Adrenergic Receptors & Classification - Receptor Rhapsody
Error: Failed to generate content for this concept group.
Catecholamines - Adrenaline's A-Team
-
IV admin (Epi IM/SC too). Rapid COMT/MAO metabolism. ADRs: Arrhythmias, HTN. ⚠️ Extravasation necrosis.
-
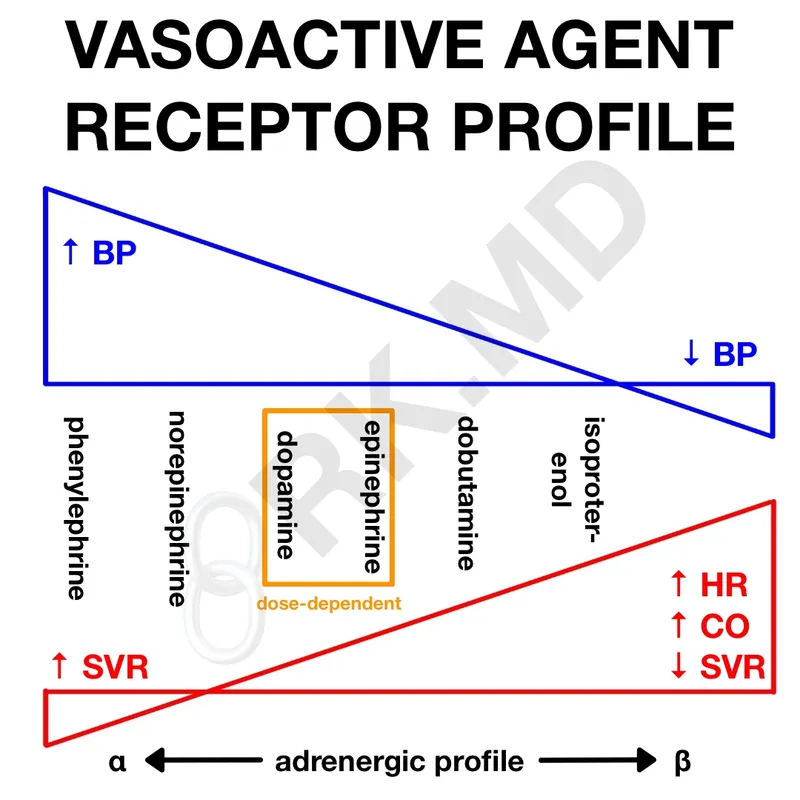
Epinephrine (Adrenaline): α1,α2,β1,β2 agonist.
- Uses: Anaphylaxis (0.3-0.5mg IM/SC 1:1000; IV 1:10000 shock), cardiac arrest, septic shock.
⭐ Epinephrine Reversal of Dale: With α-blocker, Epi causes ↓BP (unopposed β2 vasodilation).
-
Norepinephrine (Noradrenaline): α1>β1 agonist (little β2).
- Uses: Septic/cardiogenic shock (↑SVR, ↑MAP).
-
Isoproterenol (Isoprenaline): β1,β2 agonist (non-selective).
- Uses: Bradycardia/heart block (↑HR, ↓SVR).
-
Dopamine: Dose-dependent:
- Low: D1 (renal VD)
- Med: β1 (↑inotropy, ↑HR)
- High: α1 (VC)
- 📌 D1→β1→α1 (↑dose).
- Uses: Shock, bradycardia.
-
Dobutamine: Mainly β1 agonist (mild β2/α1).
- Uses: Acute HF/cardiogenic shock (↑inotropy).
Alpha-Selective Agonists - Alpha Force
- Alpha-1 ($\alpha_1$) Selective Agonists:
- Drugs: Phenylephrine, Midodrine.
- Uses:
- Phenylephrine: Mydriasis (non-cycloplegic), nasal decongestant, ↑BP (pressor).
- Midodrine: Orthostatic hypotension.
- Alpha-2 ($\alpha_2$) Selective Agonists:
- Drugs: Clonidine, Methyldopa (prodrug), Apraclonidine, Brimonidine.
- Uses:
- Clonidine: Hypertension, ADHD, opioid/nicotine withdrawal.
- Methyldopa: Hypertension in pregnancy.
- Apraclonidine, Brimonidine: Glaucoma (↓aqueous humor production).
- Key Adverse Effects (AEs):
- Clonidine: Sedation, dry mouth, ⚠️ rebound hypertension (abrupt withdrawal).
- Methyldopa: Sedation, drug-induced lupus, Coombs-positive hemolytic anemia.
⭐ Methyldopa is a notable cause of drug-induced Coombs-positive hemolytic anemia.
Beta-Selective & Other Agonists - Beta Boosters & Mixers
- β1-Selective Agonist
- Dobutamine: Primarily β1 (↑inotropy, chronotropy); cross-ref Catecholamines.
- β2-Selective Agonists
- SABA (Short-Acting): Salbutamol (Albuterol), Terbutaline.
- Uses: Acute asthma, COPD, hyperkalemia (Salbutamol), tocolysis (Terbutaline).
- LABA (Long-Acting): Salmeterol, Formoterol.
- Uses: Chronic asthma/COPD (with corticosteroids).
- Ritodrine: Tocolytic (largely replaced).
- AEs (common to β2 agonists): Tremor, tachycardia, palpitations, hypokalemia.
- SABA (Short-Acting): Salbutamol (Albuterol), Terbutaline.
- Indirect-Acting Sympathomimetics
- Amphetamine, Tyramine: MOA - Release stored NE.
- Cocaine: MOA - Inhibits NE reuptake.
- Mixed-Acting Sympathomimetics
- Ephedrine, Pseudoephedrine: MOA - Direct receptor agonism + release stored NE.
- Uses: Nasal decongestion, pressor (Ephedrine). Tachyphylaxis.
- Ephedrine, Pseudoephedrine: MOA - Direct receptor agonism + release stored NE.
⭐ Long-Acting Beta-Agonists (LABAs) like Salmeterol and Formoterol should not be used as monotherapy for asthma due to increased risk of asthma-related death; they must be used with an inhaled corticosteroid.
High-Yield Points - ⚡ Biggest Takeaways
- Dobutamine (β1 agonist): For cardiogenic shock, acute HF; primarily ↑cardiac contractility.
- Phenylephrine (α1 agonist): Causes vasoconstriction, mydriasis; used as nasal decongestant, raises BP.
- Clonidine (central α2 agonist): For hypertension, opioid withdrawal. (α-methyldopa: HTN in pregnancy).
- Salbutamol/Terbutaline (β2 agonists): For acute asthma/COPD; main side effects: tremor, tachycardia.
- Dopamine: Dose-dependent effects: low (D1 renal), medium (β1 cardiac), high (α1 vasoconstriction).
- Epinephrine (α & β agonist): Drug of choice for anaphylactic shock, cardiac arrest.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

