Cholinergic Agonists: Overview & Receptors - Acetylcholine's Allies
- Acetylcholine (ACh): Primary neurotransmitter in PNS; also CNS.
- Synthesis: Choline + Acetyl CoA (by ChAT).
- Degradation: Rapidly by Acetylcholinesterase (AChE).
- Cholinoceptor Types:
- Muscarinic (M): GPCRs; 5 subtypes (M1-M5).
- M1 ("Neural"): CNS, enteric nerves; Gq. 📌 "M1 CNS Gq"
- M2 ("Cardiac"): Heart (↓HR, ↓force); Gi. 📌 "M2 Heart Gi"
- M3 (Glands/Smooth Muscle): Glands, SM, eye (miosis); Gq. 📌 "M3 Glands/Smooth Gq"
- Nicotinic (N): Ligand-gated ion channels; rapid Na+/K+ influx.
- Nn: Autonomic ganglia, adrenal medulla, CNS.
- Nm (Muscle): Skeletal neuromuscular junction (NMJ).
- Muscarinic (M): GPCRs; 5 subtypes (M1-M5).
⭐ Bethanechol (direct M-agonist) treats urinary retention (post-op, neurogenic) via M3 action on bladder detrusor.
Direct-Acting Cholinergic Agonists - Receptor Rockstars
- Directly activate Muscarinic (M) / Nicotinic (N) receptors.
- Bethanechol: 📌 "Bethanechol for Bowels & Bladder"
- M3 selective. Uses: Post-op ileus, urinary retention.
- Resistant to AChE.
- Pilocarpine:
- M3 agonist. Tertiary amine (CNS entry possible).
- Uses: Glaucoma (open-angle, acute angle-closure), Sjögren's (xerostomia).
⭐ Pilocarpine rapidly induces miosis, opening trabecular meshwork to ↓ Intraocular Pressure (IOP) in acute angle-closure glaucoma.
- Carbachol:
- M + N agonist.
- Uses: Glaucoma, surgical miosis. Resistant to AChE.
- Methacholine:
- M3 agonist. Use: Asthma diagnosis (bronchial challenge test).
- Cevimeline:
- M3 selective. Use: Sjögren's syndrome (dry mouth/eyes).
- Side Effects (DUMBBELSS): Diarrhea, Urination, Miosis, Bronchoconstriction, Bradycardia, Emesis, Lacrimation, Salivation, Sweating. Treat with Atropine (muscarinic antagonist).
Indirect-Acting Reversible Cholinergic Agonists - Signal Boosters
- Mechanism: Inhibit acetylcholinesterase (AChE) enzyme → ↑acetylcholine (ACh) concentration at cholinergic synapses.
- Key Drugs & Specifics:
- Physostigmine: Tertiary amine (crosses BBB). Uses: Atropine overdose, glaucoma.
- Neostigmine: Quaternary amine (no CNS). Uses: Myasthenia Gravis (MG), postoperative ileus/urinary retention, reversal of non-depolarizing muscle relaxants.
- Pyridostigmine: Quaternary amine. Longer duration. Use: MG (chronic management).
- Edrophonium (Tensilon): Quaternary amine. Short-acting (diagnostic). Use: MG diagnosis (Tensilon test).
- Alzheimer's Disease Drugs: Donepezil, Rivastigmine, Galantamine (CNS active, improve cognitive function).
- Adverse Effects: Cholinergic crisis (DUMBELS: Diarrhea, Urination, Miosis, Bronchospasm/Bradycardia, Emesis, Lacrimation, Salivation/Sweating). Antidote: Atropine.
- 📌 Mnemonic (Neostigmine uses): No Mystery Please - Neostigmine for Myasthenia, Post-op ileus/urinary retention.
⭐ Physostigmine is the drug of choice for treating poisoning with atropine or other antimuscarinic drugs due to its ability to cross the blood-brain barrier and antagonize central anticholinergic effects.
Indirect-Acting Irreversible Cholinergic Agonists & Toxicity - Deadly Duty
-
Examples: Organophosphates (Malathion, Parathion, Diazinon), Nerve gases (Sarin, Soman). Echothiophate (rarely for glaucoma).
-
Mechanism: Irreversibly phosphorylate acetylcholinesterase (AChE) → ↑Acetylcholine (ACh) at all sites.
- "Aging": Enzyme-inhibitor complex strengthens over time, rendering oximes (e.g., Pralidoxime) ineffective.
-
Toxicity (Cholinergic Crisis):
- Muscarinic: 📌 DUMBBELSS: Diarrhea, Urination, Miosis (pinpoint pupils), Bronchospasm/Bronchorrhea, Bradycardia, Emesis, Lacrimation, Salivation/Sweating.
- Nicotinic: Muscle fasciculations, weakness, paralysis (can lead to respiratory failure).
- CNS: Agitation, confusion, seizures, coma.
-
Management:
- Atropine: Muscarinic antagonist. Titrate to dry secretions, HR > 80/min. Does not reverse paralysis.
- Pralidoxime (PAM): AChE reactivator. Crucial before "aging" of enzyme complex. Primarily for nicotinic effects.
- Diazepam: For seizures. Supportive ventilation often vital.
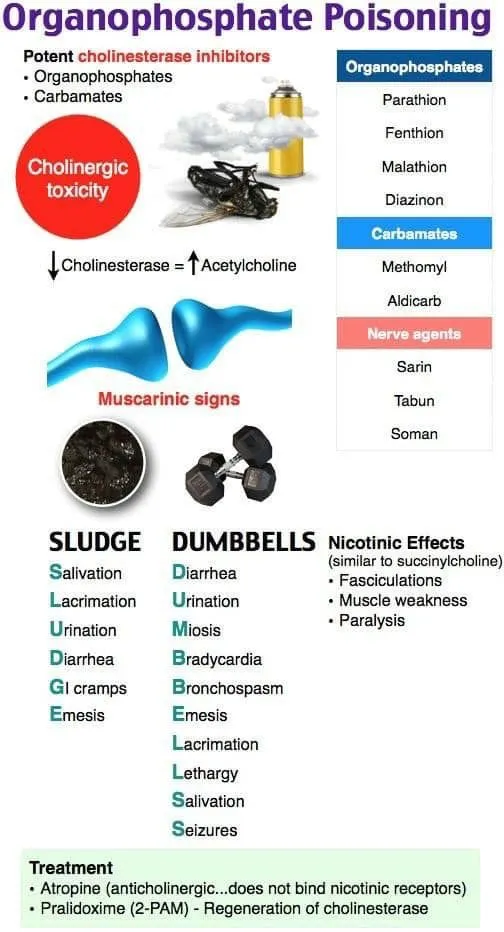
- ⭐ > Atropine reverses muscarinic and CNS effects of organophosphate poisoning but NOT nicotinic effects like muscle paralysis. Respiratory support is critical.
High‑Yield Points - ⚡ Biggest Takeaways
- Direct agonists (e.g., Pilocarpine, Bethanechol) stimulate muscarinic/nicotinic receptors.
- Indirect agonists (AChE inhibitors) like Neostigmine ↑ACh by blocking its breakdown.
- Pilocarpine: treats glaucoma (↑outflow) and xerostomia (Sjögren's).
- Bethanechol: for postoperative ileus and urinary retention (atonic bladder).
- Myasthenia gravis: treat with Neostigmine/Pyridostigmine; diagnose with Edrophonium.
- Organophosphate poisoning (irreversible AChE block): SLUDGEM; treat with Atropine + Pralidoxime.
- Physostigmine (crosses BBB): antidote for central anticholinergic toxicity (atropine overdose).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

