Immunological Memory - Remember Me?
Immunological memory is the immune system's ability to mount an enhanced, faster, and more effective response to subsequent encounters with a previously encountered antigen.
-
Primary vs. Secondary Immune Response
Feature Primary Response Secondary Response Speed Slower (days to weeks) Faster (hours to days) Magnitude Lower Higher (↑100-1000x) Predominant Ab IgM IgG (class switching), IgA, IgE Antibody Affinity Lower Higher Lag Phase Longer Shorter -
Key Cells:
- Memory B cells
- Memory T cells (CD4+ & CD8+)
-
Hallmarks:
- Specificity
- Longevity (can be lifelong)
- Rapidity (quicker activation)
- Heightened reactivity (stronger response)
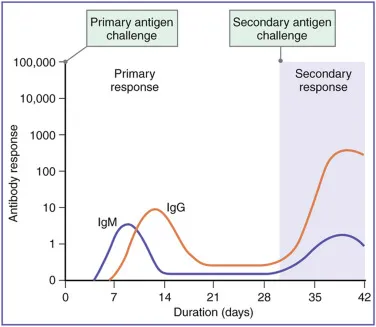
⭐ Secondary response is characterized by a rapid switch to IgG production with higher affinity antibodies due to somatic hypermutation and affinity maturation during the primary response.
Memory Cell Deep Dive - The Veteran Cells
- Memory B Cells:
- Formation: Germinal centers.
- Surface marker: CD27.
- Function: Rapid differentiation to plasma cells, affinity-matured antibodies.
- Memory T Cells:
- General marker: CD45RO. 📌 ROund for memORy (CD45RO), RA for NAive (CD45RA).
- Types:
Type Location Key Function(s) Key Markers Central ($T_{CM}$) SLOs Proliferate, differentiate to effectors CCR7, CD62L Effector ($T_{EM}$) Periphery, blood Rapid effector functions (cytokine release) CCR7-, CD62L- Tissue-Res. ($T_{RM}$) Non-lymphoid tissues Barrier defense, rapid local response CD69, CD103 - Survival & Self-renewal: Maintained by cytokines IL-7 and IL-15.
⭐ Central memory T cells ($T_{CM}$) primarily reside in secondary lymphoid organs, express CCR7 and L-selectin (CD62L), and have high proliferative capacity upon re-exposure to antigen.

Immunological Tolerance - The Peace Treaty
- Definition: Specific unresponsiveness to an antigen (especially self), preventing autoimmunity & maintaining self-non-self discrimination.
- Types & Mechanisms:
- Central Tolerance:
- Location: Thymus (T cells), Bone Marrow (B cells).
- Key Process: Deletion (apoptosis) of self-reactive lymphocytes.
- Peripheral Tolerance:
- Location: Secondary lymphoid organs, peripheral tissues.
- Key Processes: Anergy, suppression by Tregs, deletion.
- Central Tolerance:
- Factors Favoring Tolerance: High antigen dose, persistence, oral/IV route, absent co-stimulation, neonatal exposure.

⭐ The AIRE (Autoimmune Regulator) protein is crucial for expressing diverse tissue-specific antigens in the thymus, essential for central T cell tolerance.
Tolerance Mechanisms - Keeping a Lid On It
Error: Failed to generate content for this concept group.
High‑Yield Points - ⚡ Biggest Takeaways
- Immunological memory underpins vaccination, causing faster, stronger secondary responses via memory cells.
- Memory B cells rapidly secrete high-affinity IgG upon antigen re-encounter.
- Memory T cells (TCM & TEM) provide long-term cellular immunity.
- Immunological tolerance prevents autoimmunity by maintaining unresponsiveness to self-antigens.
- Central tolerance eliminates self-reactive lymphocytes via negative selection in primary lymphoid organs.
- Peripheral tolerance uses anergy, Treg (FoxP3+) suppression, and AICD (Activation-Induced Cell Death).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

