Adaptive Immunity Essentials - Smart Shield 101
- Core Features: Specificity (targets unique antigens), Memory (stronger recall), Diversity (vast antigen repertoire), Self-tolerance (ignores self).
- Main Types:
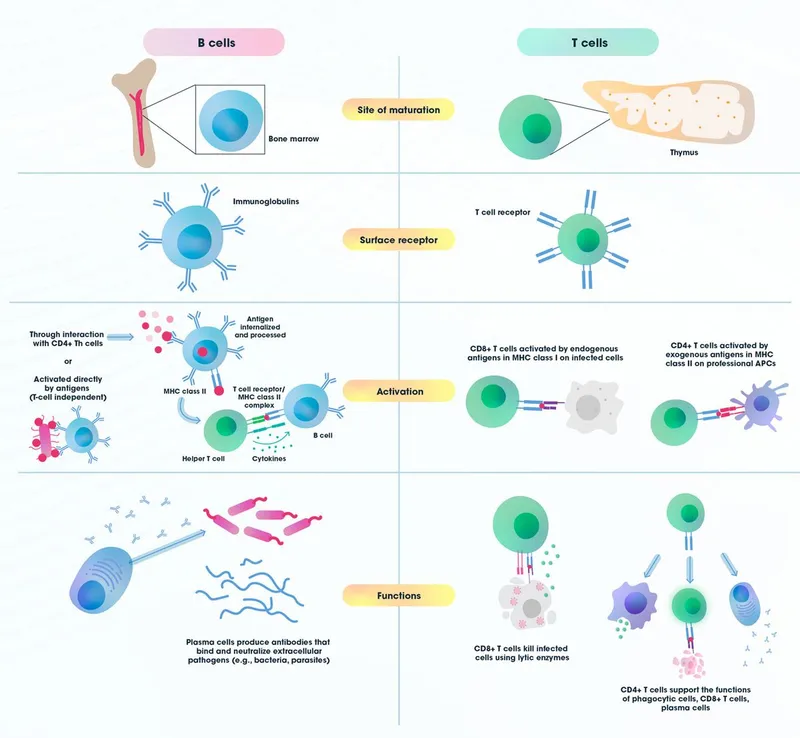
- Humoral Immunity: B-lymphocytes → plasma cells → antibodies (IgM, IgG, etc.). Targets extracellular pathogens.
- Cell-Mediated Immunity (CMI): T-lymphocytes.
- Helper T-cells (CD4+): Orchestrate response; activate B-cells, macrophages.
- Cytotoxic T-cells (CD8+): Kill infected/tumor cells. Targets intracellular pathogens.
- Distinct from Innate: Slower onset, highly specific, generates lasting memory.
⭐ Clonal selection: Antigen encounter triggers specific lymphocyte proliferation and differentiation into effector and memory cells.
Meet the Specialists - Immune Cell Lineup
-
T Lymphocytes (Thymus): 📌 Thymus Teacher
- Helper (CD4+): Activate immune cells.
- Cytotoxic (CD8+): Kill infected/tumor cells.
- Regulatory (Tregs): Suppress immunity.
-
B Lymphocytes (Bone Marrow): 📌 Bone Marrow Breeder
- Plasma cells (Ab factory), Memory B cells.
-
Antigen Presenting Cells (APCs):
- Dendritic (potent), Macrophages, B cells. Process/present antigens.
-
Antigens: Foreign molecules triggering immune response.
-
Antibodies (Ig): Y-shaped. 📌 GAMED classes:
- IgG: Main blood Ab, crosses placenta.
- IgA: Secretory (mucosal).
- IgM: 1st responder, pentamer.
- IgE: Allergy, parasites.
- IgD: B-cell surface receptor.
-
MHC (Major Histocompatibility Complex):
- MHC I: All nucleated cells; to CD8+ T. (📌 1x8=8)
- MHC II: APCs; to CD4+ T. (📌 2x4=8)
⭐ B cells act as APCs, presenting antigen to helper T cells via MHC II, crucial for T-dependent B cell activation.
Cell-Mediated Command - T-Cell Takedowns
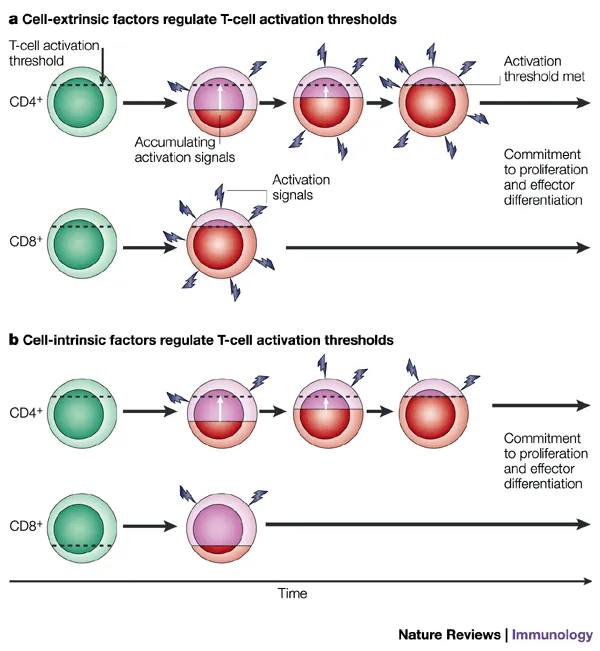
- T-Cell Activation (Two-Signal Hypothesis):
- Signal 1: T-Cell Receptor (TCR) binds MHC-peptide complex on Antigen Presenting Cell (APC).
- Signal 2: Co-stimulation (e.g., CD28 on T-cell binds B7 (CD80/CD86) on APC).
- APCs: Dendritic cells (most potent), macrophages, B-cells.
- CD4+ T-Helper (Th) Cells (MHC-II restricted): Orchestrate immune response.
- Th1: IFN-γ, IL-2. Activates macrophages, CTLs. Intracellular pathogens.
- Th2: IL-4, IL-5, IL-13. B-cell help (Ab production), eosinophil activation. Extracellular parasites.
- Th17: IL-17, IL-22. Pro-inflammatory, neutrophil recruitment. Extracellular bacteria, fungi.
- Treg: TGF-β, IL-10. Suppress immune response, maintain tolerance. 📌 FOXP3+
- CD8+ Cytotoxic T-Lymphocytes (CTLs) (MHC-I restricted): Kill infected/tumor cells.
- Mechanisms: Perforin/Granzyme release, Fas/FasL interaction (apoptosis).
⭐ Absence of co-stimulation (Signal 2) during T-cell activation (Signal 1 present) can lead to T-cell anergy or tolerance.
Humoral & Memory - B-Cell Blast & Backup
- B-Cell Activation & Differentiation:
- Naive B-cell encounters specific antigen via B-Cell Receptor (BCR).
- Requires co-stimulation from T-helper (Th) cells (CD40-CD40L interaction).
- Undergoes clonal expansion and differentiates into plasma cells & memory B-cells.
- Plasma Cells (Effector B-Cells):
- Short-lived antibody-secreting cells.
- Primary immune response: IgM produced first, followed by IgG.
- Antibody Functions (📌 ONA-C):
- Opsonization: Enhances phagocytosis.
- Neutralization: Blocks pathogen/toxin action.
- Agglutination: Clumps pathogens.
- Complement Activation: Via classical pathway (IgG, IgM).
- Memory B-Cells & Immunological Memory:
- Long-lived cells, provide rapid & robust response upon re-exposure (anamnestic response).
- Basis of vaccination.
- Secondary response: Predominantly high-affinity IgG.
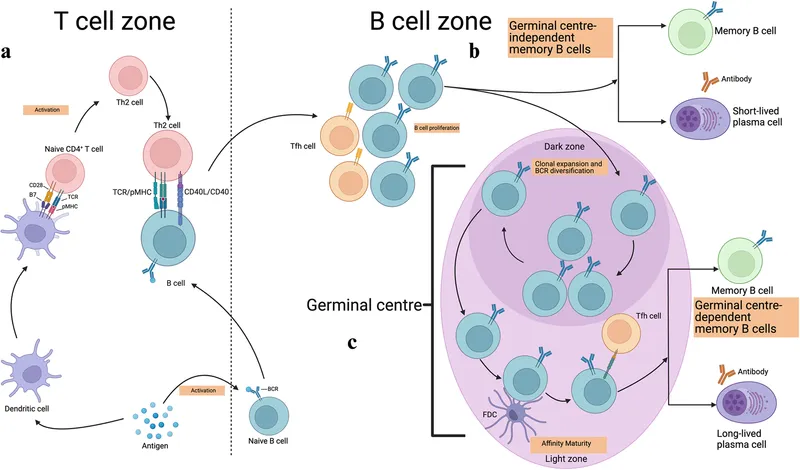
⭐ Affinity maturation, somatic hypermutation, and class switching primarily occur in the germinal centers of secondary lymphoid organs, leading to higher affinity antibodies during the course of an immune response. This is crucial for effective long-term immunity and memory.
High‑Yield Points - ⚡ Biggest Takeaways
- T-cell activation needs dual signals: TCR-MHC and co-stimulation (B7-CD28).
- MHC I presents endogenous antigens to CD8+ T cells (cytotoxic).
- MHC II presents exogenous antigens to CD4+ T cells (helper).
- B-cell activation yields plasma cells (antibodies) and memory B cells.
- Antibody class switching requires CD40L-CD40 interaction and cytokines.
- Affinity maturation in germinal centers via somatic hypermutation.
- Central tolerance (thymus/bone marrow) & peripheral tolerance prevent autoimmunity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

