions (e.g., $Na^+$, $K^+$, $Ca^{2+}$, $Cl^-$) down electrochemical gradient; speed: 10^7-10^8 ions/sec.
- Key types by gating mechanism:
- Voltage-gated: Open/close by Vm changes (e.g., neuronal $Na^+$ channels).
- Ligand-gated: Activated by ligand binding (e.g., nAChR).
- Mechanosensitive: Respond to physical deformation (touch, sound).
- Non-gated (Leak channels): Persistently open; RMP role (e.g., $K^+$ leak channels).
⭐ > Cystic Fibrosis results from mutations in CFTR, an ATP-gated $Cl^-$ channel, affecting epithelial transport.
 oka
oka
Carrier Proteins - Picky Packers
- Bind specific solutes; undergo reversible conformational changes for membrane translocation. Slower than ion channels.
- Exhibit saturation kinetics: $V_{max}$ (max transport rate) & $K_m$ (substrate affinity).
- Facilitated Diffusion: Passive, down electrochemical gradient; no direct ATP.
- Uniporter: 1 solute (e.g., GLUT1).
- Symporter: 2 solutes, same direction (e.g., SGLT1 - Na+/Glucose).
- Antiporter: 2 solutes, opposite (e.g., Na+/Ca2+ exchanger).
- 📌 Carriers CARRY, Change, Capped (saturated).
⭐ GLUT4 (muscle, adipose tissue) is insulin-dependent. Insulin promotes its translocation to the plasma membrane, boosting glucose uptake.
Active Transport - Uphill Battles
- Moves solutes against electrochemical gradient; requires energy (ATP).
- Primary Active Transport (PAT): Direct ATP use.
- $Na^+$/$K^+$ ATPase: Pumps 3 $Na^+$ out, 2 $K^+$ in.
- $Ca^{2+}$ ATPase (SERCA, PMCA): Pumps $Ca^{2+}$ out/into SR.
- $H^+$/$K^+$ ATPase: Proton pump (e.g., stomach).
- Secondary Active Transport (SAT): Uses ion gradient (from PAT).
- Symport (Cotransport): Solute + ion, same direction (e.g., SGLT1: $Na^+$-glucose).
- Antiport (Counter-transport): Solute + ion, opposite directions (e.g., NCX: $Na^+$/$Ca^{2+}$).

⭐ Digoxin inhibits Na+/K+ ATPase, ↑ intracellular Na+, ↓ Na+/Ca2+ exchange, ↑ intracellular Ca2+, ↑ cardiac contractility.
Clinical Connections - Gates Gone Wrong
- Channelopathies: Genetic disorders of ion channels, affecting cellular excitability.
- Cystic Fibrosis (CF): Defective CFTR ($Cl⁻$ channel) → viscous secretions.
- Autosomal recessive. Commonest lethal genetic disease in Caucasians.
- Long QT Syndromes (LQTS): Cardiac $K⁺$/$Na⁺$ channel defects → arrhythmias, syncope.
⭐ Romano-Ward (AD, pure cardiac) & Jervell and Lange-Nielsen (AR, +deafness) are key LQTS types.
- Periodic Paralysis: Muscle $Na⁺$/$Ca²⁺$/$K⁺$ channel defects → episodic weakness.
- E.g., Hypokalemic, Hyperkalemic types.
High‑Yield Points - ⚡ Biggest Takeaways
- Facilitated diffusion (e.g., GLUTs) is passive, saturable, and specific, using carrier/channel proteins.
- Active transport requires ATP to move solutes against concentration gradients.
- Na+/K+ ATPase (3 Na+ out, 2 K+ in) is a crucial primary active transporter.
- Secondary active transport (e.g., SGLT1) utilizes ion gradients from primary pumps.
- Ion channels (voltage-gated, ligand-gated, mechanically-gated) exhibit high selectivity.
- CFTR, an ABC transporter, is vital; its defects cause cystic fibrosis.
- Aquaporins facilitate rapid water transport across membranes an_d are highly specific for water molecules_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

