Cardiac Output: The Basics - Heart's Vital Stats
- Cardiac Output (CO): Blood pumped/ventricle/min; ~5-6 L/min.
- Formula: $CO = HR \times SV$.
- Stroke Volume (SV): Blood pumped/beat; ~70-80 mL.
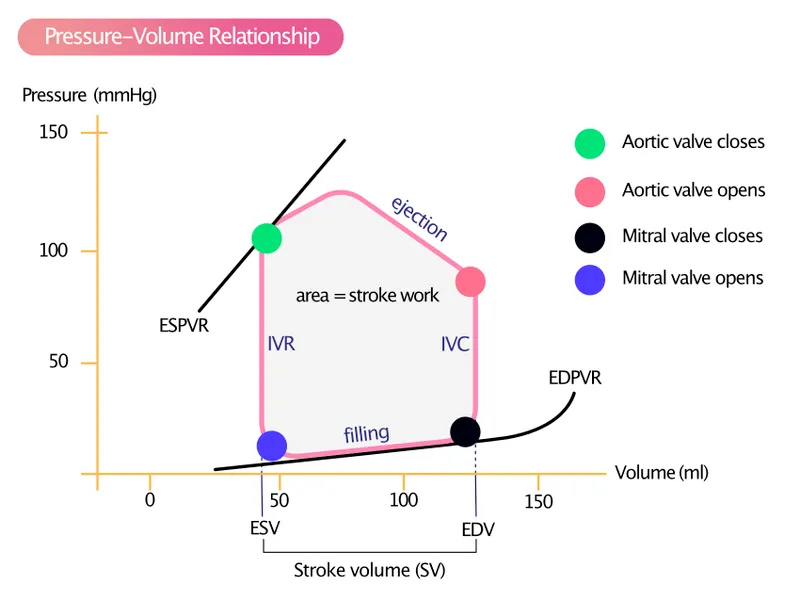
- Formula: $SV = EDV - ESV$.
- Cardiac Index (CI): CO/Body Surface Area (BSA); ~2.5-4.2 L/min/m².
- Formula: $CI = CO / BSA$.
- Ejection Fraction (EF): Percentage of End Diastolic Volume (EDV) ejected per beat; normally 55-70%.
- Formula: $EF = (SV / EDV) \times 100%$.
⭐ EF is a crucial measure of left ventricular function; values < 40% suggest systolic dysfunction/heart failure.

Heart Rate Regulation - The Cardiac Conductor
- Pacemaker: SA node (intrinsic rate 60-100 bpm). Highest discharge frequency.
- Autonomic Control (ANS):
- Sympathetic (SNS): Norepinephrine (NE) on β1 receptors → ↑HR, ↑conduction (+ve chronotropy & dromotropy).
- Parasympathetic (PNS - Vagus): Acetylcholine (ACh) on M2 receptors → ↓HR, ↓conduction (-ve chronotropy & dromotropy).
⭐ Vagal tone predominates at rest, keeping resting HR ~70 bpm (vs. SA intrinsic ~100 bpm).
- Hormonal:
- Adrenaline (β1): ↑HR.
- Thyroid hormones (T3/T4): ↑HR (↑β1 receptor sensitivity).
- Other Factors:
- Temperature: ↑Temp → ↑HR.
- Ions: K+ (HyperK+ ↓HR); Ca2+ (HyperCa2+ ↑HR).
- Bainbridge Reflex: ↑Venous return → ↑Atrial stretch → ↑HR.

Stroke Volume Regulation - The Ventricular Trio
- Preload: Ventricular stretch at end-diastole (EDV).
- Frank-Starling Mechanism: ↑Preload → ↑SV (optimal myofilament overlap).
- Factors: Venous return (volume status, venoconstriction, muscle/respiratory pumps).
- Afterload: Force opposing ventricular ejection.
- LV: Aortic pressure, Systemic Vascular Resistance (SVR).
- RV: Pulmonary artery pressure, Pulmonary Vascular Resistance (PVR).
- ↑Afterload → ↓SV.
- Contractility (Inotropy): Intrinsic strength of myocardial contraction.
- ↑Sympathetic tone (e.g., catecholamines), ↑Ca²⁺ influx → ↑Contractility → ↑SV.
- Independent of loading conditions.
📌 Mnemonic: PAC (Preload, Afterload, Contractility) drives Stroke Volume.
⭐ The Frank-Starling mechanism ensures that the heart automatically adjusts its output to match venous return, preventing blood accumulation.
Factors Modulating CO - The Output Shifters
- CO ↑ (Increased Output):
- Physiological:
- Exercise (up to 5-7x)
- Anxiety, excitement (sympathetic ↑)
- Pregnancy (↑ blood volume, ↑ metabolism)
- Eating, high environmental temperature
- Pathological:
- Hyperthyroidism (↑ BMR)
- Anemia (↓ O2 capacity, ↓ viscosity)
- Arteriovenous (AV) shunts (↓ TPR)
- Beriberi (Thiamine deficiency → vasodilation)
- Physiological:
- CO ↓ (Decreased Output):
- Physiological:
- Standing (postural change, transient ↓ VR)
- Pathological:
- Heart failure (↓ contractility)
- Myocardial Infarction (MI)
- Hemorrhage, hypovolemia (↓ VR)
- Shock (e.g., cardiogenic, hypovolemic)
- Severe valvular disease (stenosis/regurgitation)
- Cardiac tamponade (↓ filling)
- Hypothyroidism (↓ BMR)
- Physiological:
⭐ Anemia significantly ↑ CO (can double) due to ↓ blood viscosity & tissue hypoxia leading to peripheral vasodilation.
Cardiac Output Measurement - Quantifying the Flow
- Fick Principle: Uses O₂ consumption. $CO = \frac{VO_2}{C_aO_2 - C_vO_2}$. Invasive; original gold standard.
- Indicator Dilution:
- Thermodilution: Cold saline via pulmonary artery catheter (Swan-Ganz). Stewart-Hamilton equation. Common.
- Dye dilution (Indocyanine green): Historically used, now rare.
- Echocardiography: Widely used, non-invasive. Doppler (VTI (aortic)) or 2D for Stroke Volume (SV). $CO = SV \times HR$.
- Pulse Contour Analysis: Minimally invasive (arterial line); SV from arterial waveform, allows continuous monitoring.
⭐ Thermodilution via pulmonary artery catheter (PAC) is a key invasive reference method in critical care.
High‑Yield Points - ⚡ Biggest Takeaways
- CO = HR × SV; normal adult value is ~5 L/min.
- Frank-Starling Law: ↑Preload (venous return, EDV) directly ↑SV.
- Afterload: Resistance to ventricular ejection (e.g., systemic vascular resistance, aortic pressure).
- Contractility: Intrinsic myocardial pump effectiveness, altered by inotropes and ANS.
- ANS: Sympathetic ↑CO (↑HR, ↑SV); Parasympathetic (vagal) ↓HR, thus ↓CO.
- Fick Principle: CO = O₂ consumption / (Arterial O₂ content - Venous O₂ content).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

