Interaction Foundations - PK/PD Tango
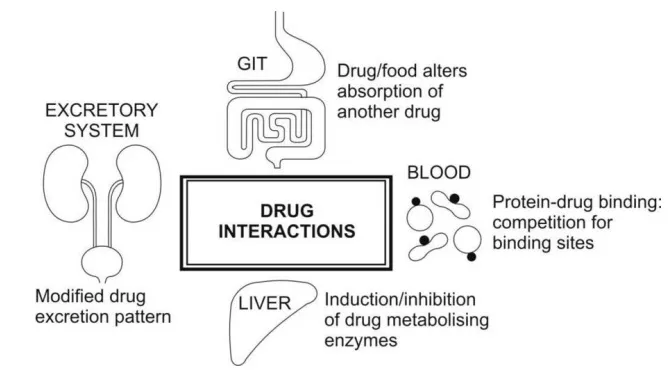
- Pharmacokinetic (PK) Interactions: Body's handling of one drug altered by another, affecting ADME:
- Absorption: e.g., altered GI pH, chelation.
- Distribution: e.g., protein binding displacement.
- Metabolism: Enzyme induction (e.g., Rifampicin ↓ warfarin) or inhibition (e.g., Erythromycin ↑ warfarin).
- Excretion: e.g., altered renal tubular secretion.
- Pharmacodynamic (PD) Interactions: One drug's effect at target site modified by another.
- Synergism: Enhanced effect (additive, potentiation).
- Antagonism: Reduced effect (competitive, non-competitive).
⭐ CYP450 enzyme interactions are the most common cause of PK drug interactions.
CYP450 Interactions - Metabolic Mayhem Makers
Cytochrome P450 (CYP450) enzymes in the liver are vital for drug metabolism. Their modulation causes significant drug-drug interactions (DDIs), impacting drug levels. Key enzymes: CYP3A4 (major), CYP2D6, CYP2C9, CYP1A2.
Common CYP450 Modulators
| Type | Effect on Substrate Drug | Examples | Mnemonic |
|---|---|---|---|
| Inducers | ↓ Drug levels (therapy failure) | Rifampicin, Carbamazepine, Phenytoin, Phenobarbital, St. John's Wort | 📌 CRAP GPS |
| Inhibitors | ↑ Drug levels (toxicity risk) | Macrolides (e.g., Erythromycin), Azole antifungals (e.g., Ketoconazole), Grapefruit juice, Protease inhibitors, Cimetidine, Amiodarone | 📌 SICKFACES.COM |
Key Problem Pairs - Danger Duos Alert
- Warfarin + NSAIDs/Amiodarone/Metronidazole/CYP modifiers → ↑Bleeding risk; Monitor INR.
- Digoxin + Diuretics/Verapamil/Amiodarone/Clarithromycin → ↑Digoxin toxicity (arrhythmias, GI, visual disturbances).
- Statins + CYP3A4 inhibitors (Macrolides, Azoles, Grapefruit) → ↑Myopathy/Rhabdomyolysis.
- MAOIs + Tyramine foods/SSRIs/TCAs/Sympathomimetics → Hypertensive crisis/Serotonin syndrome.
- SSRIs + MAOIs/Triptans/Tramadol → Serotonin Syndrome (agitation, hyperthermia, clonus).
- Methotrexate + NSAIDs/Penicillins/Probenecid → ↑MTX toxicity (myelosuppression, mucositis).
- Lithium + Thiazides/NSAIDs/ACE inhibitors → ↑Lithium toxicity (tremor, ataxia, confusion).
⭐ Grapefruit juice is a potent inhibitor of CYP3A4, significantly increasing levels of drugs like statins (e.g., Simvastatin, Atorvastatin), calcium channel blockers, and some immunosuppressants, leading to increased risk of toxicity.
ADME Mechanisms - ADME Antagonists
- Absorption Interactions:
- Chelation: Tetracycline + Antacids (↓ absorption).
- pH change: Ketoconazole + PPIs (↓ absorption).
- Motility: Metoclopramide (↑ absorption rate), Opioids (↓ rate).
- Distribution Interactions:
- Protein displacement: Warfarin + Sulfonamides (↑ free Warfarin).
- Excretion Interactions (Renal):
- Tubular secretion competition: Probenecid + Penicillin (↑ Penicillin levels).
- Urine pH change: Alkalinize urine for Salicylate OD (↑ excretion).
⭐ Probenecid competitively inhibits renal tubular secretion of Penicillin, prolonging its half-life and increasing its efficacy for certain infections.
High‑Yield Points - ⚡ Biggest Takeaways
- CYP450 modulators: Inducers (Rifampicin) ↓ drug levels; Inhibitors (Azoles, Macrolides) ↑ levels & toxicity.
- Warfarin: High risk with antibiotics, NSAIDs, Amiodarone (↑ bleeding).
- Digoxin: Toxicity ↑ by hypokalemia (diuretics), Amiodarone, Verapamil.
- Statins + CYP3A4 inhibitors (Macrolides, Azoles) = ↑ myopathy risk.
- MAOIs: Tyramine foods → hypertensive crisis; SSRIs → serotonin syndrome.
- Serotonin Syndrome: Risk with multiple serotonergic drugs (SSRIs, TCAs, Tramadol).
- QT Prolongation: Additive risk with Macrolides, Fluoroquinolones, Class III antiarrhythmics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

