Oral Anticoagulants - No Clot Zone Intro
- Drugs preventing/treating thromboembolic disorders (e.g., DVT, PE, AF).
- Administered orally, suitable for long-term anticoagulation.
- Major Classes:
- Vitamin K Antagonists (VKAs): e.g., Warfarin.
- Direct Oral Anticoagulants (DOACs):
- Direct Thrombin Inhibitors (DTIs): e.g., Dabigatran.
- Factor Xa Inhibitors: e.g., Rivaroxaban, Apixaban, Edoxaban.
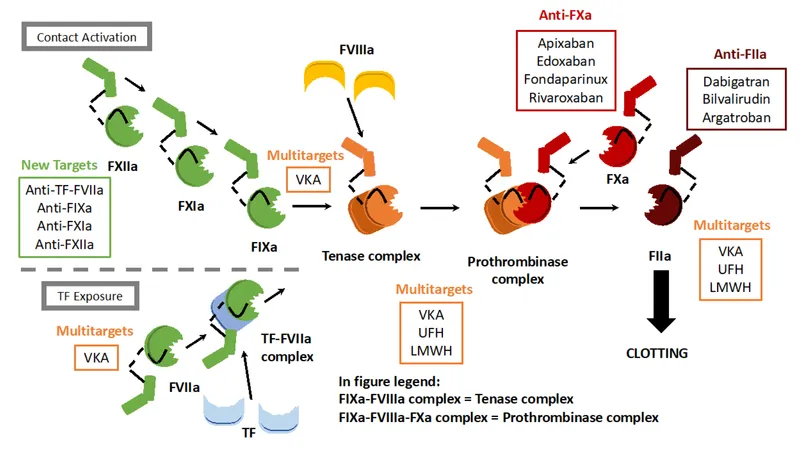
⭐ DOACs generally have a rapid onset of action, predictable anticoagulant effects, and fewer drug-food interactions compared to VKAs, often eliminating the need for routine monitoring (e.g., INR for warfarin).
Warfarin - Coumarin Kingpin
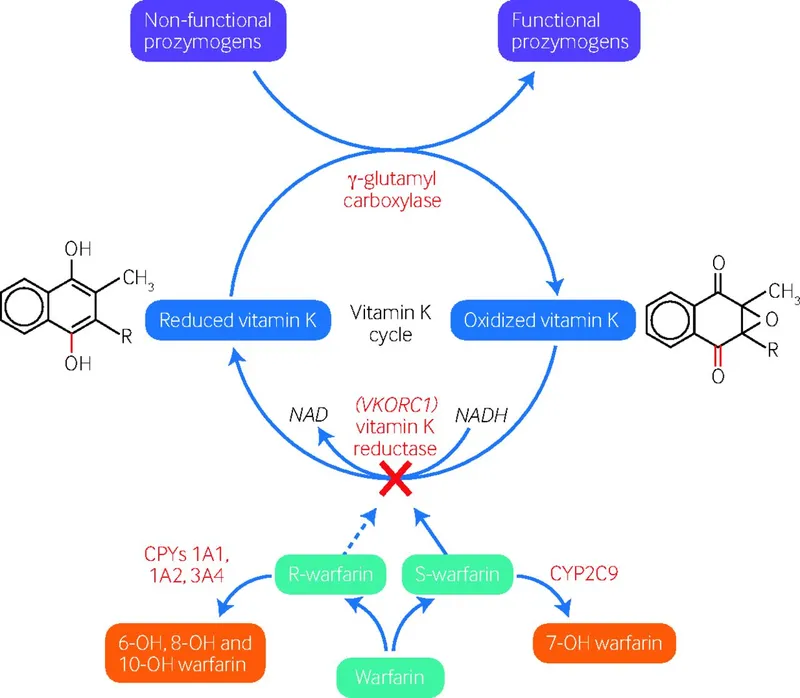
- Mechanism of Action (MOA): Inhibits Vitamin K epoxide reductase → ↓ synthesis of active Vitamin K-dependent clotting factors (II, VII, IX, X) and anticoagulant Proteins C & S.
- 📌 WEPT: Warfarin affects Extrinsic Pathway, monitored by PT/INR.
- Pharmacokinetics (PK):
- Oral; slow onset (8-12h), peak effect (36-72h); long half-life.
- Metabolized by CYP2C9 (genetic variability impacts dose).
- Crosses placenta: Teratogenic ⚠️ (Fetal Warfarin Syndrome - chondrodysplasia punctata).
- Monitoring: Prothrombin Time (PT) / International Normalized Ratio (INR).
- Target INR: 2.0-3.0 (most indications); 2.5-3.5 (e.g., mechanical heart valves).
- Interactions: Numerous! (e.g., antibiotics, antifungals, amiodarone, rifampicin, NSAIDs, leafy greens).
- Reversal of Anticoagulation:
- Stop Warfarin.
- Vitamin K1 (Phytonadione): Oral/IV; slow onset (6-24h).
- Rapid reversal (severe bleeding): Fresh Frozen Plasma (FFP) or Prothrombin Complex Concentrate (PCC).
- Adverse Effects (AEs):
- Bleeding (most common).
- Skin necrosis (initial hypercoagulable state due to ↓ Protein C; rare).
- Purple toe syndrome.
⭐ Warfarin's anticoagulant effect is delayed because it acts on the synthesis of new clotting factors, not on already circulating factors. An initial transient hypercoagulable state can occur due to faster inhibition of Protein C and S.
DOACs: Direct Thrombin Inhibitors - Dabi's Direct Hit
- Mechanism: Directly inhibits both free & clot-bound thrombin (Factor IIa).
- 📌 "Dabi's Direct Hit" on Thrombin.
- Drug: Dabigatran etexilate (oral prodrug).
- Key Features:
- Rapid onset (2-4 hrs).
- No routine coagulation monitoring needed.
- Fewer drug/food interactions vs. Warfarin.
- Predictable anticoagulant effect.
- Indications:
- Stroke prevention in Non-Valvular Atrial Fibrillation (NVAF).
- Treatment & secondary prevention of DVT/PE.
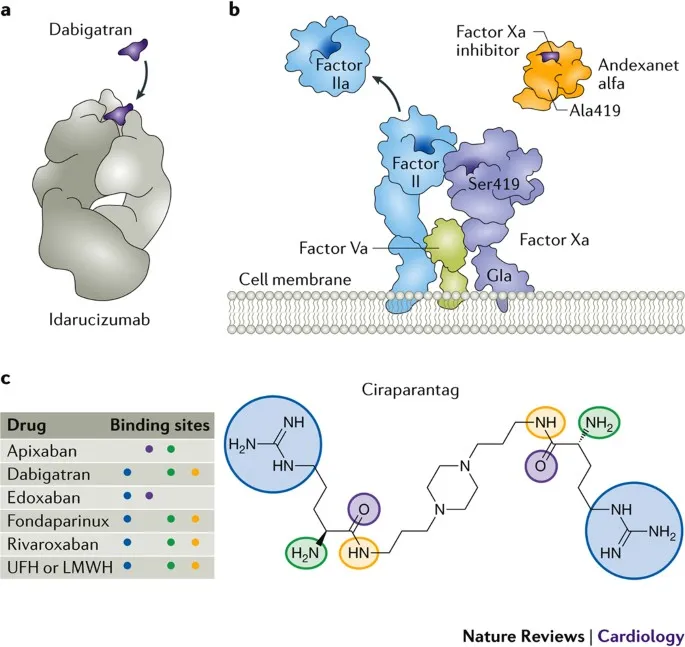
- Reversal Agent: Idarucizumab (Praxbind).
- Adverse Effects: Dyspepsia (common), bleeding.
- Elimination: Primarily renal (~80%); dose adjustment in renal impairment.
⭐ Idarucizumab is a humanized monoclonal antibody fragment that specifically binds to dabigatran and its acylglucuronide metabolites, neutralizing their anticoagulant effect rapidly.
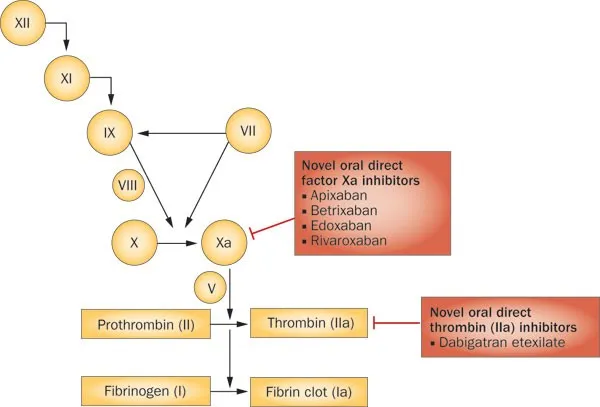
DOACs: Factor Xa Inhibitors - Xa's Hit Squad
- MOA: Directly bind & inhibit Factor Xa, ↓ thrombin generation. 📌 Suffix "-xaban" (e.g., Rivaroxaban, Apixaban, Edoxaban).
- Advantages vs. Warfarin: Rapid onset, predictable pharmacokinetics, fixed dosing, no routine INR monitoring, fewer drug/food interactions.
- Indications:
- Stroke prevention in Non-Valvular Atrial Fibrillation (NVAF).
- Treatment & secondary prophylaxis of Deep Vein Thrombosis (DVT) & Pulmonary Embolism (PE).
- Key Clinical Points:
- Bleeding is the major side effect.
- Reversal agent: Andexanet alfa.
- Renal dose adjustment required for most (check CrCl).
- Rivaroxaban: doses ≥15 mg should be taken with food.
- Apixaban: often preferred in moderate CKD & elderly due to potentially lower bleeding risk.
⭐ Andexanet alfa is a specific antidote for rivaroxaban and apixaban, acting as a recombinant modified human Factor Xa decoy protein that binds and sequesters these inhibitors.
High‑Yield Points - ⚡ Biggest Takeaways
- Warfarin: Vitamin K antagonist (Factors II, VII, IX, X, C, S). Monitor INR (target 2-3). Teratogenic.
- Antidotes for Warfarin: Vitamin K (slow), FFP/PCC (rapid).
- DOACs (Dabigatran, Rivaroxaban, Apixaban): Rapid onset, fixed dose, no routine monitoring.
- Dabigatran: Direct thrombin (IIa) inhibitor. Antidote: Idarucizumab.
- Rivaroxaban/Apixaban: Direct Factor Xa inhibitors. Antidote: Andexanet alfa.
- Warfarin needs bridging due to initial Protein C & S drop.
- DOACs: ↓ ICH risk vs Warfarin; some ↑ GI bleed risk. Costlier.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

