DILI Basics - Liver's Drug Drama
- What is DILI? Liver injury caused by medications, herbal products, or toxins. Significant cause of Acute Liver Failure (ALF).
- Key Injury Patterns:
- Hepatocellular: Predominant Alanine Aminotransferase (ALT) elevation.
- Cholestatic: Predominant Alkaline Phosphatase (ALP) elevation.
- Mixed: Both ALT and ALP are elevated.
- R-Value (CIOMS Scale): Quantifies liver injury pattern.
- Formula: $R = (ALT / ULN_{ALT}) / (ALP / ULN_{ALP})$
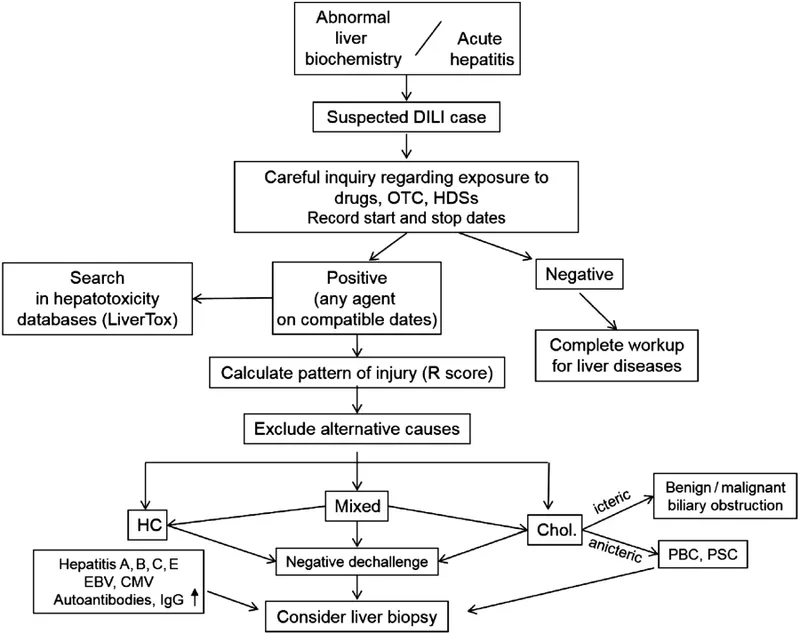
⭐ The R-value (CIOMS scale) is critical: Hepatocellular DILI is defined by $R \ge \textbf{5}$, Cholestatic DILI by $R \le \textbf{2}$, and Mixed DILI by $\textbf{2} < R < \textbf{5}$.
Mechanisms & Risks - Why Livers Suffer
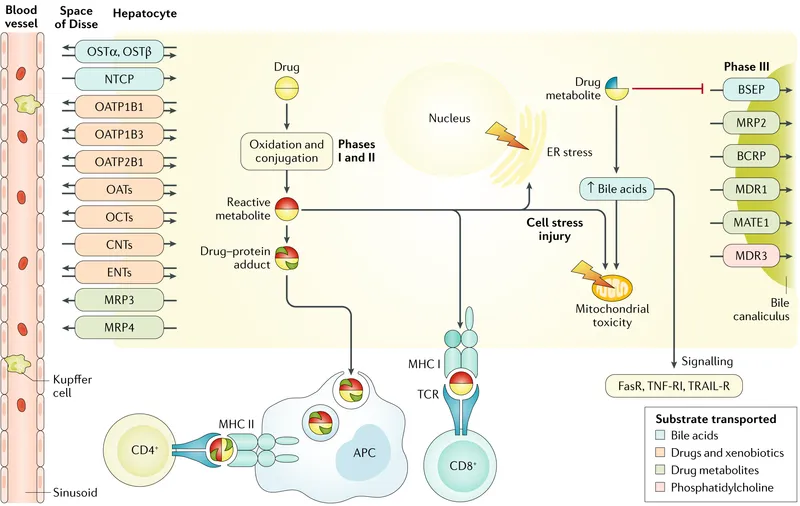
- Mechanisms of Injury:
- Direct (Intrinsic): Predictable, dose-dependent. E.g., Paracetamol (NAPQI formation).
- Pathways: Covalent binding, oxidative stress, mitochondrial dysfunction.
- Idiosyncratic (iDILI): Unpredictable, not strictly dose-related.
- Immune-allergic (e.g., halothane, phenytoin).
- Non-allergic/Metabolic (e.g., isoniazid, valproate causing mitochondrial injury).
- Bile salt export pump (BSEP) inhibition.
- Direct (Intrinsic): Predictable, dose-dependent. E.g., Paracetamol (NAPQI formation).
- Key Risk Factors:
- Drug: High daily dose (>50-100 mg/day), lipophilicity, extensive hepatic metabolism.
- Host: Age (elderly ↑risk), genetics (e.g., CYP variants, HLA-B*5701), alcohol use, female sex, obesity, pre-existing liver disease, malnutrition.

⭐ Most DILI cases are idiosyncratic, meaning they are unpredictable, not strictly dose-dependent, and occur in a minority of individuals exposed to the drug.
Top Drug Offenders - Pharma's Hit List
| Drug | Pattern of Injury | Key Points / Management |
|---|---|---|
| Paracetamol | Intrinsic, hepatocellular necrosis | Dose-dependent; Toxic dose >150 mg/kg; Antidote: NAC |
| Isoniazid (INH) | Idiosyncratic, hepatocellular | ↑ risk with age, alcohol, rifampicin; Monitor LFTs |
| Valproic Acid | Idiosyncratic, microvesicular steatosis | Reye-like syndrome; Carnitine may help |
| Amiodarone | Idiosyncratic, phospholipidosis | Mimics alcoholic hepatitis; Long half-life |
| Statins | Idiosyncratic, hepatocellular/cholestatic | Usually mild ALT ↑; Monitor LFTs if symptomatic |
| NSAIDs | Idiosyncratic, varied | Diclofenac, Sulindac common; Discontinue drug |
| Amoxicillin-Clavulanate | Idiosyncratic, cholestatic | Often delayed onset (1-6 weeks); Jaundice common |
Spotting & Solving - DILI Detective Work
⭐ Hy's Law identifies patients with hepatocellular DILI at high risk (10-50%) of fatal liver injury: Jaundice (Bilirubin >2-3x ULN) + ALT/AST elevation (>3x ULN) without significant ALP rise, in absence of other causes.
- Diagnosis:
- Thorough drug history (timing, dose, prior exposure).
- Exclude other liver diseases (viral, alcohol, autoimmune).
- Causality assessment (e.g., RUCAM score).
- Liver biopsy if diagnosis remains uncertain.
- Management Principles:
- Prompt withdrawal of suspected drug.
- Supportive care; specific antidotes (e.g., NAC for paracetamol).
- Monitor LFTs; consider transplant for ALF.
High‑Yield Points - ⚡ Biggest Takeaways
- Paracetamol is the most common DILI cause; N-acetylcysteine is the antidote.
- Intrinsic DILI is dose-dependent (e.g., paracetamol); Idiosyncratic DILI is unpredictable.
- Amoxicillin-clavulanate and anabolic steroids frequently cause cholestatic DILI.
- Isoniazid, halothane, and statins are common causes of hepatocellular DILI.
- Reye's syndrome: aspirin in children with viral illness, causing encephalopathy and fatty liver.
- Valproate can cause fatal hepatotoxicity, especially microvesicular steatosis in children.
- Methotrexate use can lead to chronic liver injury, fibrosis, and cirrhosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

