NMBA Basics - Muscle Meltdown Intro
- Neuromuscular Blocking Agents (NMBAs): Potent drugs inducing skeletal muscle paralysis by acting at the Neuromuscular Junction (NMJ).
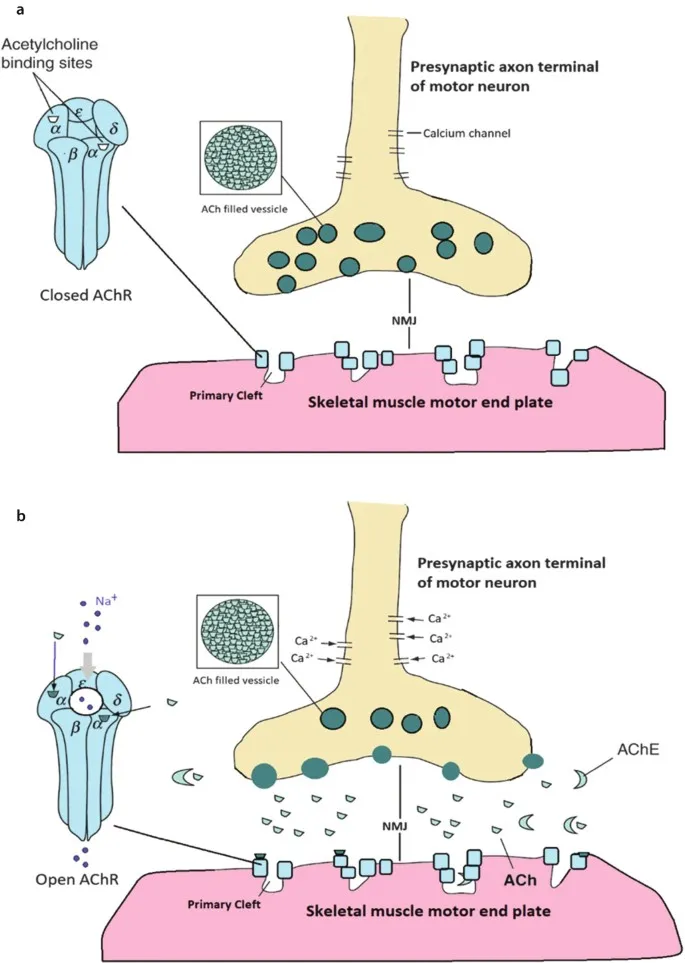
- Mechanism: Interfere with acetylcholine (ACh) binding to postsynaptic muscle-type nicotinic receptors ($N_M$ AChR).
- Primary Goal: Achieve profound muscle relaxation for medical procedures.
- Categories:
- Depolarizing (e.g., Succinylcholine)
- Non-depolarizing (e.g., "-curoniums", "-curiums") 📌 "-curare" derivatives.
- Key Uses: Surgical relaxation, endotracheal intubation, facilitating mechanical ventilation in ICU.
⭐ NMBAs provide NO analgesia or amnesia. Always ensure adequate sedation and analgesia in conscious patients.
Succinylcholine - The Fast & Furious Relaxer
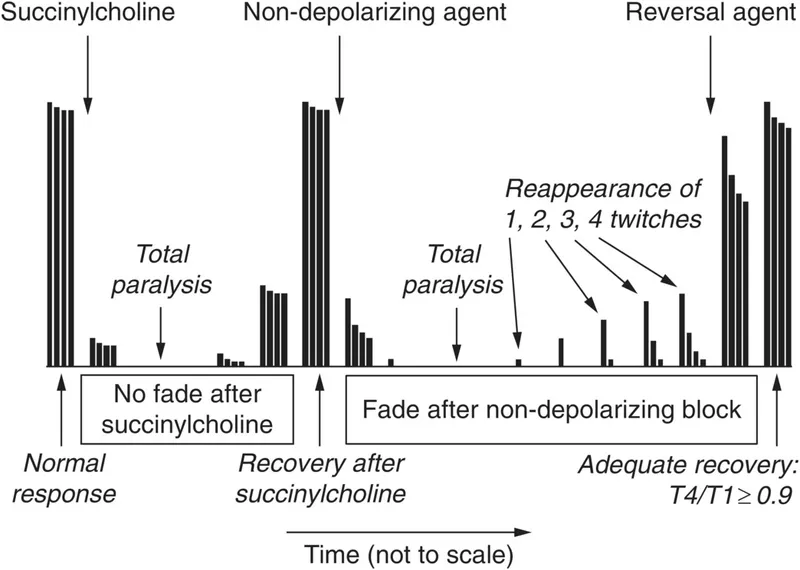
- Class: Depolarizing neuromuscular blocker (DNMB).
- Mechanism (Phase I): Binds nAChR → initial depolarization (fasciculations) → sustained flaccid paralysis. Not reversed by AChE inhibitors.
- Phase II (prolonged/high dose): Desensitizing block.
- Kinetics: Onset <1 min; Duration 5-10 min. Metabolized by plasma pseudocholinesterase. Deficiency → prolonged apnea.
- Uses: Rapid Sequence Intubation (RSI), ECT.
- Adverse Effects:
- ⚠️ Hyperkalemia: Risk ↑ in burns, crush injury, denervation (after 24-72h), neuromuscular disease.
- ⚠️ Malignant Hyperthermia (MH): Trigger.
- ↑IOP, ↑Intragastric pressure, Myalgia.
- Bradycardia (esp. children/repeat doses).
- Contraindications: MH history, hyperkalemia risk states, penetrating eye injury.
⭐ Succinylcholine is contraindicated after 24-72 hours in major burns or crush injuries due to fatal hyperkalemia risk from extrajunctional ACh receptor upregulation.
Non-Depolarizing Agents - The Steady Blockers
- Mechanism: Competitive antagonists at NMJ Nm receptors. Prevent ACh action; no depolarization.
- Classification & Key Features:
- Isoquinoline Derivatives:
- Atracurium: Hofmann elimination (non-enzymatic, temp/pH dependent) & ester hydrolysis. Laudanosine (metabolite, CNS stimulant/seizures). Histamine release.
- Cisatracurium: Isomer of atracurium. Hofmann elimination. Less laudanosine, minimal histamine. Organ-independent.
- Mivacurium: Shortest acting. Metabolized by plasma pseudocholinesterase. Histamine release. (Prolonged if atypical cholinesterase).
- Steroid Derivatives (suffix "-curonium"):
- Pancuronium: Long-acting. Mainly renal excretion. Vagolytic (↑HR).
- Vecuronium: Intermediate-acting. Mainly hepatic metabolism. Minimal CV effects.
- Rocuronium: Intermediate-acting, rapid onset. Hepatic metabolism. Reversible by Sugammadex.
- Isoquinoline Derivatives:
- Paralysis Sequence: Eyes/face/fingers → limbs → trunk → intercostals → diaphragm. Reverse recovery. 📌 (Order: Face/Fingers → Limbs → Trunk → Intercostals → Diaphragm)
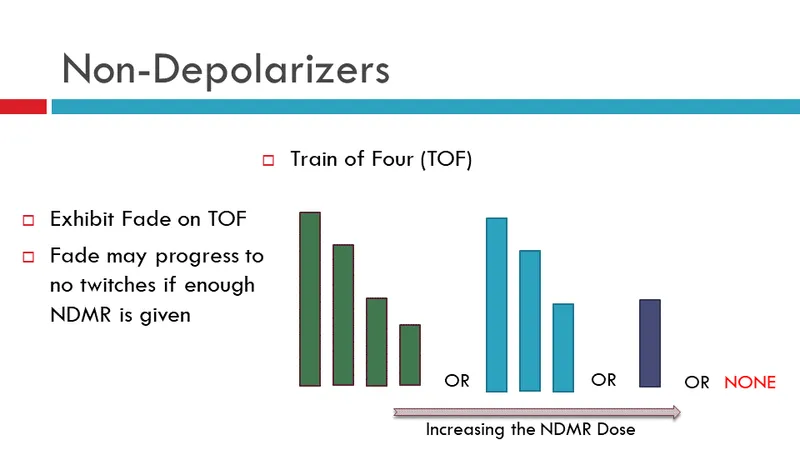
- Monitoring: Train-of-Four (TOF) stimulation.
- Reversal:
- AChE inhibitors (e.g., Neostigmine) + Antimuscarinic (e.g., Glycopyrrolate).
- Sugammadex (specific for Rocuronium, Vecuronium).
- Interactions: Potentiated by inhalational anesthetics, aminoglycosides, hypothermia, Mg²⁺, myasthenia gravis (↑sensitivity).
⭐ Cisatracurium is preferred in patients with renal or hepatic failure due to its organ-independent Hofmann elimination and lower histamine release.
Reversal & Clinical Pearls - Waking Up the Muscles
- Reversal:
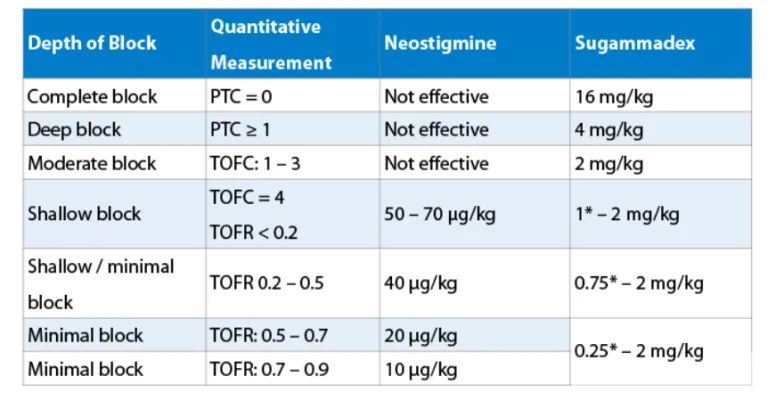
- Anticholinesterases (AChEIs): Neostigmine (0.04-0.07 mg/kg) + Antimuscarinic (Glycopyrrolate 0.01-0.02 mg/kg) to block muscarinic side effects.
- Sugammadex: For Rocuronium, Vecuronium. Dose 2-4 mg/kg (moderate block), 16 mg/kg (immediate rescue).
- Goal: Train-of-Four (TOF) ratio > 0.9 for extubation.
- Pearls:
- Potentiation of NMBs: Aminoglycosides, volatiles, hypothermia, ↓K⁺, ↑Mg²⁺, Myasthenia Gravis.
- Antagonism of NMBs: Chronic anticonvulsants (e.g., phenytoin).
- ⭐ > Sugammadex can decrease hormonal contraceptive efficacy; counsel patient.
High‑Yield Points - ⚡ Biggest Takeaways
- Succinylcholine: Rapid onset/offset, Phase I (depolarizing) & Phase II block; key risks: hyperkalemia, malignant hyperthermia.
- Non-depolarizing agents (e.g., rocuronium, vecuronium): Competitive antagonists at Nm receptors.
- Reversal: Neostigmine (AChE inhibitor) for non-depolarizers; Sugammadex for rocuronium/vecuronium.
- Atracurium/Cisatracurium: Unique Hoffman elimination, ideal in renal/hepatic failure.
- Mivacurium: Shortest acting non-depolarizer, metabolized by plasma pseudocholinesterase.
- Pancuronium: Long-acting agent, causes tachycardia (vagolytic effect).
- TOF monitoring: Shows fade with non-depolarizers and Phase II block of succinylcholine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

