Stroke ID & Initial Steps - Brain Attack Alert!
- Recognize Stroke: 📌 BE-FAST (Balance, Eyes, Face, Arm, Speech, Time to call).
- Immediate Actions (Pre-hospital & ED):
- Stabilize: ABCs (Airway, Breathing, Circulation).
- Check: Vital signs, Blood Glucose (fingerstick) - rule out mimics (e.g., < 50 mg/dL or > 400 mg/dL)!
- History: Last Known Well (LKW) time is CRITICAL.
- Neurological Exam: Baseline NIHSS score.
- Activate Stroke Protocol: "Brain Attack" team.
- Crucial First Imaging:
- Non-Contrast CT Head (NCCT): STAT! Differentiates ischemic vs. hemorrhagic.
⭐ Rapid NCCT head is crucial; "Time is Brain" - every minute, ~1.9 million neurons are lost in an untreated large vessel occlusion stroke.
Ischemic Stroke - Thrombolysis & Thrombectomy Triumph
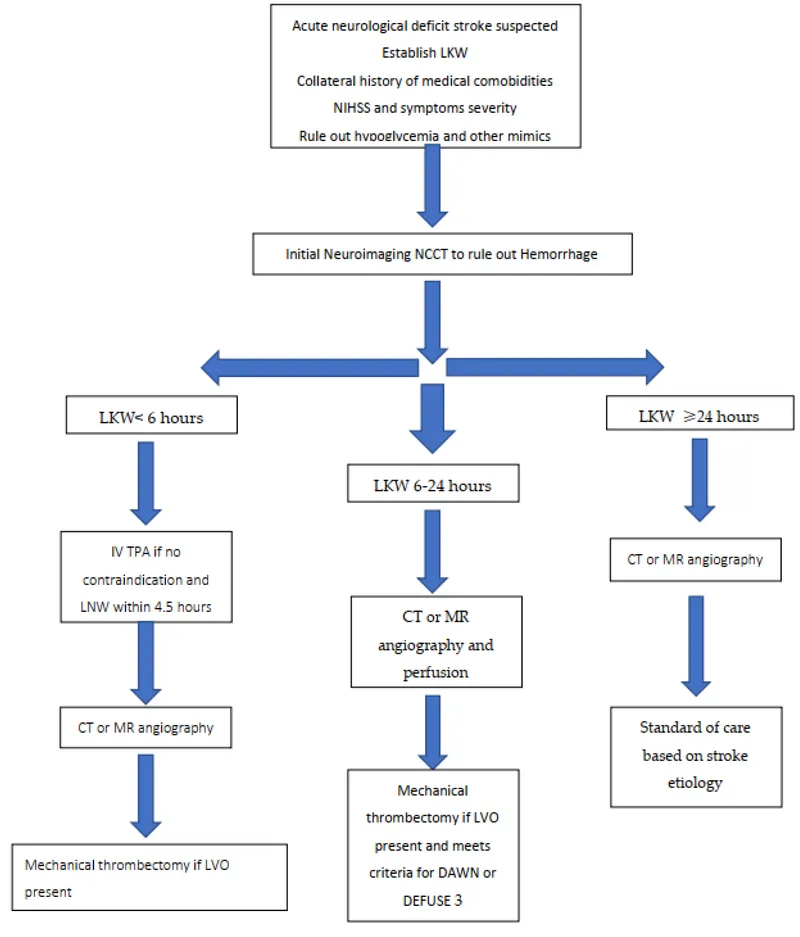
- Goal: Rapid reperfusion to salvage penumbra. 📌 "Time is Brain!"
- IV Thrombolysis (Alteplase - r-tPA):
- Window: <4.5 hours from LSO (Last Seen Normal).
- Dose: 0.9 mg/kg (max 90mg); 10% IV bolus, rest over 1 hr.
- BP target pre-Rx: <185/110 mmHg.
- Post-Rx BP target: <180/105 mmHg for 24h.
- ⚠️ Key CIs: Persistent BP >185/110, active bleed, recent major surgery/trauma, INR >1.7, Plt <100k, Glc <50/>400.
- Mechanical Thrombectomy (MT):
- Indication: LVO (Large Vessel Occlusion) in anterior circulation (ICA, MCA-M1/M2).
- Window: <6 hours; up to 24 hours for select patients (DAWN/DEFUSE-3).
- Often follows IV thrombolysis if eligible.
- Antiplatelets:
- Aspirin (160-325 mg) at 24-48h post-stroke (or 24h post-IVT).
- DAPT (Aspirin + Clopidogrel) for minor stroke (NIHSS ≤3-5)/TIA for 21-90 days.
⭐ The NINDS trial established IV tPA efficacy within 3 hours of ischemic stroke onset; ECASS-III extended this to 4.5 hours.
Hemorrhagic Stroke - Stop the Bleed Strategy
- Core Aims: Rapid BP control, reverse anticoagulation, manage Intracranial Pressure (ICP), neurosurgical consult.
- BP Management:
- Target SBP <140 mmHg (if SBP 150-220 mmHg).
- If SBP >220 mmHg, consider cautious reduction to SBP <160 mmHg.
- Agents: Labetalol, Nicardipine, Esmolol. ⚠️ Avoid vasodilators like nitroprusside (can ↑ICP).
- Anticoagulation Reversal:
- Warfarin: IV Vitamin K + Prothrombin Complex Concentrate (PCC) (preferred) or FFP. Target INR <1.4.
- DOACs: Idarucizumab (Dabigatran); Andexanet alfa (Rivaroxaban, Apixaban). PCC if specific agent unavailable.
- Heparin/LMWH: Protamine sulfate.
- ICP Control: Head elevation (30°), osmotic therapy (Mannitol, hypertonic saline), External Ventricular Drain (EVD) if hydrocephalus/significant Intraventricular Hemorrhage (IVH).
- Surgery: Hematoma evacuation for cerebellar hemorrhage >3 cm with neurological deterioration/brainstem compression, or supratentorial with significant mass effect.
⭐ For patients with intracerebral hemorrhage (ICH) on warfarin, reversal with 4-factor PCC is preferred over Fresh Frozen Plasma (FFP) due to faster International Normalized Ratio (INR) correction and lower volume administration.
Post-Stroke Care - Road to Recovery
- Supportive Care:
- ABCs, vitals, glucose (140-180 mg/dL), temperature control.
- Dysphagia screen, DVT prophylaxis.
- Manage complications (edema, seizures, infection).
- Secondary Prevention (Ischemic Stroke/TIA):
- Antiplatelets: Aspirin, Clopidogrel. DAPT (Aspirin + Clopidogrel) for 21 days (minor stroke/TIA).
- Anticoagulation for cardioembolic source (e.g., AFib).
- Statins: High-intensity (e.g., Atorvastatin 40-80mg) for all.
- BP target: <130/80 mmHg (long-term).
- Lifestyle modification.
- Rehabilitation:
- Early physiotherapy, occupational, speech therapy.
- Address motor, sensory, cognitive, communication deficits.
⭐ High-intensity statin (e.g., Atorvastatin 40-80mg) for all ischemic stroke patients for secondary prevention, reducing recurrence risk_._
High-Yield Points - ⚡ Biggest Takeaways
- Time is brain: Rapid reperfusion is paramount in acute stroke.
- IV Alteplase for ischemic stroke within 3-4.5 hours of symptom onset.
- Mechanical thrombectomy for LVO, window up to 24 hours in select cases.
- Immediate non-contrast CT head to exclude intracranial hemorrhage.
- BP goals: Permissive hypertension (≤185/110 mmHg) pre-thrombolysis; <180/105 mmHg post.
- Aspirin (160-325mg) within 24-48 hours (delay 24h post-Alteplase).
- NIHSS score assesses severity and guides treatment decisions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

