Platelet Essentials - Tiny Clotting Titans
- Origin: Megakaryocytes (bone marrow). Lifespan: 7-10 days.
- Normal Count: 1.5 - 4.5 lakh/µL (or 150,000 - 450,000/µL).
- Structure: Anucleated, discoid. Granules:
- Alpha (α): Fibrinogen, vWF, PF4.
- Dense (δ): ADP, ATP, $Ca^{2+}$, Serotonin.
- Key Receptors: GpIb (binds vWF for adhesion), GpIIb/IIIa (binds fibrinogen for aggregation).
- Functions: Primary hemostasis (platelet plug), secondary hemostasis (phospholipid surface), clot retraction.

⭐ Bernard-Soulier syndrome is due to GpIb deficiency, causing impaired platelet adhesion. Glanzmann thrombasthenia is due to GpIIb/IIIa deficiency, causing impaired aggregation.
Primary Hemostasis - The Initial Plug
- Vascular Spasm: Immediate but transient vasoconstriction post-injury.
- Platelet Adhesion:
- Endothelial damage exposes subendothelial collagen & von Willebrand Factor (vWF).
- Platelets adhere: GP Ia/IIa to collagen; GP Ib-IX-V to vWF.
⭐ vWF is critical, acting as a molecular bridge between platelet GP Ib and exposed subendothelial collagen.
- Platelet Activation & Degranulation:
- Adhesion triggers shape change (disc to spiny sphere) and degranulation.
- Release of mediators:
- ADP (potent activator & aggregator)
- Thromboxane A₂ (TXA₂) (vasoconstrictor, promotes aggregation)
- Serotonin (5-HT) (vasoconstrictor)
- Platelet Aggregation:
- Activated platelets express GP IIb/IIIa receptors.
- Fibrinogen binds to GP IIb/IIIa, linking adjacent platelets.
- Forms the initial, unstable primary hemostatic plug.
- 📌 Mnemonic: GP 1b for vWF Binding; GP 2b/3a for 2 (two) platelets to Aggregate.

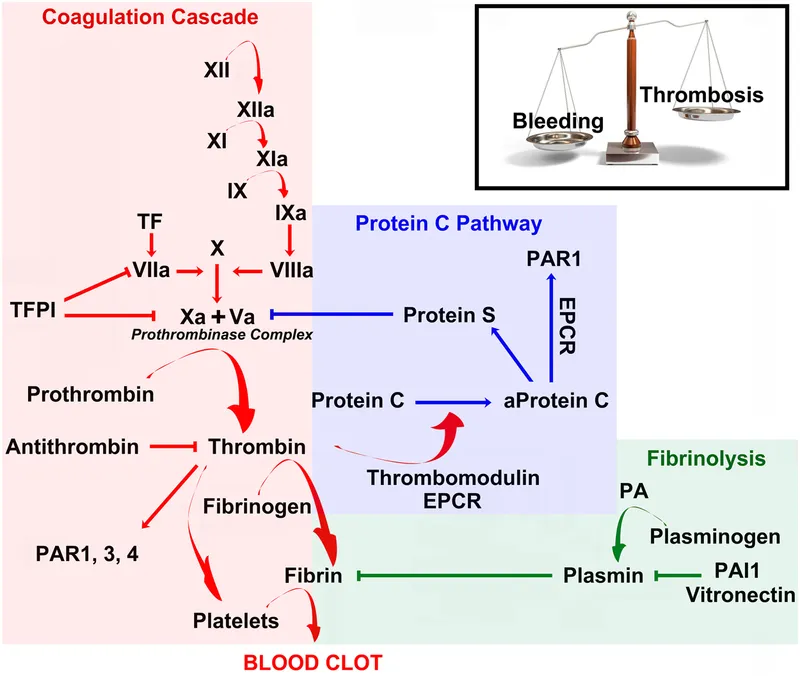
Coagulation Cascade - The Fibrin Factory
- Enzymatic cascade amplifying initial hemostatic plug. Goal: Fibrin mesh formation.
- Pathways:
- Intrinsic Pathway: Activated by subendothelial collagen. Factors XII, XI, IX, VIII. Lab: aPTT.
- Extrinsic Pathway: Tissue Factor (TF/Factor III) release from injury. Factor VII. Lab: PT.
- Common Pathway: Factor X activation (Xa). Xa + Va convert Prothrombin (Factor II) to Thrombin (IIa). Thrombin converts Fibrinogen (Factor I) to Fibrin. Factor XIIIa stabilizes clot.
- 📌 Vit K-dependent factors: II, VII, IX, X, Proteins C & S.

⭐ Calcium (Factor IV) is essential for multiple steps, acting as a cofactor for many coagulation factors.
Fibrinolysis & Regulation - Clot Control Crew
- Fibrinolysis: Enzymatic clot breakdown by Plasmin.
- Plasminogen $\xrightarrow{\text{tPA, uPA}}$ Plasmin.
- Plasmin degrades fibrin $\rightarrow$ FDPs; D-dimer (specific thrombosis marker).
- Key Regulators (Anticoagulants/Inhibitors):
- Antithrombin III: Major inhibitor of thrombin (IIa), Xa. Heparin augments.
- Protein C & S (Vit. K-dep): Inactivate factors Va, VIIIa. Thrombin-thrombomodulin activates.
- TFPI (Tissue Factor Pathway Inhibitor): Inhibits Xa & TF-VIIa.
- PAI-1: Plasminogen Activator Inhibitor-1; inhibits tPA, uPA.
- $\alpha_2$-Antiplasmin: Directly inhibits circulating plasmin.
⭐ D-dimer elevation is crucial in diagnosing DVT, PE, DIC, reflecting ongoing fibrinolysis.
Hemostasis Disorders & Drugs - Clotting Chaos & Cures
- Platelet Disorders:
- Thrombocytopenia: ITP, TTP (ADAMTS13↓), HUS, DIC (consumptive).
- Qualitative: Glanzmann (GpIIb/IIIa↓), Bernard-Soulier (GpIb↓ - 📌 Big Suckers).
- Coagulation Disorders:
- Hemophilia A (FVIII↓), B (FIX↓): X-linked, PTT↑.
- vWD: Most common inherited; BT↑, PTT variable.
- Vit K def: FII, VII, IX, X, C, S↓; PT↑.
- Drugs:
- Antiplatelets: Aspirin (COX inh), Clopidogrel (ADP-R inh).
- Anticoagulants: Heparin (PTT), Warfarin (PT/INR), DOACs (e.g., Rivaroxaban).
- Thrombolytics: Alteplase (tPA).
⭐ Fresh Frozen Plasma (FFP) reverses warfarin rapidly; contains all clotting factors.
High‑Yield Points - ⚡ Biggest Takeaways
- Platelet adhesion: GpIb binds vWF. Aggregation: GpIIb/IIIa binds fibrinogen.
- Bernard-Soulier syndrome: GpIb defect (↓ adhesion). Glanzmann thrombasthenia: GpIIb/IIIa defect (↓ aggregation).
- Aspirin inhibits COX-1 (↓ TXA2). Clopidogrel blocks ADP (P2Y12) receptors.
- Vitamin K is vital for factors II, VII, IX, X, Protein C & S.
- Hemophilia A: Factor VIII deficiency. Hemophilia B: Factor IX deficiency. vWD: vWF defect.
- PT assesses extrinsic/common pathways; aPTT assesses intrinsic/common pathways.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

