Cytochrome P450 Polymorphisms - Enzyme Superfamily
- Heme-containing monooxygenases.
- Location: Primarily Endoplasmic Reticulum (microsomal); some in Mitochondria.
- Function: Key enzymes in Phase I drug metabolism.
- Catalyze reactions: Oxidation (most common), reduction, hydrolysis.
- Nomenclature: e.g., CYP2D6
- CYP: Cytochrome P450
- 2: Family (≥40% amino acid sequence homology)
- D: Subfamily (≥55% homology)
- 6: Individual gene.
⭐ CYP3A4 is the most abundant CYP enzyme in the human liver and metabolizes approximately 50% of clinically used drugs.
Cytochrome P450 Polymorphisms - Code Tweaks
Genetic variations in CYP genes alter drug metabolism. Key types:
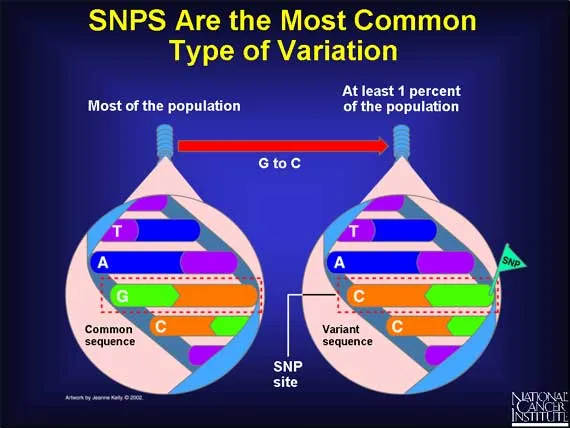
- Single Nucleotide Polymorphisms (SNPs): Single base changes affecting enzyme activity.
- Copy Number Variations (CNVs): Gene duplications (↑ activity) or deletions (↓ activity).
Allele Nomenclature:
- *1: Wild-type (normal function).
- *2, *3, etc.: Variant alleles (altered function).
Metabolizer Phenotypes & Implications:
| Phenotype | Activity | Clinical Implication |
|---|---|---|
| Ultra-rapid (UM) | ↑↑ | Risk of therapeutic failure |
| Extensive (EM) | Normal | Expected drug response |
| Intermediate (IM) | ↓ | Risk of side effects, ↓ clearance |
| Poor (PM) | ↓↓/None | High risk of toxicity, minimal clearance |
⭐ Copy Number Variations (CNVs) of the CYP2D6 gene are a major cause of the ultra-rapid metabolizer (UM) phenotype.
Cytochrome P450 Polymorphisms - CYP All-Stars
Genetic variations in CYP enzymes significantly alter drug metabolism, affecting efficacy and toxicity.
| Enzyme | Key Variants | Common Substrates | Clinical Relevance of Polymorphisms |
|---|---|---|---|
| CYP2D6 | Non-functional: * extit{3},* extit{4},* extit{5} Reduced function: * extit{10},* extit{17} Increased function: Duplications | Codeine, Tamoxifen, β-blockers (metoprolol, carvedilol), Antidepressants (SSRIs, TCAs), Antipsychotics | Poor metabolizers (PMs): ↑ toxicity (e.g., TCAs) or ↓ efficacy (e.g., codeine, tamoxifen). Ultrarapid metabolizers (UMs): ↓ efficacy or ↑ active metabolite toxicity. |
| CYP2C19 | Non-functional: * extit{2},* extit{3} Increased function: * extit{17} | Clopidogrel, PPIs (omeprazole), Diazepam, Voriconazole | PMs: ↓ clopidogrel efficacy (↑ risk of stent thrombosis), ↑ PPI/diazepam exposure. UMs (*17/*17): ↑ clopidogrel active metabolite, ↓ PPI efficacy. |
| CYP2C9 | Reduced function: * extit{2},* extit{3} | Warfarin, Phenytoin, NSAIDs (ibuprofen, celecoxib), Losartan | PMs: ↑ warfarin/phenytoin exposure (↑ bleeding/toxicity risk). Requires lower doses. |
📌 Mnemonic for CYP2D6 substrates: Can Tom Beat All Antidepressants? (Codeine, Tamoxifen, Beta-blockers, Antipsychotics, Antidepressants).
Cytochrome P450 Polymorphisms - Dosing Dilemmas
- Genetic variations in CYP enzymes (e.g., CYP2D6, CYP2C19, CYP2C9) alter drug metabolism.
- Clinical Implications:
- Prodrug Activation: ↓ effect with Poor Metabolizers (PMs).
- Codeine (CYP2D6) → Morphine.
- Clopidogrel (CYP2C19) → Active form.
- Drug Toxicity: ↑ risk in PMs.
- Warfarin (CYP2C9).
- TCAs (CYP2D6).
- Therapeutic Failure: ↓ efficacy in PMs.
- Tamoxifen (CYP2D6) → Endoxifen.
- Prodrug Activation: ↓ effect with Poor Metabolizers (PMs).
- Dosing: Adjust based on genotype; Clinical Pharmacogenetics Implementation Consortium (CPIC) guidelines are key. Ethnic variations in allele frequencies impact population risk.
⭐ Patients with CYP2C19 loss-of-function alleles (e.g., *2, *3) exhibit diminished response to clopidogrel, leading to higher risk of major adverse cardiovascular events like stent thrombosis.
High‑Yield Points - ⚡ Biggest Takeaways
- CYP2D6 metabolizes many psychiatric drugs & opioids (codeine); polymorphisms affect efficacy/toxicity.
- CYP2C19 activates clopidogrel; poor metabolizers have ↑ stent thrombosis risk.
- CYP2C9 variants require ↓ warfarin dose due to ↑ bleeding risk.
- CYP3A4/5 metabolize ~50% of drugs; polymorphisms generally less critical.
- Inducers (rifampicin) ↑ CYP activity, ↓ drug levels; Inhibitors (ketoconazole) ↓ activity, ↑ drug levels.
- Genetic testing aids drug selection/dosing for narrow therapeutic index drugs.
- Ethnic variations in CYP alleles impact population drug responses.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

