Heparins - Clot Busters Classic
- Mechanism: Potentiate Antithrombin III (ATIII).
- Unfractionated Heparin (UFH):
- Via ATIII: inactivates Thrombin (IIa) & Factor Xa (1:1).
- Monitor: aPTT (1.5-2.5x control).
- Reversal: Protamine Sulfate.
- ⚠️ Risk: Heparin-Induced Thrombocytopenia (HIT).
- Low Molecular Weight Heparins (LMWHs): (e.g., Enoxaparin, Dalteparin)
- Via ATIII: Xa > IIa inhibition.
- Monitor: Anti-Xa assay (usually not needed).
- Reversal: Protamine Sulfate (partial).
- ↓ HIT risk vs UFH.
- Fondaparinux:
- Synthetic pentasaccharide; Via ATIII: selectively inhibits Factor Xa.
- No routine monitoring; no reversal agent.
- Minimal HIT risk.
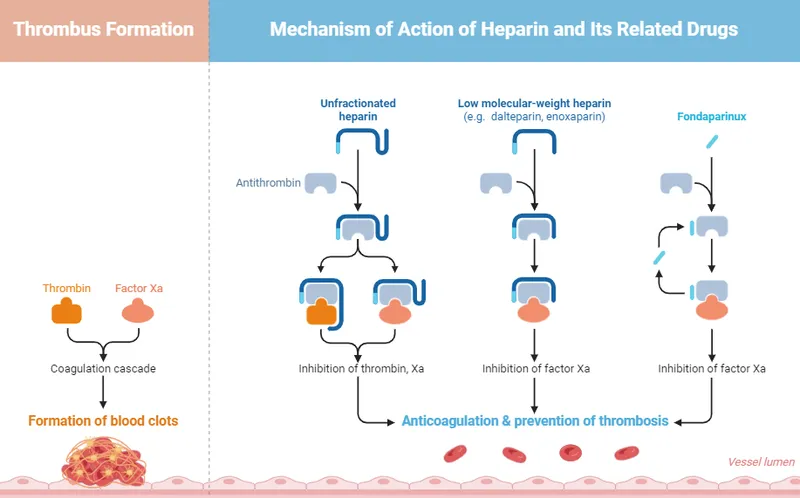
⭐ UFH acts via antithrombin to inhibit factors IIa (thrombin) and Xa almost equally. LMWHs preferentially inhibit Factor Xa over IIa (approx. 2-4:1 ratio). Fondaparinux selectively inhibits only Factor Xa via antithrombin activation.
Direct Thrombin Inhibitors - Thrombin Tamers
Directly bind to and inhibit thrombin (Factor IIa), preventing fibrin formation. Independent of antithrombin; act on free & clot-bound thrombin.
- Parenteral DTIs:
- Bivalirudin: Rapid onset, short half-life. Use: PCI. Monitor: ACT/aPTT.
- Argatroban: Hepatic metabolism. Use: HIT (especially with renal impairment). Monitor: aPTT.
- Oral DTI:
- Dabigatran Etexilate: Prodrug.
- Uses: Stroke prevention in non-valvular AF, VTE treatment/prophylaxis.
- Reversal: Idarucizumab.
- AEs: Bleeding, dyspepsia.
- 📌 "DABigatran directly ATTACKS thrombin."
- Dabigatran Etexilate: Prodrug.
⭐ Argatroban is preferred for HIT in patients with renal dysfunction as it undergoes hepatic metabolism, unlike lepirudin (renal excretion).
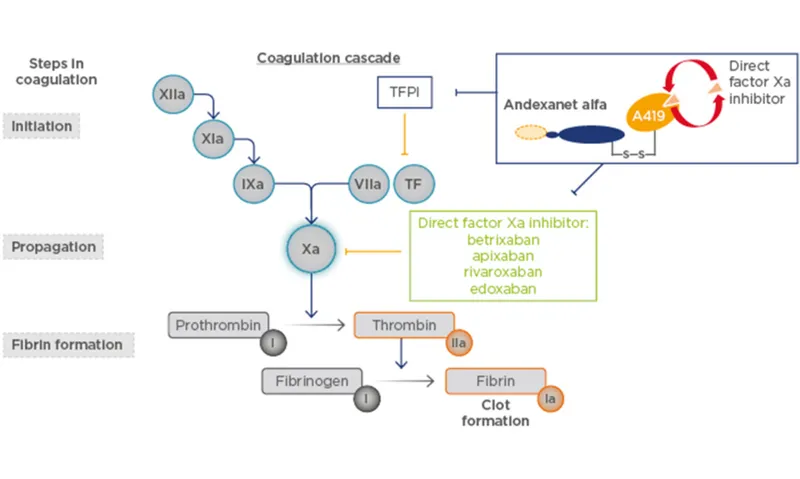
Direct Factor Xa Inhibitors - Xa Zappers
Oral anticoagulants directly inhibiting Factor Xa. Common suffix "-xaban".
- Agents: Rivaroxaban, Apixaban, Edoxaban, Betrixaban.
- 📌 Mnemonic: "-xa-ban" indicates Xa inhibition.
- Mechanism: Directly bind to active site of Factor Xa (free & clot-bound).
- Blocks conversion of prothrombin to thrombin.
- Key Features:
- Oral, fixed dosing.
- Predictable effect, no routine INR monitoring.
- Rapid onset/offset.
- Uses:
- DVT/PE treatment & prophylaxis.
- Stroke prevention in non-valvular Atrial Fibrillation (NVAF).
- Side Effects: Bleeding (main concern).
- Antidote: Andexanet alfa (for rivaroxaban, apixaban).
- Caution: Renal impairment (dose adjustment/avoid).
⭐ Rivaroxaban (≥15 mg doses) should be taken with food for optimal absorption; apixaban can be taken with or without food.
Anticoagulant Crossroads - Clinical Choices & Cautions
- Choice by Condition:
- Pregnancy: LMWH (safe). Warfarin (X: teratogenic), DOACs (avoid).
- Renal Impairment (CrCl < 30 mL/min): UFH (esp. if CrCl < 15 mL/min), adjust LMWH/DOACs; Warfarin usable.
- Heparin-Induced Thrombocytopenia (HIT): STOP heparins! Use Argatroban, Bivalirudin, Fondaparinux.
- Mechanical Valves: Warfarin. NVAF: DOACs preferred.
- Reversal Agents:
- Heparin/LMWH: Protamine Sulfate.
- Warfarin: Vit K (slow), PCC/FFP (rapid).
- Dabigatran (DTI): Idarucizumab.
- Factor Xa Inhibitors: Andexanet Alfa; PCC.
- Monitoring:
- UFH: aPTT. LMWH: Anti-Xa (select cases). Warfarin: PT/INR (target 2-3; 2.5-3.5 for high-risk valves). DOACs: Generally no routine monitoring.
- Warfarin Interactions: High risk. Affected by CYP2C9 inhibitors (e.g., Amiodarone ↑INR) & inducers (e.g., Rifampin ↓INR), antibiotics, diet (Vitamin K).
⭐ For patients on Warfarin requiring urgent surgery, reversal with Prothrombin Complex Concentrate (PCC) is faster than FFP and Vitamin K alone.
High‑Yield Points - ⚡ Biggest Takeaways
- UFH acts via Antithrombin III on Factors Xa & IIa; monitor aPTT. LMWH mainly targets Factor Xa via AT-III.
- Protamine sulfate reverses heparin. Heparin-Induced Thrombocytopenia (HIT) is a critical risk.
- Direct Thrombin Inhibitors (e.g., oral Dabigatran) directly block thrombin (IIa).
- Direct Factor Xa Inhibitors (e.g., oral Rivaroxaban, Apixaban) directly block Factor Xa.
- DOACs offer fixed dosing, predictable effects, and no routine monitoring.
- Antidotes: Idarucizumab for Dabigatran; Andexanet alfa for Xa inhibitors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

