Venous Return & CVP Basics - Blood's Journey Home
- Venous Return (VR): Total volume of blood flowing from systemic veins into the right atrium per minute.
- Major determinant of End-Diastolic Volume (EDV) and thus Cardiac Output (CO) via Frank-Starling law.
- Central Venous Pressure (CVP): Hydrostatic pressure within the thoracic vena cava, near the right atrium; reflects Right Atrial Pressure (RAP).
- Normal range: 2-8 mmHg.
- Key indicator of right ventricular preload and intravascular volume status.
⭐ CVP measurement is crucial for assessing right ventricular function and guiding fluid resuscitation in critically ill patients, reflecting right heart filling pressure and volume status effectively a surrogate for preload for the right ventricle
Venous Return Drivers - Pushing Blood Uphill
- Primary Driver: Pressure Gradient ($P_{msf} - P_{RA}$)
- $P_{msf}$ (Mean Systemic Filling Pressure): ~7 mmHg. Reflects blood volume, vascular tone.
- $P_{RA}$ (Right Atrial Pressure/CVP): 0-5 mmHg. Impedance to VR.
- Assisting Pumps & Factors:
- Muscle Pump: Skeletal muscle contraction + one-way valves propel blood towards heart.

- Respiratory Pump: Inspiration → ↓ intrathoracic pressure, ↑ intra-abdominal pressure → aids venous flow to thorax.
- Venous Tone: Sympathetic stimulation → venoconstriction → ↑ $P_{msf}$ → ↑ VR.
- Cardiac Suction: Ventricular contraction (AV valve descent) & diastolic relaxation create suction effect, ↓ $P_{RA}$.
- Blood Volume: ↑ Blood volume → ↑ $P_{msf}$ → ↑ VR.
- Muscle Pump: Skeletal muscle contraction + one-way valves propel blood towards heart.
- Opposing Factor:
- Gravity: Tends to pool blood in dependent veins; countered by muscle/respiratory pumps & venous valves.
⭐ The respiratory pump's contribution to venous return is most significant during deep inspiration or increased respiratory effort, such as during exercise.
CVP Unveiled - Heart's Welcome Mat
- Central Venous Pressure (CVP) reflects right atrial pressure (RAP), indicating RV preload & volume status.
- Measurement: Central line (tip SVC/RA); transducer at phlebostatic axis (4th ICS, mid-axillary).
- Normal: 2-6 mmHg (3-8 cm H₂O).
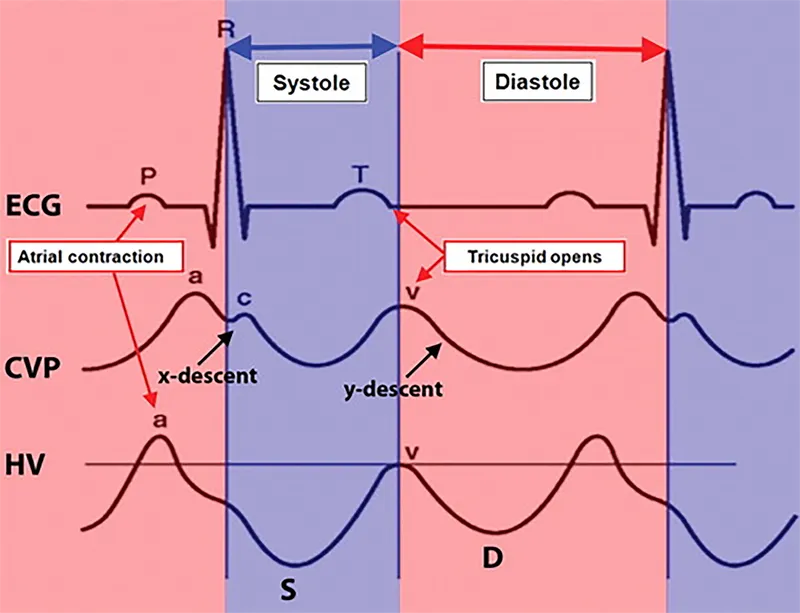
- CVP Waveform: 📌 Apple Cider Xtra Velvet Yummy
- a wave: Atrial contraction (absent in AFib).
- c wave: Tricuspid bulge (ventricular systole).
- x descent: Atrial relaxation, RV downward pull.
- v wave: Atrial venous filling (tricuspid closed).
- y descent: Tricuspid opens, early ventricular fill.
- Factors ↑ CVP: Hypervolemia, RV failure, tamponade, PEEP, tricuspid stenosis/regurg.
- Factors ↓ CVP: Hypovolemia, vasodilation (sepsis).
⭐ Cannon 'a' waves: Large 'a' waves from atrial contraction against closed tricuspid valve (e.g., complete heart block, VTach).
Clinical Tie-Ins - When Flow Goes Wrong
- ↓ VR / ↓ CVP (CVP < 2 mmHg):
- Causes: Hemorrhage, dehydration, vasodilation (e.g., sepsis).
- Signs: Hypotension, tachycardia, collapsed neck veins, ↓ preload.
- ↑ VR / ↑ CVP (CVP > 8 mmHg):
- Causes: Right heart failure, fluid overload.
- Signs: JVD, edema, ascites, hepatomegaly.
- Impaired VR (Obstruction):
- Cardiac Tamponade:
⭐ Beck's Triad: Hypotension, JVD, Muffled Heart Sounds.
- Pulsus paradoxus (>10 mmHg ↓ SBP on inspiration).
- Tension Pneumothorax: ↑ intrathoracic pressure → ↓VR; tracheal deviation.
- SVC Syndrome: Facial/arm swelling, JVD.
- Constrictive Pericarditis: Kussmaul's sign (JVP ↑ on inspiration).
- Cardiac Tamponade:
High‑Yield Points - ⚡ Biggest Takeaways
- Venous Return (VR): crucial blood flow to right atrium; primarily driven by Mean Systemic Filling Pressure (MSFP).
- Central Venous Pressure (CVP) or Right Atrial Pressure (RAP) opposes VR; normal CVP is 0-8 mmHg.
- Key determinant: VR = (MSFP - RAP) / RVR (Resistance to Venous Return).
- Factors ↑VR: ↑blood volume, venoconstriction, skeletal muscle pump, respiratory pump.
- Factors ↓VR: ↓blood volume, venodilation, ↑RAP (e.g., heart failure, tamponade).
- CVP clinically reflects right ventricular preload and intravascular volume status.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

