Thiazide Diuretics - Pressure Plungers
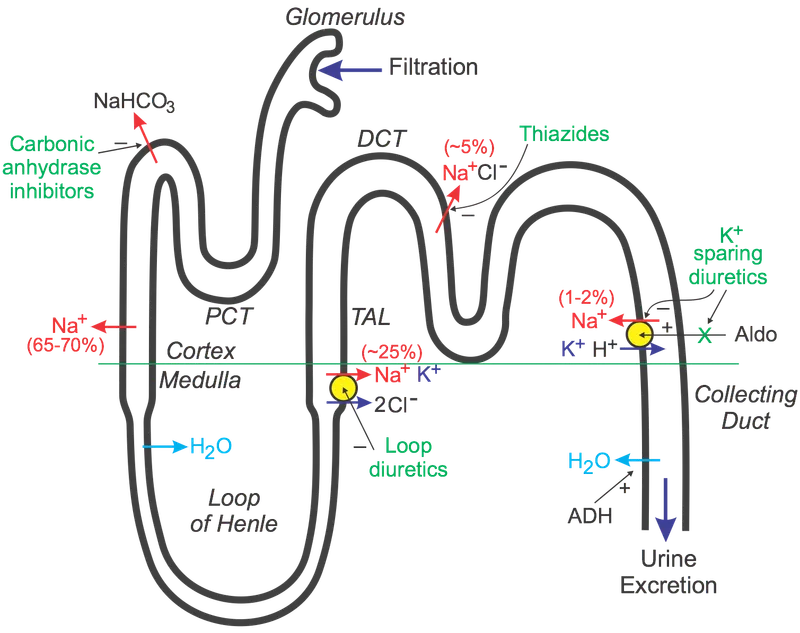
- Mechanism (MOA): Inhibit Na⁺-Cl⁻ cotransporter (NCC) in early Distal Convoluted Tubule (DCT).
- Results in ↑ Na⁺, Cl⁻, K⁺, Mg²⁺ excretion.
- Conversely, ↓ Ca²⁺ excretion (can lead to hypercalcemia).
- Key Drugs:
- Hydrochlorothiazide (HCTZ): Common, shorter acting.
- Chlorthalidone: Longer half-life, often preferred for sustained BP control.
- Indapamide: Vasodilatory properties; less adverse metabolic effects.
- Hypertension Role: First-line therapy, especially for uncomplicated HTN, elderly, and African-American patients. Effective in salt-sensitive hypertension.
- Added benefit: Slows demineralization in osteoporosis due to ↓ Ca²⁺ excretion.
- Adverse Effects: 📌 "HyperGLUC": HyperGlycemia, HyperLipidemia, HyperUricemia (can precipitate gout), HyperCalcemia.
- Also: HypoKalemia (⚠️ risk of arrhythmias), Hyponatremia, HypoMagnesemia.
- Sulfa allergy cross-reactivity.
⭐ Thiazides may lose efficacy when Glomerular Filtration Rate (GFR) falls below 30 mL/min (except Metolazone).
 oka
oka
Loop & K+-Sparing Diuretics - Electrolyte Experts
-
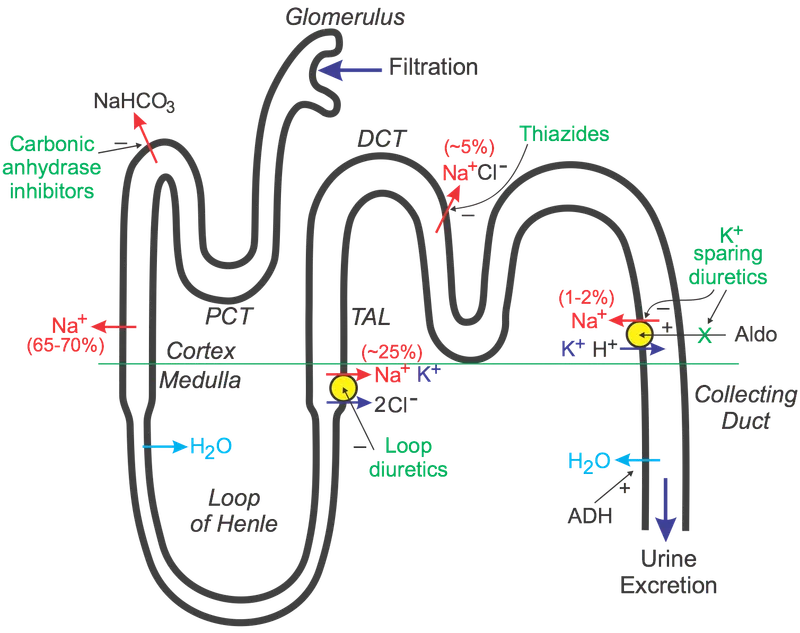
Loop Diuretics (e.g., Furosemide, Torsemide):
- MoA: Inhibit Na+-K+-2Cl- symporter in thick ascending limb (TAL). Potent.
- HTN Use:
- Emergencies, fluid overload (HF, CKD).
- Resistant HTN.
- Effective if GFR < 30 mL/min.
- Electrolytes: ↓K+, ↓Mg2+, ↓Ca2+ (chronic); metabolic alkalosis.
- ADRs: Ototoxicity, hyperuricemia, hypovolemia.
-
K+-Sparing Diuretics:
- Aldosterone Antagonists (e.g., Spironolactone, Eplerenone):
- MoA: Block aldosterone receptors (late DCT/CD).
- HTN Use: Resistant HTN (esp. ↑aldosterone), HF.
- ADRs: Hyperkalemia, gynecomastia (spironolactone).
- ENaC Inhibitors (e.g., Amiloride, Triamterene):
- MoA: Block ENaC (late DCT/CD).
- HTN Use: Combo to prevent ↓K+.
- ADRs: Hyperkalemia.
- Aldosterone Antagonists (e.g., Spironolactone, Eplerenone):
⭐ Spironolactone is key for resistant hypertension, especially with suspected hyperaldosteronism.
Clinical Application & Guidelines - Diuretic Strategy
- First-line: Thiazides (e.g., Chlorthalidone, Hydrochlorothiazide) for most uncomplicated hypertension.
- Chlorthalidone often preferred: longer duration, better 24-hr BP control.
- Specific Conditions:
- CKD (eGFR < 30 mL/min/1.73$m^2$), Heart Failure: Loop diuretics (e.g., Furosemide).
- Resistant Hypertension, Primary Aldosteronism: $K^+$-sparing (Spironolactone, Eplerenone).
- Gout: Avoid thiazides; consider alternatives.
- Osteoporosis: Thiazides (↓ $Ca^{2+}$ excretion).
- Combination Therapy:
- Preferred: Diuretic + ACEi/ARB (e.g., "A+D" strategy).
- Diuretic + CCB.
- Guidelines (JNC8, ACC/AHA, IGH): Emphasize thiazides as initial/adjunctive therapy.
⭐ Chlorthalidone is generally preferred over hydrochlorothiazide for hypertension management due to its longer half-life and superior evidence for cardiovascular risk reduction.
Adverse Effects & Monitoring - Safety Net
- Thiazides (HCTZ, Chlorthalidone):
- ↓$K^+$, ↓$Na^+$, ↑$Ca^{2+}$, ↑uric acid, ↑glucose, ↑lipids.
- Sulfa allergy. Ineffective if GFR < 30 mL/min.
- Loop Diuretics (Furosemide):
- ↓$K^+$, ↓$Na^+$, ↓$Mg^{2+}$, ↓$Ca^{2+}$, ↑uric acid.
- Ototoxicity (esp. rapid IV). Sulfa allergy.
- $K^+$-Sparing:
- Spironolactone: ↑$K^+$, gynecomastia.
- Amiloride: ↑$K^+$.
- Monitoring:
- BP, electrolytes ($K^+$, $Na^+$), renal function (BUN, Cr).
- Glucose, uric acid, lipids (for thiazides/loops).
- Interactions:
- NSAIDs: ↓ diuretic effect.
- Lithium: ↑ toxicity.
- Digoxin: ↑ toxicity with ↓$K^+$.
- ACEi/ARBs + $K^+$-sparing: risk of severe ↑$K^+$.
⭐ Thiazides cause hypercalcemia; Loop diuretics cause hypocalcemia.
High‑Yield Points - ⚡ Biggest Takeaways
- Thiazides (e.g., Chlorthalidone) are first-line for uncomplicated hypertension; act on Na-Cl cotransporter in DCT.
- Chlorthalidone is preferred over HCTZ for longer action and proven CVD risk reduction.
- Key adverse effects: Hypokalemia, hyponatremia, hyperuricemia, hyperglycemia.
- Loop diuretics (e.g., Furosemide) for hypertension with renal insufficiency (GFR < 30) or HF.
- K+-sparing diuretics (e.g., Spironolactone) counter thiazide-induced hypokalemia or for resistant HTN.
- Spironolactone specific risks: gynecomastia, hyperkalemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

