Innate Immunity: First Responders & Fortresses
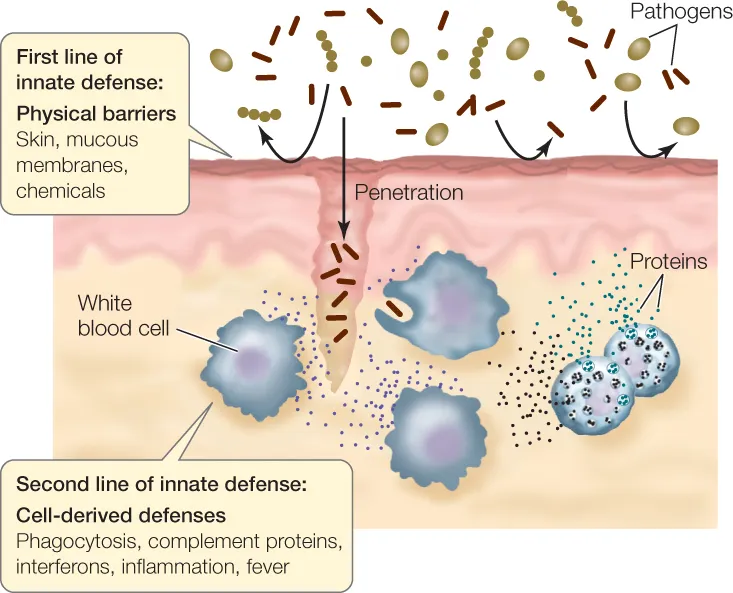
- Body's in-built, immediate defense system; present from birth.
- Characteristics:
- Non-specific: Acts broadly against diverse pathogens.
- Rapid: Mobilized within minutes to hours.
- No immunological memory: Response intensity is consistent upon re-exposure.
| Feature | Innate Immunity | Adaptive Immunity |
|---|---|---|
| Specificity | Low (Pattern recognition) | High (Antigen-specific) |
| Response Time | Fast (Hours) | Slow (Days to weeks) |
| Memory | Absent | Present (Long-term) |
| Key Cells | Phagocytes, NK cells, Mast cells | T-lymphocytes, B-lymphocytes |
Cellular Sentinels - The Immune Foot Soldiers
| Cell Type | Key Identifying Feature/Marker | Primary Function(s) |
|---|---|---|
| Neutrophils | Multi-lobed nucleus (3-5); MPO+, CD66b+ | Phagocytosis (bacteria); acute inflammation; NETs (📌 Neutrophil Extracellular Traps). First responders. |
| Macrophages | Kidney-shaped nucleus; CD14+, CD68+; from monocytes | Phagocytosis; antigen presentation; cytokine release; tissue repair. |
| Dendritic Cells | Star-shaped; high MHC-II, CD11c+ | Potent APCs; link innate & adaptive immunity; T-cell activation. |
| NK Cells | Large granular lymphocyte; CD16+, CD56+ (CD3-) | Kill tumor/virally infected cells (MHC-I independent); ADCC; IFN-γ production. |
| Mast Cells | Granules with histamine, tryptase; c-Kit (CD117)+ | Allergic reactions (Type I); inflammation; parasite defense; degranulation. |
| Eosinophils | Bilobed nucleus; eosinophilic granules (MBP) | Parasite defense; allergic reactions (modulate); chronic inflammation. |
| Basophils | Bilobed/S-shaped nucleus; basophilic granules (histamine) | Allergic/inflammatory reactions; parasite defense; release histamine. |
Molecular Alarms - PAMPs, PRRs & Messengers
- PAMPs (Pathogen-Associated Molecular Patterns): Microbial structures (e.g., LPS, peptidoglycan, dsRNA).
- DAMPs (Damage-Associated Molecular Patterns): Host molecules from stressed/damaged cells.
- PRRs (Pattern Recognition Receptors): Host sensors for PAMPs/DAMPs.
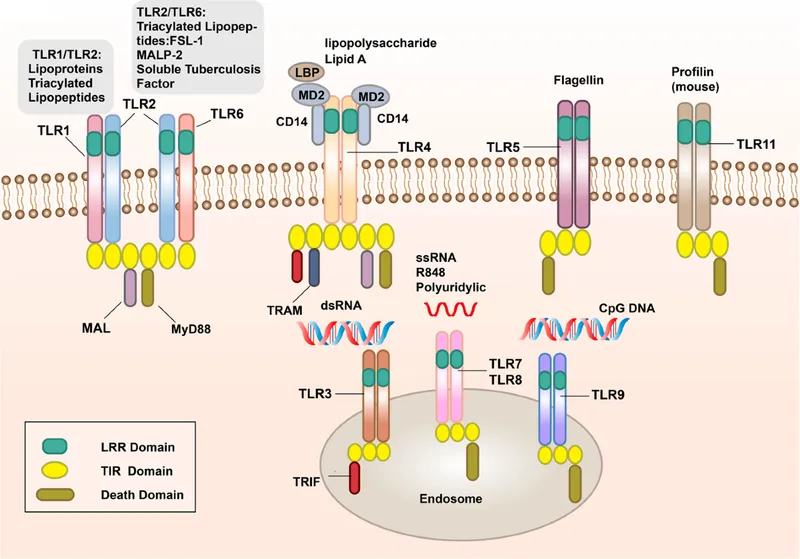
- Toll-like Receptors (TLRs): Key membrane-bound PRRs.
TLR Ligand Recognizes TLR2 Peptidoglycan, Lipoproteins Gram (+) bacteria, Fungi TLR3 dsRNA Viruses TLR4 LPS (Endotoxin) Gram (-) bacteria TLR5 Flagellin Motile bacteria TLR9 Unmethylated CpG DNA Bacterial/Viral DNA - NLRs (NOD-like Receptors): Cytosolic; detect bacterial peptidoglycans, other signals.
- RLRs (RIG-I-like Receptors): Cytosolic; detect viral RNA.
- Toll-like Receptors (TLRs): Key membrane-bound PRRs.
- Complement System: Plasma protein cascade.
- Key Functions: Opsonization (C3b), Anaphylatoxins (C3a, C5a), MAC (C5b-9 lysis).
- Key Cytokines (Soluble Messengers):
- TNF-α, IL-1, IL-6: Pro-inflammatory; fever, acute phase protein synthesis.
- IL-12: Activates NK cells, promotes Th1 differentiation.
- Type I IFNs (IFN-α, IFN-β): Antiviral state; ↑MHC I expression.
⭐ TLR4, along with MD-2 and CD14, is the primary receptor for Lipopolysaccharide (LPS) from Gram-negative bacteria, a critical trigger for septic shock.
Innate Responses - Inflammation & Action
- Inflammation:
- Cardinal signs: Calor (heat), Rubor (redness), Tumor (swelling), Dolor (pain), Functio laesa (loss of function). 📌 Mnemonic: PRISH (Pain, Redness, Immobility, Swelling, Heat).
- Key mediators: Histamine, prostaglandins, leukotrienes.
- Events: Vasodilation, ↑ vascular permeability, leukocyte recruitment.
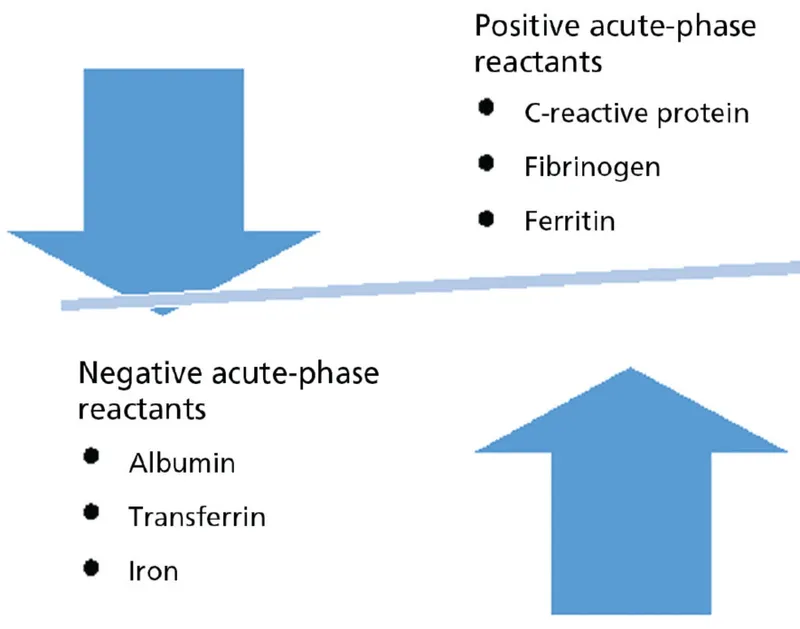
- Acute Phase Reactants (APRs): C-Reactive Protein (CRP), Serum Amyloid A (SAA), Fibrinogen.
- Phagocytosis: Key mechanism for eliminating pathogens and debris.
- Natural Killer (NK) Cells:
- Activation: "Missing self" hypothesis (recognize cells lacking MHC-I).
- Killing mechanism: Release perforins (create pores) and granzymes (induce apoptosis).
⭐ C-Reactive Protein (CRP) is a major acute phase reactant; its levels can increase >1000-fold during acute inflammation, making it a sensitive marker of inflammation and infection.
High-Yield Points - ⚡ Biggest Takeaways
- Innate immunity: Rapid, non-specific, first-line defense; no immunological memory.
- Key cells: Phagocytes (Neutrophils, Macrophages), NK cells, Mast cells, Dendritic cells.
- Recognition: PAMPs (e.g., LPS) by PRRs (e.g., TLRs; TLR4 recognizes LPS).
- Complement system: Key for opsonization, MAC formation (lysis), and inflammation.
- Inflammation: Cardinal signs (rubor, calor, dolor, tumor); mediated by cytokines.
- Type I Interferons (IFN-α, IFN-β): Potent antiviral activity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

