Baroreceptor Reflex - Pressure Patrol
- Receptors: Stretch-sensitive mechanoreceptors.
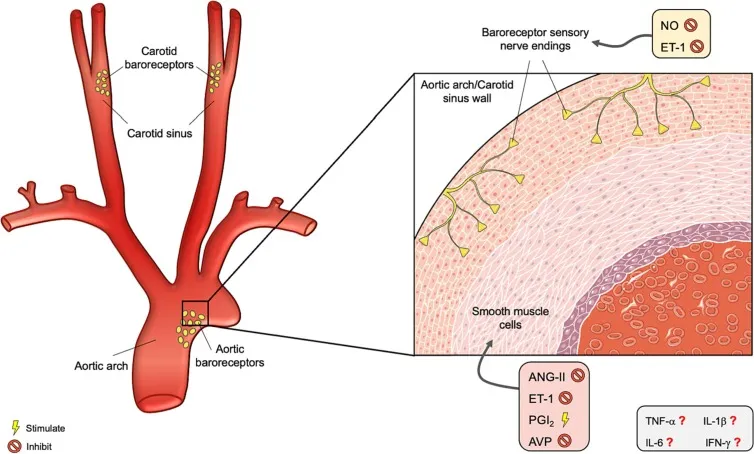
- Carotid Sinus (afferent: CN IX - Hering's nerve): Responds to ↑ & ↓ BP. More sensitive, operates at lower pressures.
- Aortic Arch (afferent: CN X): Responds primarily to ↑ BP. Higher threshold pressure.
- Central Integration: Afferents project to Nucleus Tractus Solitarius (NTS) in the medulla.
- Efferent Response & Effect:
- If BP ↑:
- NTS excites vagal nuclei (↑ parasympathetic) & inhibits vasomotor center (↓ sympathetic).
- Result: ↓ Heart Rate, ↓ Contractility, Vasodilation (↓ Total Peripheral Resistance) → ↓BP.
- If BP ↓:
- ↓Baroreceptor firing → NTS disinhibition of vasomotor center (↑ sympathetic) & inhibition of vagal nuclei (↓ parasympathetic).
- Result: ↑ Heart Rate, ↑ Contractility, Vasoconstriction (↑ TPR) → ↑BP.
- If BP ↑:
- Function: Rapid, moment-to-moment negative feedback regulation of arterial BP. Buffers acute BP fluctuations (e.g., posture changes).
⭐ Baroreceptors adapt (reset) to sustained changes in BP (e.g., chronic hypertension) over 1-2 days, making them less effective for long-term BP control.
📌 Mnemonic: "Pressure Patrol" - Baroreceptors Patrol blood Pressure levels, initiating rapid adjustments.
Chemoreceptor Reflex - Gas Gauge Guardians
- Function: Monitors blood chemistry ($P_{O2}$, $P_{CO2}$, pH); modulates cardiorespiratory activity to maintain homeostasis.
- Sensors (Chemoreceptors):
- Peripheral:
- Carotid Bodies (carotid bifurcation): Key for hypoxia. Stimuli: ↓ $P_{O2}$ (< 60 mmHg), ↑ $P_{CO2}$, ↑ $[H^+]$. Afferent: CN IX.
- Aortic Bodies (aortic arch): Stimuli: similar. Afferent: CN X.
- Central:
- Medulla oblongata: Main sensor for $CO_2$. Stimuli: ↑ $P_{CO2}$ (via CSF $[H^+]$).
- Peripheral:
- Response (to Hypoxia/Hypercapnia/Acidosis):
- ↑ Sympathetic drive → widespread vasoconstriction (except brain/heart), ↑ TPR, ↑ BP.
- ↑ Respiration (dominant effect, aims to correct gas imbalance).
- Initial vagal bradycardia, often overridden by lung reflexes or direct sympathetic effects.
⭐ Peripheral chemoreceptors are the only significant reflex mechanism responding to arterial hypoxemia.
Atrial & Low-Pressure Reflexes - Volume Vigilantes
- Receptors: Low-pressure (volume) receptors in atria, pulmonary vessels.
- Stimulus: ↑ Blood volume → atrial stretch.
- Afferent: Vagus (CN X).
- Goal: Regulate ECF volume.
- Responses to ↑ Volume:
- ↓ ADH → ↑ diuresis.
- ↑ ANP (atria):
- Natriuresis, diuresis.
- Vasodilation.
- Inhibits RAAS.
- Renal vasodilation, ↓ renal sympathetic tone → ↑ Na+/water excretion.
- Bainbridge Reflex: ↑ Heart rate with ↑ atrial filling.
⭐ ANP is released from atrial myocytes in response to stretch, promoting vasodilation and excretion of sodium and water.
Special Reflexes & Maneuvers - Situational Savers
- Valsalva Maneuver: Forced expiration. 4 phases impact BP/HR. Tests autonomic function; can terminate SVTs.
- Carotid Sinus Massage (CSM): Stimulates baroreceptors → ↑vagal tone → ↓HR. For PSVT. ⚠️ Check for bruits.
- Oculocardiac Reflex (Aschner's): Eyeball pressure → ↓HR. Afferent: CN V, Efferent: CN X.
- Bainbridge (Atrial) Reflex: ↑Venous return (atrial stretch) → ↑HR.
- Bezold-Jarisch Reflex: LV receptor stimulation (e.g., inferior MI) → Hypotension, Bradycardia, Apnea.
Cushing Reflex Pathway:
⭐ Cushing reflex (Hypertension, Bradycardia, Irregular Respiration) is a late sign of severely ↑ICP, often indicating impending brain herniation.
High‑Yield Points - ⚡ Biggest Takeaways
- Baroreceptors (carotid sinus/aortic arch): Key for short-term BP control; ↑BP → ↓HR, vasodilation.
- Peripheral chemoreceptors: Respond to ↓PaO₂, ↑PaCO₂, ↓pH → ↑BP, ↑ventilation.
- Bainbridge reflex: ↑atrial stretch (↑venous return) → ↑HR.
- Cushing reflex (↑ICP): Triad of hypertension, bradycardia, irregular respiration.
- Bezold-Jarisch reflex: Coronary/ventricular stimuli → hypotension, bradycardia.
- Valsalva maneuver: Tests autonomic function. Phase II: ↓BP, ↑HR. Phase IV: ↑BP, ↓HR.
- Oculocardiac reflex: Globe pressure → bradycardia (CN V afferent, CN X efferent).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

