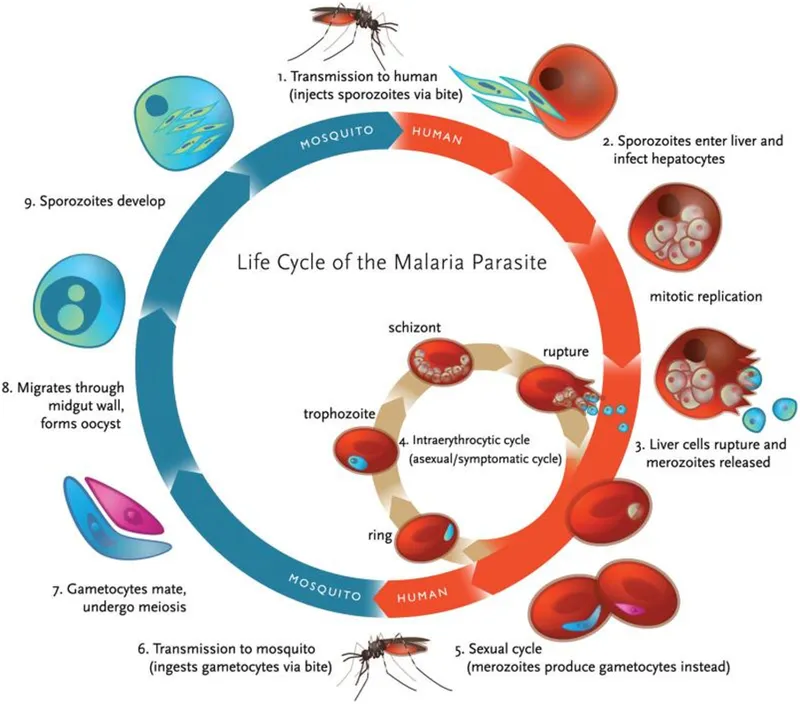
Antimalarials - Malaria Mayhem Meds
- Goal: Eradicate parasites from blood (clinical cure) & liver (radical cure).
- **Classification (Simplified):
- Blood Schizonticides: Act on erythrocytic forms. E.g., Chloroquine, Artemisinins, Quinine, Mefloquine.
- Tissue Schizonticides: Act on liver stages (hypnozoites). E.g., Primaquine.
- Gametocytocidals: Kill sexual forms. E.g., Primaquine.
- Key Drugs & Actions:
- Chloroquine: Inhibits heme polymerase. For sensitive P. vivax/ovale/malariae. Resistance in P. falciparum (PfCRT gene).
- Artemisinins (Artesunate, Artemether): Endoperoxide; free radical damage. Rapid action. DOC for severe malaria (IV Artesunate) & uncomplicated P. falciparum (as ACTs).
- Primaquine: Radical cure for P. vivax/ovale. ⚠️ Test for G6PD deficiency (risk of hemolysis).
- Mefloquine: Prophylaxis & treatment. Neuropsychiatric side effects.
- Atovaquone-Proguanil (Malarone®): Prophylaxis & treatment.
- 📌 All Clinicians Treat with ACTs for uncomplicated Falciparum.
⭐ Artemisinin-based Combination Therapy (ACT) is the WHO-recommended first-line treatment for uncomplicated P. falciparum malaria to combat resistance and improve efficacy.
Other Antiprotozoals - Protozoa Purge Pills
- Metronidazole & Tinidazole:
- MOA: Free radical damage in anaerobes.
- Uses: Amoebiasis, Giardiasis, Trichomoniasis, anaerobic infections. 📌 GET Anaerobes on the Metro (Giardia, Entamoeba, Trichomonas).
- AE: Disulfiram-like effect with alcohol, metallic taste, neurotoxicity (rare).
- Luminal Amoebicides: (For asymptomatic E. histolytica cyst passers)
- Diloxanide furoate (DOC), Iodoquinol (AE: optic neuritis), Paromomycin.
- Nitazoxanide:
- Broad spectrum: Giardia, Cryptosporidium. MOA: Inhibits PFOR enzyme.
- Leishmaniasis:
- Sodium Stibogluconate: AE: Cardiotoxicity (QT prolongation), pancreatitis.
- Amphotericin B (liposomal): DOC for Visceral Leishmaniasis (Kala-azar).
- Miltefosine: Oral, teratogenic.
- African Trypanosomiasis (Sleeping Sickness):
- Hemolymphatic stage: Suramin, Pentamidine.
- CNS stage: Melarsoprol (arsenical; AE: encephalopathy), Eflornithine.
- American Trypanosomiasis (Chagas Disease):
- Nifurtimox, Benznidazole.
- Pentamidine:
- Uses: Pneumocystis jirovecii pneumonia (PJP), Leishmaniasis, African Trypanosomiasis (early West African).
- AE: Pancreatitis, dysglycemia, nephrotoxicity.
⭐ Metronidazole is ineffective against luminal amoebic cysts; requires a luminal agent like Diloxanide furoate for eradication of infection and to prevent carrier state development or relapse after tissue amoebicide therapy for invasive disease.
Anthelmintics - Worm Wipeout Weapons
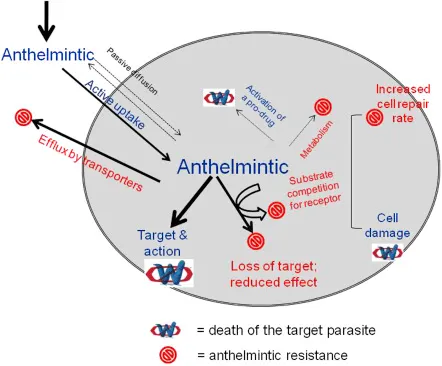
- Benzimidazoles (BZDs): Albendazole, Mebendazole
- Mech: Inhibit parasite β-tubulin → disrupt microtubule polymerization.
- Uses: Broad-spectrum - Ascaris, hookworm, whipworm (Trichuris), pinworm (Enterobius).
- Albendazole: Hydatid disease, neurocysticercosis. Fatty meal ↑ absorption.
- Praziquantel (PZQ):
- Mech: ↑ Ca²⁺ influx → tetanic muscle contraction & paralysis.
- Uses: Trematodes (Schistosomiasis, Clonorchiasis), Cestodes (Taeniasis, Diphyllobothriasis).
⭐ Praziquantel is the drug of choice for infections caused by all Schistosoma species.
- Ivermectin:
- Mech: Activates glutamate-gated Cl⁻ channels → flaccid paralysis.
- Uses: Onchocerciasis (DOC), Strongyloidiasis, Filariasis (microfilaricidal for W. bancrofti, B. malayi).
- Pyrantel Pamoate:
- Mech: Depolarizing neuromuscular blocker (nicotinic agonist) → spastic paralysis.
- Uses: Pinworm, Ascaris, Hookworm (alternative).
- Diethylcarbamazine (DEC):
- Mech: Alters parasite surface membrane → enhances host immune destruction; inhibits arachidonic acid metabolism.
- Uses: Lymphatic filariasis (W. bancrofti, B. malayi - DOC for adult worms & microfilariae), Loiasis (DOC), Tropical Pulmonary Eosinophilia.
- ⚠️ Mazzotti reaction (from dying microfilariae).
High‑Yield Points - ⚡ Biggest Takeaways
- Metronidazole: DOC for amebiasis, giardiasis, trichomoniasis; disulfiram-like reaction with alcohol.
- Albendazole/Mebendazole: Inhibit microtubule synthesis; Albendazole for neurocysticercosis, hydatid disease.
- Praziquantel: DOC for schistosomiasis & most cestodes; increases Ca²⁺ permeability.
- Chloroquine: For malaria prophylaxis & sensitive strains; risk of retinopathy (chronic use).
- ACTs (Artemisinin Combination Therapies): First-line for uncomplicated P. falciparum malaria.
- Ivermectin: DOC for onchocerciasis, strongyloidiasis; acts on glutamate-gated Cl⁻ channels.
- DEC (Diethylcarbamazine): DOC for lymphatic filariasis, loiasis; can cause Mazzotti reaction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

