Macrolides: Intro & MOA - Ribosome Raiders
- Bacteriostatic agents; can be bactericidal at high concentrations.
- Structure: Large macrocyclic lactone ring with attached deoxy sugars.
- Mechanism of Action (MOA):
- Bind reversibly to the 50S ribosomal subunit.
- Specifically to the 23S rRNA component, near the peptidyltransferase center.
- Inhibit bacterial protein synthesis by blocking the translocation step.
- Prevents movement of peptidyl-tRNA from the A-site (acceptor) to the P-site (peptidyl).
- 📌 Mnemonic (Ribosomal targets): "Buy AT 30, CCELL at 50" (E for Erythromycin/Macrolides).
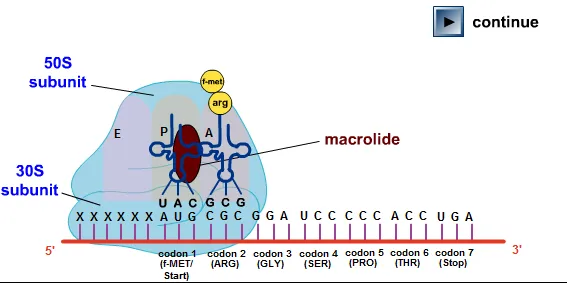
- Bind reversibly to the 50S ribosomal subunit.
⭐ Macrolides primarily inhibit protein synthesis by binding to the 23S rRNA of the 50S ribosomal subunit, thereby blocking polypeptide chain elongation and translocation.
Macrolides: PK & Spectrum - Germ Targets
Pharmacokinetics (PK) Comparison:
| Feature | Erythromycin | Clarithromycin | Azithromycin |
|---|---|---|---|
| Absorption | Variable, food ↓, acid-labile | Good, acid-stable | Good, food ↓(cap), acid-stable |
| Distribution | Wide (excl. CNS) | Wide, ↑tissue (lung) | Extensive tissue, ↑Vd 📌AziTHROugh tissues |
| Metabolism | Hepatic (CYP3A4 inhib.) | Hepatic (CYP3A4 inhib.), active met. | Minimal hepatic, no CYP inhib. |
| Excretion | Biliary | Renal & Biliary | Biliary |
| t½ | ~1.5h | 3-7h | 40-68h (long) |
- Gram (+): Strep (pneumo, pyogenes), MSSA.
- Atypicals: Mycoplasma, Chlamydia, Legionella.
- Gram (-): H. influenzae, M. catarrhalis, N. gonorrhoeae, Campylobacter, H. pylori (Clarithro).
- Others: B. pertussis, MAC (Azithro/Clarithro).
⭐ Azithromycin's unique PK (long t½, high tissue conc.) allows short-course therapy (e.g., 3-5 days) for many infections.
Macrolides: Clinical Uses - Healing Hits
- Atypical pneumonias: Mycoplasma, Legionella, Chlamydia pneumoniae.
- Community-Acquired Pneumonia (CAP): Often first-line or in combination.
- Upper Respiratory Tract Infections (URTIs): Pharyngitis, sinusitis (if penicillin allergy).
- Skin and Soft Tissue Infections (SSTIs): Mild to moderate, especially if penicillin-allergic.
- Sexually Transmitted Infections (STIs): Chlamydia trachomatis (azithromycin single dose), chancroid.
- Pertussis (Whooping Cough): Drug of choice for treatment and prophylaxis.
- H. pylori eradication regimens (clarithromycin).
- Diphtheria: Carrier state and active infection (alternative to penicillin).
- Prophylaxis: Rheumatic fever (if penicillin allergy), MAC in HIV (azithromycin).
⭐ Azithromycin is highly effective as a single 1g oral dose for uncomplicated Chlamydia trachomatis genital infections.
📌 Mnemonic: "MACRO" for Mycoplasma, Atypical pneumonia, Chlamydia, Respiratory infections, Other (Pertussis, Diphtheria).
Macrolides: ADRs & Interactions - Drug Duels
- ADRs:
- GI Upset (most common, esp. Erythromycin)
- QT Prolongation & Torsades de Pointes (⚠️ Erythromycin > Clarithromycin > Azithromycin)
- Cholestatic Hepatitis (Erythromycin estolate)
- Ototoxicity (high doses, reversible)
- 📌 MACRO (Erythromycin): Motility, Arrhythmia, Cholestatic hepatitis, Rash, eOsinophilia.
- Ketolides (Telithromycin): Severe hepatotoxicity, Myasthenia Gravis exacerbation (⚠️ Contraindicated).
- Drug Interactions (CYP3A4 Inhibition - Erythromycin, Clarithromycin):
- ↑ Warfarin, Statins (Simvastatin, Atorvastatin), Theophylline, Carbamazepine, Cyclosporine.
- Avoid with other QT-prolonging drugs.
- Azithromycin: Minimal CYP interaction.
⭐ Clarithromycin & Erythromycin are potent CYP3A4 inhibitors; Azithromycin is the safest regarding drug interactions.
Macrolides: Resistance & Ketolides - Bugs Fight Back
- Macrolide Resistance:
- Methylation of 23S rRNA (erm genes): Main, high-level.
- Efflux pumps (mef genes).
- Esterase inactivation.
- Ketolides (e.g., Telithromycin):
- Engineered to combat resistance.
- Stronger, dual 23S rRNA binding; evade efflux.
- Effective against macrolide-resistant S. pneumoniae.
⭐ Ketolides overcome erm-mediated resistance (if inducible) due to dual rRNA binding and stability against efflux pumps.
High‑Yield Points - ⚡ Biggest Takeaways
- Mechanism: Bind 50S ribosome, blocking protein synthesis (translocation).
- Spectrum: Atypical pathogens (Mycoplasma, Chlamydia, Legionella), some Gram-positives, H. pylori.
- Pharmacokinetics: CYP450 inhibition (Erythromycin, Clarithromycin); Azithromycin has long half-life, fewer interactions.
- Adverse Effects: GI upset (motilin agonism), QT prolongation, cholestatic hepatitis, ototoxicity.
- Resistance: Methylation of 23S rRNA (erm genes), efflux pumps.
- Ketolides (Telithromycin): Overcome some macrolide resistance; higher affinity for 50S ribosome.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

