General Diuretic AEs - Fluid & Lytes Gone Wild
- Hemodynamic:
- Hypovolemia → ↓ perfusion, azotemia.
- Hypotension (orthostatic), dizziness.
- Electrolyte Disturbances:
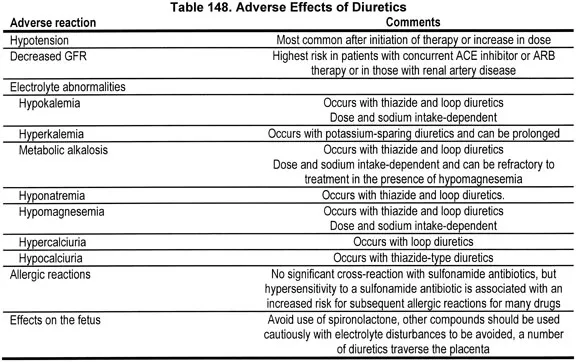
- Hyponatremia (↓Na⁺): Common with thiazides in elderly.
- Hypokalemia (↓K⁺): Weakness, arrhythmias (Loops, Thiazides).
- Hyperkalemia (↑K⁺): K⁺-sparing diuretics, ACEIs.
- Hypomagnesemia (↓Mg²⁺): Tetany, arrhythmias (Loops, Thiazides).
- Calcium: ↓Ca²⁺ (Loops); ↑Ca²⁺ (Thiazides).
- Acid-Base Imbalances:
- Metabolic Alkalosis (Loops & Thiazides).
- Metabolic Acidosis (CAIs, K⁺-sparing).
- Metabolic & Other:
- Hyperuricemia → Gout (Thiazides > Loops).
- Hyperglycemia, glucose intolerance (Thiazides, Loops).
- Dyslipidemia: ↑LDL, ↑TG (Thiazides).
- Ototoxicity (IV Loops).
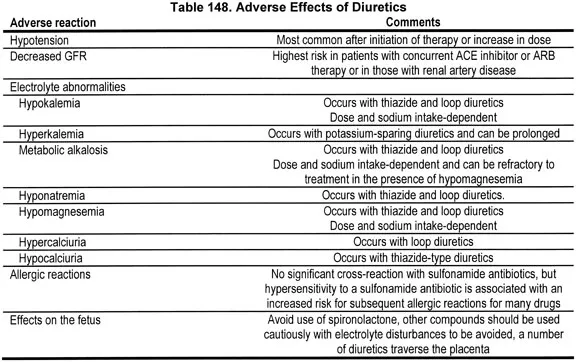
⭐ Diuretic-induced hyponatremia is particularly common and concerning in elderly patients taking thiazides; can cause confusion/seizures.
Loop & Thiazide AEs - Ouch, Sugar, Gout!
| Adverse Effect | Loop Diuretics (e.g., Furosemide) | Thiazide Diuretics (e.g., Hydrochlorothiazide) |
|---|---|---|
| Electrolytes | ↓K+, ↓Na+, ↓Cl- | ↓K+, ↓Na+, ↓Cl- |
| ↓Ca++, ↓Mg++ | ↑Ca++ | |
| Metabolic | ↑Uric acid (Gout) | ↑Glucose (Hyperglycemia) |
| ↑Lipids (Hyperlipidemia) | ||
| ↑Uric acid (Gout) | ||
| Ototoxicity | Yes (dose-related) | No |
| Sulfa Allergy | Yes (most) | Yes |
⭐ Ethacrynic acid, a loop diuretic, is an option for patients with sulfa allergy but carries a higher risk of ototoxicity.
Key Interactions:
- NSAIDs: ↓ diuretic effect.
- Aminoglycosides (with Loops): ↑ ototoxicity.
- Digoxin: ↑ toxicity if hypokalemia.
- Lithium: ↓ clearance, ↑ toxicity (especially Thiazides).
K-Sparing & Other AEs - HyperK & Odd Jobs
- K-Sparing Diuretics:
- Hyperkalemia (Serum K+ > 5.5 mEq/L): Most significant; risk ↑ with ACEi/ARBs, NSAIDs, renal insufficiency.
- Spironolactone:
- Antiandrogenic effects: Gynecomastia (can be painful), menstrual irregularities, impotence.
⭐ Spironolactone-induced painful gynecomastia is a common reason for non-compliance.
- Amiloride & Triamterene:
- Metabolic acidosis (Type 4 RTA-like, due to ↓ H+ secretion).
- Triamterene: Blue fluorescence in urine, nephrolithiasis (poorly soluble), megaloblastic anemia (folate antagonist).
- Osmotic Diuretics (e.g., Mannitol):
- Initial: ECF volume expansion (⚠️ can precipitate pulmonary edema in HF patients).
- Later: Dehydration, electrolyte imbalances (hypernatremia, hyponatremia, hypokalemia).
- Headache, nausea, vomiting.
- Carbonic Anhydrase Inhibitors (CAIs - e.g., Acetazolamide):
- Metabolic acidosis (non-anion gap, due to renal HCO₃⁻ wasting).
- Hypokalemia (due to ↑ K+ secretion in distal nephron).
- Renal stones (calcium phosphate, from ↑ urinary pH & ↑ phosphate excretion).
- Paresthesias, drowsiness, tinnitus.
- Sulfa allergy (cross-reactivity).
Diuretic Drug Interactions - Risky Mixes
Key interactions to monitor for enhanced toxicity or reduced efficacy:
| Diuretic Class / General | Interacting Drug | Consequence |
|---|---|---|
| All Diuretics | NSAIDs | ↓ Diuretic efficacy, ↑ risk of renal failure. |
| All Diuretics | ACEi / ARBs | Risk of severe hypotension; Hyperkalemia (critical with K+-sparing). |
| All Diuretics | Digoxin | ↑ Digoxin toxicity (secondary to hypokalemia/hypomagnesemia). |
| All Diuretics | Lithium | ↑ Lithium toxicity (due to reduced renal excretion of Li+). |
| Loop Diuretics | Aminoglycosides | Synergistic ↑ ototoxicity & nephrotoxicity. |
| Thiazides | Dofetilide | ↑ Risk of Torsades de Pointes (QT prolongation from hypokalemia). |
High‑Yield Points - ⚡ Biggest Takeaways
- Loop and Thiazide diuretics commonly cause hypokalemia and metabolic alkalosis.
- Potassium-sparing diuretics can lead to hyperkalemia, especially with ACE inhibitors or ARBs.
- Loop diuretics (e.g., furosemide) carry a risk of ototoxicity, worsened by aminoglycosides.
- Thiazides are associated with hyperuricemia, hyperglycemia, and hyperlipidemia.
- NSAIDs can reduce the efficacy of most diuretics.
- Lithium toxicity risk is increased with thiazides and loop diuretics.
- Spironolactone may cause gynecomastia and other anti-androgenic effects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

