Overview & Mechanisms - Blood Cell Busters
Adverse drug reactions (ADRs) damaging blood cells (RBCs, WBCs, platelets) or bone marrow. Leads to anemia, leukopenia, agranulocytosis, thrombocytopenia, pancytopenia, or aplastic anemia. Mechanisms:
- Immune-mediated Destruction:
- Hapten-induced (e.g., Penicillin causing hemolytic anemia)
- Innocent bystander (e.g., Quinidine causing thrombocytopenia)
- True Autoimmune (e.g., Methyldopa causing hemolytic anemia)
- Direct Dose-Dependent Toxicity:
- Myelosuppression (e.g., Chemotherapeutic agents, Linezolid)
- Idiosyncratic Reactions: Unpredictable, often severe, not dose-related.
- Aplastic anemia (e.g., Chloramphenicol, NSAIDs)
- Agranulocytosis (e.g., Clozapine, Carbimazole, Propylthiouracil)
- Oxidative Hemolysis:
- In G6PD deficient individuals with oxidant drugs (e.g., Primaquine, Sulfonamides, Dapsone).
⭐ Chloramphenicol exhibits two forms of bone marrow toxicity: a common, dose-related, reversible erythroid suppression, and a rare, fatal, idiosyncratic aplastic anemia unrelated to dose or duration of therapy.
Aplastic Anemia & Agranulocytosis - Marrow Mayhem
-
Aplastic Anemia (Pancytopenia + Hypocellular Marrow)
- Key Drugs:
- Dose-dependent: Chemotherapy, chloramphenicol (early, reversible suppression).
- Idiosyncratic: Chloramphenicol (late, irreversible aplasia, fatal), NSAIDs (phenylbutazone), sulfonamides, gold, anticonvulsants (carbamazepine, phenytoin), PTU.
- Clinical: Anemia (fatigue), thrombocytopenia (bleeding), neutropenia (infections).
- Dx: BM biopsy (<25% cellularity, ↑fat).
- Rx: Stop drug, support (transfusions, antibiotics), IST (ATG, cyclosporine), BMT.
- Key Drugs:
-
Agranulocytosis (Severe Neutropenia: ANC < 500/µL)
- Key Drugs: Clozapine, antithyroids (PTU, methimazole), sulfonamides, carbamazepine, ticlopidine, metamizole.
- Clinical: Sudden fever, sore throat, mouth ulcers; sepsis risk.
- Dx: CBC (isolated neutropenia). BM: myeloid arrest/hypocellular.
- Rx: Stop drug, IV antibiotics, G-CSF.
⭐ Clozapine mandates regular ANC monitoring (e.g., weekly for 18 wks) for agranulocytosis risk.
Thrombocytopenia & Hemolytic Anemia - Platelet Plunge & RBC Rupture
Drug-Induced Thrombocytopenia (DITP):
- Mechanism: Immune (drug-dependent Abs).
- Onset: 5-14 days; rapid on re-exposure.
- Key Drugs: Heparin (HIT: ⚠️ paradoxical thrombosis risk!), Quinine, Sulfonamides, Vancomycin, GP IIb/IIIa inhibitors (Abciximab: rapid).
- Features: Bleeding, petechiae.
- Rx: Stop drug. Platelets if severe. HIT: non-heparin anticoagulants.
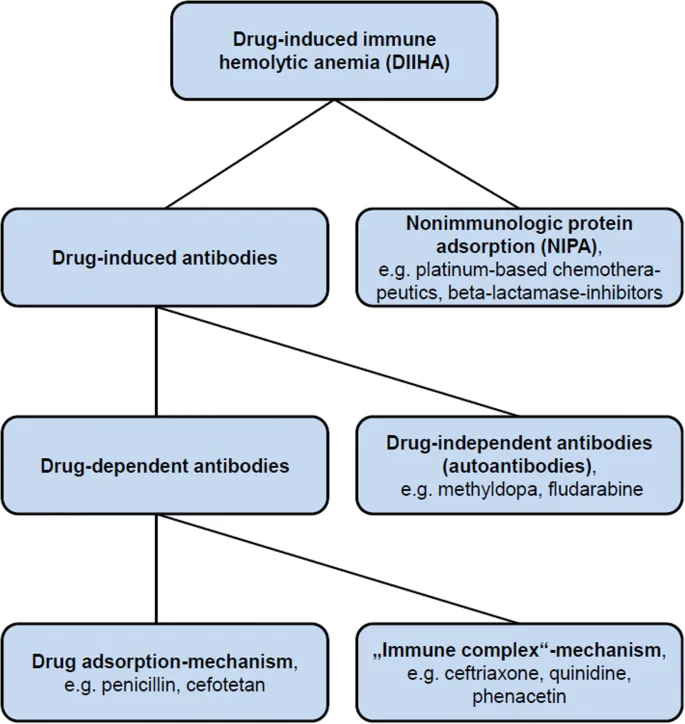
Drug-Induced Hemolytic Anemia (DIHA):
- Mechanisms:
- Immune: Hapten (Penicillin G), Immune Complex (Quinidine), Autoimmune (Methyldopa).
- Oxidative: Dapsone, Primaquine (G6PD def.).
- Features: Anemia, jaundice, ↑LDH, +ve DAT.
- Rx: Stop drug. Steroids for immune.
⭐ HIT: prothrombotic despite ↓platelets. Suspect if platelet drop >50% or thrombosis 5-14 days post-heparin.
Diagnosis, Management & Prevention - Spotting & Stopping Trouble
- Diagnosis: Key: drug exposure timeline. Bone marrow biopsy if severe/unclear.
- Management: STOP drug immediately! Supportive (transfusions, G-CSF). Immunosuppression for immune cases.
- Prevention: Genetic tests (e.g., G6PD, HLA-B*5701). Monitor high-risk drugs (clozapine, MTX). Patient education.
⭐ Clozapine mandates regular WBC monitoring due to high risk of agranulocytosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Aplastic anemia: Key offending drugs include chloramphenicol, gold salts, carbamazepine, and NSAIDs.
- Agranulocytosis: Strongly associated with clozapine, thiouracils (e.g., propylthiouracil), and sulfonamides.
- Megaloblastic anemia: Caused by methotrexate, phenytoin, trimethoprim due to folate antagonism or impaired absorption.
- Hemolytic anemia: Especially in G6PD deficiency, triggered by sulfonamides, dapsone, primaquine, nitrofurantoin.
- Thrombocytopenia: Heparin (HIT) is critical; also quinidine, sulfonamides, valproic acid.
- Drug-induced lupus (procainamide, hydralazine, isoniazid) can present with pancytopenia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

