Mechanisms: Overview - Med Mixology 101
- Drug Interaction (DI): Drug's effect modified by another substance (drug, food, herb).
- Primary Mechanisms:
- Pharmacokinetic (PK): Body's action on drug altered ("ADME").
- Absorption: e.g., Chelation, pH changes.
- Distribution: Protein binding displacement.
- Metabolism: CYP450 enzyme induction/inhibition.
- Excretion: Altered renal/biliary clearance.
- Pharmacodynamic (PD): Drug's action on body modified.
- Receptor interactions (synergism, antagonism).
- Post-receptor effects.
- Pharmaceutical: Physical/chemical incompatibility (e.g., IV admixtures).
- Pharmacokinetic (PK): Body's action on drug altered ("ADME").
- Key Outcomes: ↑Toxicity or ↓Efficacy.
⭐ Most clinically significant drug interactions involve alterations in drug metabolism via CYP450 enzyme induction or inhibition (Pharmacokinetic).
Mechanisms: PK (AD) - Entry & Spread Sabotage
- Absorption (Entry Sabotage)
- Altered Gastric pH:
- Antacids (↑pH) ↓ absorption of acidic drugs (e.g., ketoconazole, iron).
- Acidic environment (stomach) favors acidic drug absorption.
- Chelation/Complexation:
- Tetracyclines, Fluoroquinolones + Ca²⁺, Mg²⁺, Fe²⁺/³⁺, Al³⁺ (in antacids, dairy, iron preps) → ↓ absorption. 📌 "TFs bind Cations" (Tetracyclines, Fluoroquinolones bind Cations).
- Altered Gut Motility:
- Prokinetics (e.g., metoclopramide): ↑ motility → ↓ absorption of slowly absorbed drugs (e.g., digoxin); ↑ for rapidly absorbed (e.g., paracetamol).
- Anticholinergics: ↓ motility → opposite effects.
- P-glycoprotein (P-gp) Efflux Pump Modulation:
- Inducers (e.g., rifampicin): ↑ P-gp efflux → ↓ absorption of substrates (e.g., digoxin).
- Inhibitors (e.g., verapamil): ↓ P-gp efflux → ↑ absorption of substrates (e.g., digoxin).
- Altered Gastric pH:
- Distribution (Spread Sabotage)
- Protein Binding Displacement:
- Highly protein-bound drugs (e.g., warfarin, phenytoin, sulfonamides) can displace each other from albumin.
- Aspirin displaces warfarin → ↑ free warfarin → ↑ bleeding risk.
- ⭐ > Displacement is clinically significant mainly for drugs with >90% protein binding, small Volume of Distribution (Vd), and narrow therapeutic index.
- Altered Tissue Uptake/Binding:
- Digoxin + Quinidine: Quinidine displaces digoxin from tissue binding sites & inhibits P-gp → ↑ plasma digoxin levels → toxicity.
- Protein Binding Displacement:
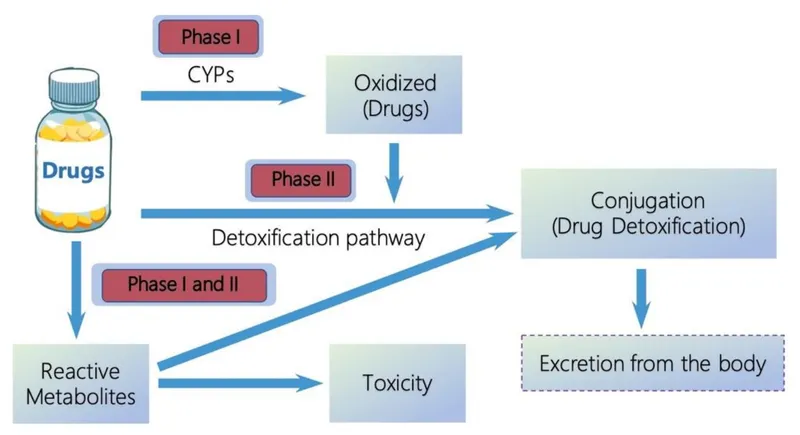
Mechanisms: PK (ME) - Metabolism & Exit Mayhem
Metabolism (Biotransformation): Primarily hepatic; alters drug structure.
- Enzyme Induction: ↑Metabolism. Effect: ↓Drug levels/failure or ↑Toxic metabolite. Onset: Slow.
- 📌 Inducers: CRAP GPS (Carbamazepine, Rifampicin, Alcohol (chronic), Phenytoin, Griseofulvin, Phenobarbitone, Sulfonylureas/Smoking/St. John's Wort).
- Enzyme Inhibition: ↓Metabolism. Effect: ↑Drug levels/toxicity. Onset: Rapid.
- 📌 Inhibitors: SICKFACES.COM Group (Sodium valproate, Isoniazid, Cimetidine, Ketoconazole, Fluconazole, Alcohol (acute), Chloramphenicol, Erythromycin, Sulfonamides, Ciprofloxacin, Omeprazole, Metronidazole, Grapefruit juice).
- CYP450: Main system; CYP3A4 for ~50% drugs. Genetic variants (CYP2D6, CYP2C19) → varied response.
⭐ Grapefruit juice (CYP3A4 inhibitor) ↑ levels & toxicity of statins, Calcium channel blockers, cyclosporine.
Excretion (Elimination): Primarily renal.
- Renal:
- Filtration: unbound drug.
- Secretion: active; competition (Probenecid + Penicillin → ↑Penicillin).
- Reabsorption: pH-dependent ion trapping.
- Acidic drugs (Aspirin): Alkalinize urine (NaHCO₃) for ↑Excretion.
- Basic drugs (Amphetamine): Acidify urine (NH₄Cl) for ↑Excretion.
- Biliary & Enterohepatic Circulation:
- Bile excretion, gut reabsorption → prolongs action (Digoxin, OCPs).
- Antibiotics may ↓ OCP efficacy.
Mechanisms: PD - Target Site Tussles
- Drugs interact at same/related target sites, altering cellular/physiological response.
- Receptor Site Competition:
- Competitive Antagonism: Naloxone (antagonist) displaces morphine (agonist) at µ-opioid receptors.
- Partial vs. Full Agonist: Buprenorphine (partial agonist) can ↓ efficacy of morphine (full agonist) if co-administered.
- Allosteric Modulation:
- Drugs bind to different sites on one receptor complex, modifying the primary ligand's effect.
- E.g., Benzodiazepines & Barbiturates on GABA-A receptor (enhance GABAergic inhibition, ↑Cl⁻ influx).
- Physiological (Functional) Antagonism:
- Two drugs act on different receptors/pathways, producing opposing physiological effects on the same system.
- E.g., Histamine (H1; bronchoconstriction) vs. Adrenaline (β2; bronchodilation).
⭐ Co-administration of Sumatriptan (5-HT1D agonist) and Ergotamine derivatives is contraindicated due to synergistic vasoconstriction (risk of severe coronary/cerebral ischemia); allow at least a 24-hour interval between them.
High‑Yield Points - ⚡ Biggest Takeaways
- Pharmacokinetic (PK) interactions alter drug ADME (Absorption, Distribution, Metabolism, Excretion).
- Pharmacodynamic (PD) interactions at target sites: synergism, antagonism, additive effects.
- CYP450 enzyme induction (e.g., rifampicin) ↓ drug levels, reducing efficacy.
- CYP450 enzyme inhibition (e.g., ketoconazole) ↑ drug levels, increasing toxicity risk.
- P-glycoprotein (P-gp) modulation impacts drug absorption and cellular efflux.
- Altered absorption: chelation (e.g., tetracyclines + antacids) or pH changes reduce bioavailability.
- Protein binding displacement (e.g., warfarin by NSAIDs) ↑ free drug concentration and effect.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

