Intro to Psychiatric PGx - Gene-Drug Dance
- Pharmacogenomics (PGx): Study of how an individual’s genetic makeup influences their response to medications.
- Psychiatric PGx Focus: Aims to personalize psychiatric treatment by predicting drug efficacy and adverse drug reactions (ADRs) based on genetic variations.
- Core Principle: Genes influence both pharmacokinetics (what the body does to the drug) and pharmacodynamics (what the drug does to the body).
- Key Gene Groups:
- Metabolizing Enzymes: Cytochrome P450 (CYP) family (e.g., CYP2D6, CYP2C19) crucial for processing many psychotropics.
- Drug Targets/Transporters: E.g., Serotonin transporter (SLC6A4) for SSRIs.
- Clinical Goal: Optimize drug selection & dosage, ↑ treatment success, ↓ trial-and-error.
⭐ Variations in the CYP2D6 gene can classify individuals as poor, intermediate, extensive, or ultrarapid metabolizers, significantly impacting plasma concentrations and clinical outcomes of many antidepressants and antipsychotics like risperidone and aripiprazole. This is a frequent exam topic regarding ADRs or efficacy failures.
Key Metabolic Genes (CYPs) - Metabolism Masters
Cytochrome P450 (CYP) enzymes: Key for Phase I drug metabolism. Genetic variations (polymorphisms) alter activity:
- Poor Metabolizers (PM): ↑Drug levels, ↑Toxicity risk.
- Intermediate Metabolizers (IM): ↓Enzyme activity.
- Extensive Metabolizers (EM): Normal activity (wild-type).
- Ultra-rapid Metabolizers (UM): ↓Drug levels, ↓Efficacy risk.
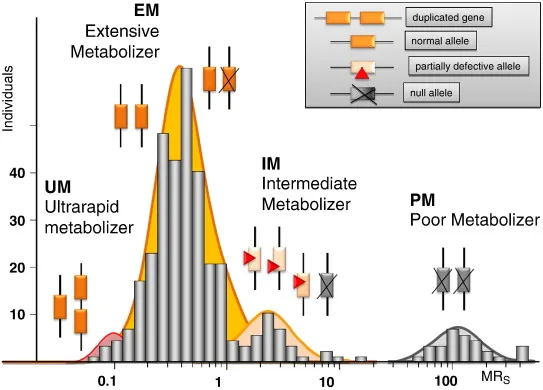
Major Psychiatric CYPs & Clinical Pearls:
- CYP2D6:
- Substrates: Many SSRIs (e.g., paroxetine, fluoxetine), TCAs, risperidone, aripiprazole, atomoxetine.
- PMs (~7% Caucasians): ↑Toxicity. UMs: ↓Efficacy.
- CYP2C19:
- Substrates: Citalopram, escitalopram, sertraline, diazepam, some TCAs.
- PMs (~2-5% Caucasians, ~15-20% Asians): ↑Side effects.
- CYP3A4/5:
- Substrates: Alprazolam, quetiapine, lurasidone, buspirone.
- Inducers (e.g., carbamazepine): ↓Drug levels. Inhibitors (e.g., grapefruit juice): ↑Drug levels.
- CYP1A2:
- Substrates: Clozapine, olanzapine, duloxetine.
- 📌 Smoking (PAHs are inducers) → ↓clozapine/olanzapine levels.
⭐ Smoking induces CYP1A2, potentially decreasing clozapine plasma levels by up to 50%. This can lead to therapeutic failure; dose adjustments are critical with changes in smoking status.
Key Pharmacodynamic Genes - Target Tactics
- Serotonin System:
- HTR2A (Receptor): Polymorphisms (e.g., -1438A/G) affect antipsychotic response (clozapine) & side effects (weight gain); SSRI efficacy.
- SLC6A4 (SERT Transporter): 5-HTTLPR polymorphism.
- S (short) allele: ↓ transporter, ↓ SSRI efficacy, ↑ side effects.
- L (long) allele: better SSRI response.
- 📌 Slow Starters Suffer (S-allele & SSRIs).
- Dopamine System:
- DRD2 (Receptor): Taq1A (ANKK1) A1 allele: ↓ D2 density, affects antipsychotic efficacy, ↑ tardive dyskinesia.
- DRD3 (Receptor): Ser9Gly polymorphism: antipsychotic response.
- Other Key Genes:
- BDNF: Val66Met (Met allele: ↓ BDNF secretion, poorer antidepressant response).
- CACNA1C: Risk for bipolar, schizophrenia; may affect lithium response.
⭐ SLC6A4 5-HTTLPR polymorphism significantly influences SSRI efficacy and side-effect profiles; 'S' allele often means poorer outcomes.
Clinical Application of PGx - Test & Treat Wisely
- Goal: Tailor drug selection & dosing using genetic data.
- Benefits:
- ↑ Efficacy, ↓ ADRs.
- Personalized therapy, ↓ trial-and-error.
- Consider PGx Testing If:
- Poor treatment response.
- History of significant Adverse Drug Reactions (ADRs).
- Starting drugs with known PGx markers (e.g., TCAs, SSRIs, carbamazepine).
- Key Gene-Drug Pairs:
- CYP2D6, CYP2C19: Metabolism of many SSRIs, TCAs, antipsychotics. (Phenotypes: Poor, Intermediate, Normal, Ultrarapid Metabolizers).
- HLA-B**1502*: Carbamazepine & risk of Stevens-Johnson Syndrome (SJS)/Toxic Epidermal Necrolysis (TEN).
- HLA-A**3101*: Carbamazepine & Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS)/Maculopapular Exanthema (MPE).
- Limitations:
- Guidelines not available for all psychotropic drugs.
- Cost, accessibility, Variants of Uncertain Significance (VUS).
- Supplements clinical judgment; does not replace it.
⭐ Testing for HLA-B1502* is strongly recommended in individuals of Asian ancestry before initiating carbamazepine due to high risk of SJS/TEN. For European ancestry, HLA-A3101* is more relevant for carbamazepine-induced hypersensitivity reactions like DRESS or MPE.
High‑Yield Points - ⚡ Biggest Takeaways
- CYP2D6 polymorphisms alter metabolism of many antidepressants (SSRIs, TCAs) & antipsychotics (risperidone).
- CYP2C19 variants impact metabolism of SSRIs (citalopram, sertraline) & some TCAs.
- HLA-B*1502 testing is vital in Asians before carbamazepine to prevent SJS/TEN.
- HLA-A*3101 links to carbamazepine hypersensitivity (DRESS) in diverse populations.
- CYP1A2 activity (smoking induces) affects clozapine & olanzapine levels.
- ADRA2A variants may predict methylphenidate response in ADHD.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

