Topical Steroids: Intro & Action - Skin Soothers
- Synthetic analogs of natural corticosteroids; for localized skin inflammation & related conditions.
- Primary Actions:
- Anti-inflammatory: Inhibit Phospholipase A2 (↓ prostaglandins, leukotrienes). Bind Glucocorticoid Receptors (GREs) → alter gene expression. ↓ inflammatory cytokine release.
- Immunosuppressive: ↓ activity of lymphocytes & macrophages.
- Anti-proliferative: ↓ DNA synthesis & mitosis in epidermal cells.
- Vasoconstrictive: Reduces local blood flow & erythema.
⭐ Vasoconstriction (blanching) is a key mechanism of topical corticosteroids and forms the basis for potency assessment (e.g., Stoughton-McKenzie test).
Steroid Strength & Types - Potency Powerhouse
Topical corticosteroids grouped by potency; crucial for matching strength to condition & site.
- Potency Classes (US System):
- Class I (Superpotent): Clobetasol propionate 0.05%, Halobetasol 0.05%
- Class II (Potent): Fluocinonide 0.05%, Betamethasone dipropionate 0.05% (aug.)
- Class III (Upper Mid-Strength): Betamethasone valerate 0.1%
- Class IV (Mid-Strength): Triamcinolone acetonide 0.1% (cream/oint.)
- Class V (Lower Mid-Strength): Fluocinolone acetonide 0.01%
- Class VI (Mild): Desonide 0.05%, Alclometasone dipropionate 0.05%
- Class VII (Least Potent): Hydrocortisone 1%, 2.5%
📌 Mnemonic (Examples I→VII): "Clever Foxes Bring Tasty Fish During Harvest"
- Formulation & Potency: Potency ↑ with occlusive vehicles.
- Ointments (most potent) > Creams > Lotions > Gels > Solutions/Sprays (least potent).
- Occlusion (e.g., plastic wrap) ↑ absorption significantly (e.g., 10-100x).

⭐ Clobetasol propionate is a superpotent (Class I) topical corticosteroid, while hydrocortisone (1%) is a mild (Class VII) one.
Uses & Application - Skin Savers
- Key Indications:
- Eczemas (atopic, contact, seborrheic, discoid), Psoriasis (localized, non-plaque).
- Lichen Planus, Lichen Sclerosus, DLE, severe insect bites.
- Application Guidelines:
- Apply thinly 1-2 times/day; use Fingertip Unit (FTU) for quantity.
- Shortest effective duration; taper frequency or potency on improvement.
- Occlusion (e.g., under dressing) ↑ potency & absorption; use short-term, cautiously.
- Avoid on ulcerated or untreated infected skin (unless specific antimicrobial combo).
⭐ One Fingertip Unit (FTU) is the amount of ointment expressed from a tube with a 5mm nozzle onto the adult index finger from tip to DIP joint, approximately 0.5g, which covers an area of two adult hands.
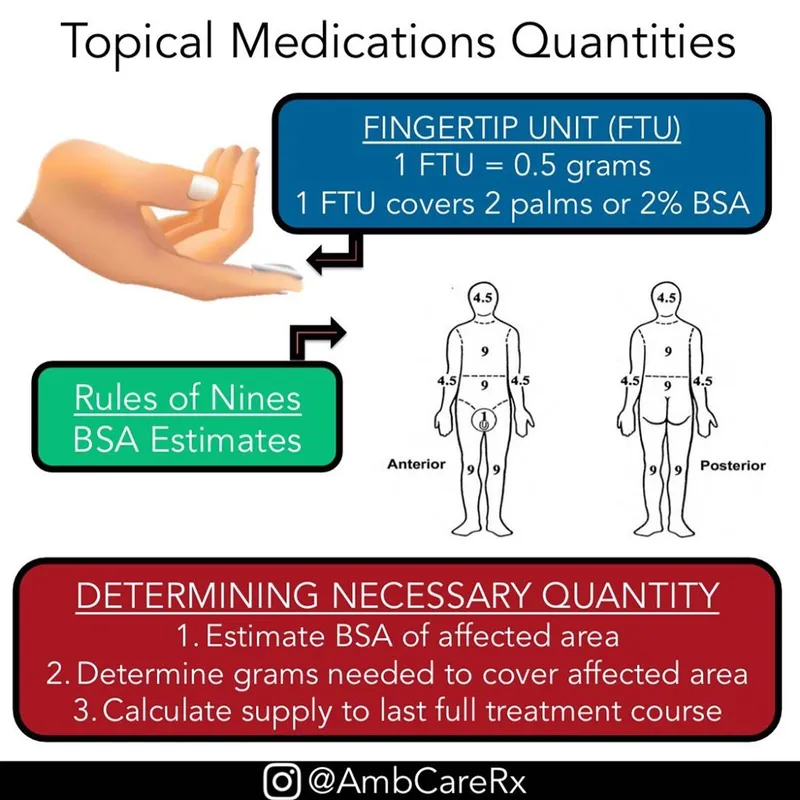 visual guide for topical steroid application)
visual guide for topical steroid application)
Side Effects & Cautions - Handle With Care

Local Side Effects:
- Skin atrophy (thinning, fragility, easy bruising) - most common
- Telangiectasia, striae, purpura
- Acneiform eruptions, rosacea, perioral dermatitis
- Hypopigmentation
- Delayed wound healing
- Tachyphylaxis (tolerance)
- Allergic contact dermatitis (to steroid or vehicle)
Systemic Side Effects (rare with low-medium potency; risk with high potency, large area, prolonged use, occlusion):
- Hypothalamic-Pituitary-Adrenal (HPA) axis suppression
- Cushing's syndrome
- Growth retardation (children)
- Hyperglycemia, glaucoma
Cautions/Contraindications:
- Untreated bacterial, fungal, or viral skin infections (e.g., herpes simplex, varicella zoster)
- Hypersensitivity
- Use potent steroids cautiously on face, intertriginous areas, and in children.
⭐ Skin atrophy, characterized by thinning, fragility, and easy bruising, is the most common and characteristic local side effect of prolonged topical corticosteroid use.
⚠️ Avoid abrupt withdrawal after prolonged use; taper gradually to prevent rebound phenomenon. 📌 Skin atrophy, Telangiectasia, Rosacea, Infections, Pigmentation changes, Epidermal thinning, Delayed healing (STRIPED) for local effects (partial mnemonic).
High‑Yield Points - ⚡ Biggest Takeaways
- Mechanism: Anti-inflammatory, immunosuppressive, anti-proliferative via glucocorticoid receptors.
- Potency classification (low to superpotent) guides selection; e.g., hydrocortisone (low), clobetasol (superpotent).
- Site matters: Low potency for face/groin; high potency for palms/soles.
- Side effects: Skin atrophy, striae, telangiectasias, tachyphylaxis, systemic absorption.
- Tachyphylaxis: Rapid ↓ in drug response with repeated use.
- Occlusion significantly ↑ absorption and potency.
- Avoid abrupt withdrawal of potent steroids to prevent rebound phenomenon.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

