Bronchodilators: Overview & Classes - Airway Openers 101
- Drugs that dilate bronchi & bronchioles, decreasing airway resistance and improving airflow to the lungs.
- Mechanism: Primarily act by relaxing airway smooth muscle; some also modulate inflammation.
- Key indications: Asthma, Chronic Obstructive Pulmonary Disease (COPD).
- Major Classes:
- β2-Adrenergic Agonists (e.g., Salbutamol, Formoterol)
- Muscarinic Antagonists (e.g., Ipratropium, Tiotropium)
- Methylxanthines (e.g., Theophylline)
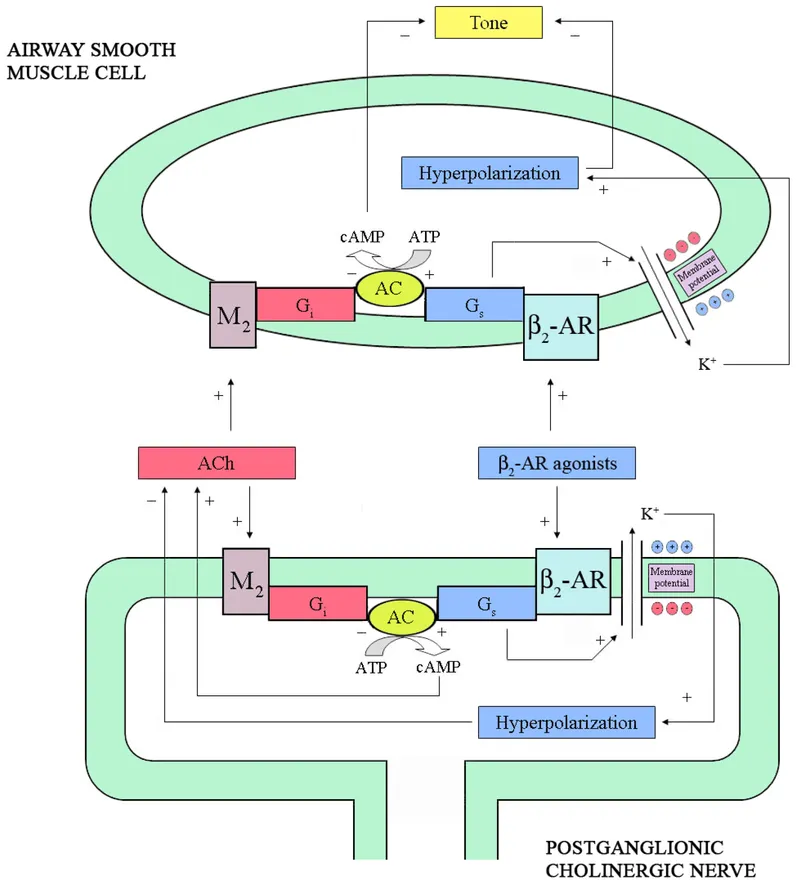
⭐ β2-agonists are the most effective bronchodilators; they activate adenylyl cyclase, leading to increased intracellular cAMP, which causes bronchial smooth muscle relaxation. 📌 Remember "BAM" for Bronchodilator classes: Beta-agonists, Anticholinergics, Methylxanthines for quick recall during exams!
Beta-2 Agonists - Speedy Relief Crew
- MOA: Activate $\beta_2$ adrenergic receptors → $↑cAMP$ → bronchial smooth muscle relaxation & bronchodilation.
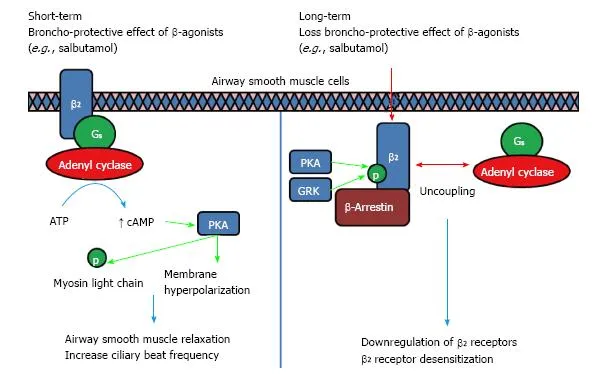
- Types & Uses:
Feature SABA (Short-Acting) LABA (Long-Acting) Ultra-LABA Drugs Salbutamol, Levosalbutamol, Terbutaline Salmeterol, Formoterol Indacaterol, Olodaterol, Vilanterol Onset <5 min Sal: 20 min, For: 2-3 min 5-15 min Duration 4-6 hrs >12 hrs >24 hrs Role Rescue (acute asthma/COPD) Maintenance (Asthma with ICS, COPD) Maintenance (COPD, Asthma) - 📌 Mnemonic (SABA): "Salbutamol Alleviates Breathlessness Acutely."
- Key Side Effects: Tachycardia, palpitations, tremor, hypokalemia (monitor K+), headache.
⭐ Exam Favourite: Formoterol (LABA) has rapid onset (2-3 min), like SABAs, suiting reliever/maintenance (SMART therapy).
Antimuscarinics (Anticholinergics) - Block That Squeeze
-
Mechanism: Block M3 receptors in airway smooth muscle → bronchodilation by ↓ vagal tone.
-
Primary use: COPD (maintenance/relief). Adjunct in severe asthma.
-
Comparison:
Feature SAMA (e.g., Ipratropium) LAMA (e.g., Tiotropium) Onset 15-30 min ~30 min Duration 4-6 hrs 12-24 hrs (Tio: 24h) Use Acute relief (COPD/asthma) Maintenance (COPD, asthma) -
Key Drugs:
- SAMA: Ipratropium bromide, Oxitropium bromide.
- LAMA: Tiotropium, Glycopyrronium, Aclidinium, Umeclidinium.
-
Side Effects: Dry mouth (common), metallic taste. Systemic effects (blurred vision, urinary retention) rare with inhaled quaternary amines.
-
Caution: Narrow-angle glaucoma, BPH.

⭐ Ipratropium, a quaternary amine, has minimal systemic absorption, enhancing safety.
Methylxanthines - Old School Power
- Examples: Theophylline, Aminophylline (IV).
- MOA: Non-selective PDE inhibition (↑cAMP, ↑cGMP); Adenosine receptor antagonism; ↑HDAC activity (anti-inflammatory).
- Therapeutic Range: 10-20 mcg/mL (narrow).
- AEs: Tachycardia, arrhythmias, N/V, CNS stimulation, seizures (toxic).
- 📌 THEO: Tremors/Tachycardia, Hyperthermia/Headache, Emesis, Overdose (seizures, arrhythmias).
- Interactions: CYP450 metabolism (many drugs affect levels; smoking ↓ levels).
⭐ Theophylline toxicity is precipitated by macrolides (e.g., erythromycin) and quinolones (e.g., ciprofloxacin) due to CYP1A2 inhibition.
Bronchodilator Clinical Strategy - Pick Your Player
- SABA (Salbutamol): Acute relief (SOS).
- LABA (Salmeterol, Formoterol): Chronic asthma (with ICS), COPD.
- SAMA (Ipratropium): Acute asthma/COPD (adjunct).
- LAMA (Tiotropium): COPD (mainstay), severe asthma.
- Methylxanthines (Theophylline): 3rd line, monitor levels.
⭐ Formoterol: a LABA with rapid onset, suitable for SMART therapy (Single Maintenance And Reliever Therapy) in asthma.
High‑Yield Points - ⚡ Biggest Takeaways
- SABA (e.g., Salbutamol) are first-line rescue for acute asthma attacks.
- LABA (e.g., Salmeterol) for asthma maintenance, always combined with ICS.
- Anticholinergics (e.g., Ipratropium, Tiotropium) are first-line for COPD; Ipratropium in severe acute asthma.
- Theophylline: narrow therapeutic index; watch for seizures and arrhythmias.
- Leukotriene antagonists (e.g., Montelukast) for aspirin-exacerbated respiratory disease & exercise-induced asthma.
- Omalizumab (Anti-IgE monoclonal antibody) for severe, persistent allergic asthma.
- Roflumilast (PDE-4 inhibitor) reduces COPD exacerbations in severe cases_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

