Cardiac Action Potentials - Shocking Phases
 action potential with phases and ionic currents)
action potential with phases and ionic currents)
 action potential with phases and ionic currents)
action potential with phases and ionic currents)
- Comparison of Cardiac Action Potentials:
| Feature | Non-Pacemaker (Ventricular/Atrial) | Pacemaker (SA/AV Node) |
|---|---|---|
| RMP | Stable $\approx \textbf{-90mV}$ | Unstable $\approx \textbf{-60mV}$ |
| Threshold | $\approx \textbf{-70mV}$ | $\approx \textbf{-40mV}$ to $\textbf{-50mV}$ |
| Phase 0 (Upstroke) | Rapid $Na^+$ influx ($I_{Na}$) | Slow $Ca^{2+}$ influx ($I_{Ca,L}$) |
| Phase 1 (Early Repol.) | Transient $K^+$ efflux ($I_{to}$) | Absent |
| Phase 2 (Plateau) | $Ca^{2+}$ influx ($I_{Ca,L}$), $K^+$ efflux ($I_K$) | Absent |
| Phase 3 (Repol.) | Rapid $K^+$ efflux ($I_K$) | $K^+$ efflux ($I_K$) |
| Phase 4 | Resting potential ($I_{K1}$) | Spontaneous diastolic depolarization: $Na^+$ influx ($I_f$ - funny current), $Ca^{2+}$ ($I_{Ca,T}$) |
Introduction to Cardiac Electrophysiology
What is Cardiac Electrophysiology?
Cardiac electrophysiology is the study of the electrical properties and activities of the heart that enable coordinated cardiac contraction. The heart functions as both a mechanical pump and an electrical system, where electrical impulses initiate and coordinate each heartbeat.
Why Study Cardiac Electrophysiology?
Understanding cardiac electrophysiology is fundamental for:
- Clinical Diagnosis: Interpreting ECGs and identifying arrhythmias
- Therapeutic Interventions: Managing cardiac rhythm disorders
- Pharmacology: Understanding how cardiac drugs affect electrical conduction
- Pathophysiology: Recognizing how diseases alter normal cardiac electrical activity
Key Concepts We'll Explore:
- Cardiac Action Potentials: The electrical events in different cardiac cells
- Conduction System: How electrical impulses spread through the heart
- ECG Interpretation: Recording and understanding the heart's electrical activity
- Autonomic Regulation: How the nervous system controls heart rhythm
- Clinical Applications: High-yield points for medical examinations
Foundation Principles:
The heart's electrical system operates on three fundamental principles:
- Automaticity: Certain cardiac cells can spontaneously generate electrical impulses
- Conductivity: Electrical impulses can spread from cell to cell
- Excitability: Cardiac cells can respond to electrical stimulation
⭐ Clinical Relevance: Cardiac electrophysiology forms the basis for understanding arrhythmias, ECG interpretation, and the mechanism of action of antiarrhythmic drugs - all high-yield topics for medical examinations.
This comprehensive overview will prepare you to understand the detailed mechanisms that follow, from action potentials to clinical applications.
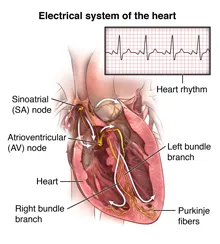
Conduction System - Heart's Highway
- SA Node (Pacemaker): 60-100 bpm. Initiates impulse.
- Internodal/Atrial Pathways: Spread to AV node.
- AV Node (Gatekeeper): 40-60 bpm. Delay: 0.12-0.20 s (ventricular filling).
- Bundle of His & Branches: To ventricles. His rate: 20-40 bpm.
- Purkinje Fibers: Rapid distribution. Rate: 15-40 bpm. Fastest conduction.
- 📌 Mnemonic: "Silly Aussies Bake Perfect Pies" (SA node, Atria, AV node, Bundle of His, Purkinje fibers, Papillary muscles)

⭐ The AV node acts as a 'gatekeeper', slowing conduction to allow for adequate ventricular filling before contraction.
ECG Basics - Wave Wisdom
ECG records heart's electrical activity. Key components:
| ECG Component | Electrical Event / Significance | Normal Values |
|---|---|---|
| P Wave | Atrial depolarization | Height <2.5 mm, width <0.12 s |
| PR Interval | AV conduction (P onset to QRS onset) | 0.12-0.20 s |
| QRS Duration | Ventricular depolarization | <0.12 s (typically 0.08-0.10 s) |
| ST Segment | Isoelectric; early ventricular repolarization (plateau) | Baseline |
| T Wave | Ventricular repolarization | Upright in most leads |
| QT Interval | Total ventricular systole (depol + repol) | Rate-dependent; QTc (Bazett: $QTc = \frac{QT}{\sqrt{RR}}$) <0.44s(M), <0.46s(F) |
| U Wave | Late repolarization (Purkinje/papillary) | Not always seen; if present, same polarity as T |
Regulation & Properties - Electric Control
Autonomic Nervous System (ANS) Effects on Heart
| Property | Sympathetic (NE, $\beta_1$) | Parasympathetic (ACh, $M_2$) |
|---|---|---|
| Chronotropy (HR) | ↑ (↑ SA node Phase 4 slope: ↑ $I_f$, ↑ $I_{Ca,L}$) | ↓ (↓ SA node Phase 4 slope: ↑ $I_{K,ACh}$, ↓ $I_f$) |
| Dromotropy (AV) | ↑ Conduction (↑ $I_{Ca,L}$) | ↓ Conduction (↓ $I_{Ca,L}$, ↑ $I_{K,ACh}$) |
| Inotropy | ↑ Contractility (↑ $Ca^{2+}$ influx) | ↓ Atrial contractility (↓ $I_{Ca,L}$); minimal ventricular effect |
Refractory Periods:
- Absolute (ARP): No new AP possible. Na+ channels inactivated.
- Effective (ERP): ARP + early RRP. No propagated AP can be generated.
- Relative (RRP): Stronger stimulus needed for AP. Some Na+ channels recovered.
⭐ Sympathetic stimulation increases heart rate by increasing the slope of phase 4 depolarization in SA nodal cells, primarily through enhanced $I_f$ and $I_{Ca,L}$ currents.
High‑Yield Points - ⚡ Biggest Takeaways
- SA node is the primary pacemaker (60-100 bpm).
- AV node causes crucial conduction delay (PR interval) for ventricular filling.
- Phase 0 (rapid depolarization) in ventricular myocytes is due to Na+ influx.
- Phase 3 (repolarization) in ventricular myocytes is primarily due to K+ efflux.
- Effective Refractory Period (ERP) protects against cardiac tetany.
- QT interval prolongation is a risk factor for Torsades de Pointes.
- Vagal stimulation ↓ heart rate; sympathetic stimulation ↑ heart rate and contractility.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

