First-Line Anti-TB Drugs - TB Titans
📌 Mnemonic: RIPE (Rifampicin, Isoniazid, Pyrazinamide, Ethambutol).
-
Isoniazid (H)
- MOA: Inhibits mycolic acid synthesis (KatG activation).
- ADRs: Peripheral neuropathy (give Pyridoxine B6 10-25mg), hepatotoxicity, drug-induced lupus.
- Bactericidal. Monitor LFTs.
-
Rifampicin (R)
- MOA: Inhibits DNA-dependent RNA polymerase.
- ADRs: Orange-red body fluids, hepatotoxicity, flu-like syndrome, potent CYP450 inducer.
- Bactericidal.
-
Pyrazinamide (Z)
- MOA: Disrupts cell membrane (pncA activation); active in acidic pH (macrophages).
- ADRs: Hepatotoxicity (most hepatotoxic, dose-dependent), hyperuricemia (gout), arthralgia.
- Bactericidal. Monitor LFTs, uric acid.
-
Ethambutol (E)
- MOA: Inhibits arabinosyl transferase (cell wall).
- ADRs: Optic neuritis (↓visual acuity, red-green color blindness), hyperuricemia.
- Bacteriostatic. Monitor vision. Renal dose adjustment.
⭐ Ethambutol causes dose-dependent optic neuritis (retrobulbar); monitor visual acuity and color vision regularly.
Second-Line Anti-TB Drugs - Backup Brigade
For MDR/XDR-TB or first-line intolerance. Less effective, more toxic.
- Injectables (Aminoglycosides/Polypeptides):
- Amikacin (Amk), Kanamycin (Km), Capreomycin (Cm)
- ADRs: Ototoxic, Nephrotoxic ⚠️ Monitor.
- Fluoroquinolones (FQs):
- Levofloxacin (Lfx), Moxifloxacin (Mfx)
- ADRs: Tendinopathy, CNS effects, QT prolongation (Mfx).
- Oral Bacteriostatic Agents:
- Cycloserine (Cs):
- ADRs: CNS toxicity (psychosis, seizures 📌 Psycho-serine), neuropathy. Give Pyridoxine.
- Ethionamide (Eto):
- ADRs: GI upset, hepatotoxic, hypothyroidism.
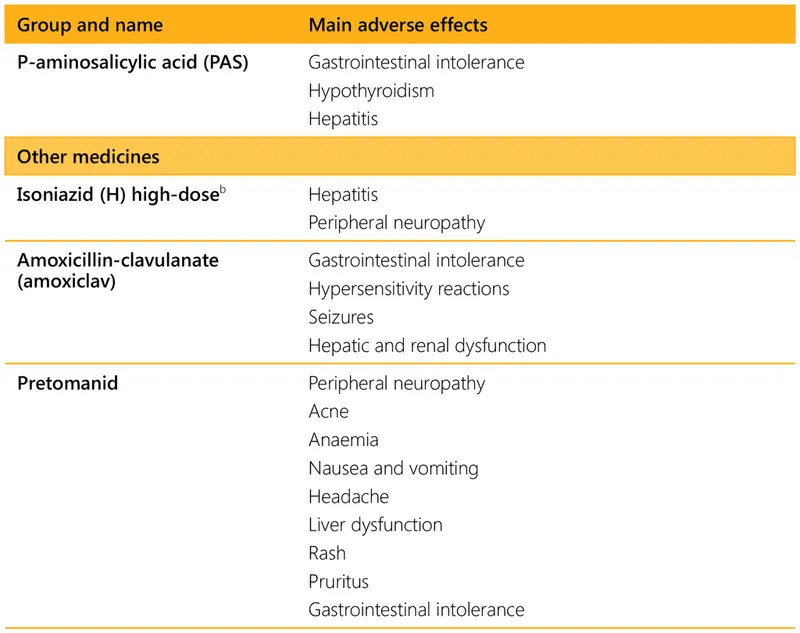
- PAS (Para-aminosalicylic acid):
- ADRs: GI upset, hypersensitivity, goitrogenic.
- Cycloserine (Cs):
- Newer/Repurposed Drugs:
- Bedaquiline (Bdq):
- ADRs: QT prolongation (⚠️ BBW), hepatotoxic.
- Delamanid (Dlm):
- ADRs: QT prolongation.
- Linezolid (Lzd):
- ADRs: Myelosuppression, neuropathy (long use > 28 days).
- Bedaquiline (Bdq):
⭐ Bedaquiline & Delamanid are vital for MDR-TB, but watch for QT prolongation.
Anti-Leprosy Drugs - Hansen's Helpers
- Key Drugs (📌 RDC: Rifampicin, Dapsone, Clofazimine):
- Dapsone: Folate antagonist. SE: Hemolysis (G6PD def.), agranulocytosis.
- Rifampicin: RNA pol inhibitor. SE: Hepatotoxicity, orange-red urine.
- Clofazimine: Phenazine dye; DNA binding. SE: Skin pigmentation (red-brown), GI upset.
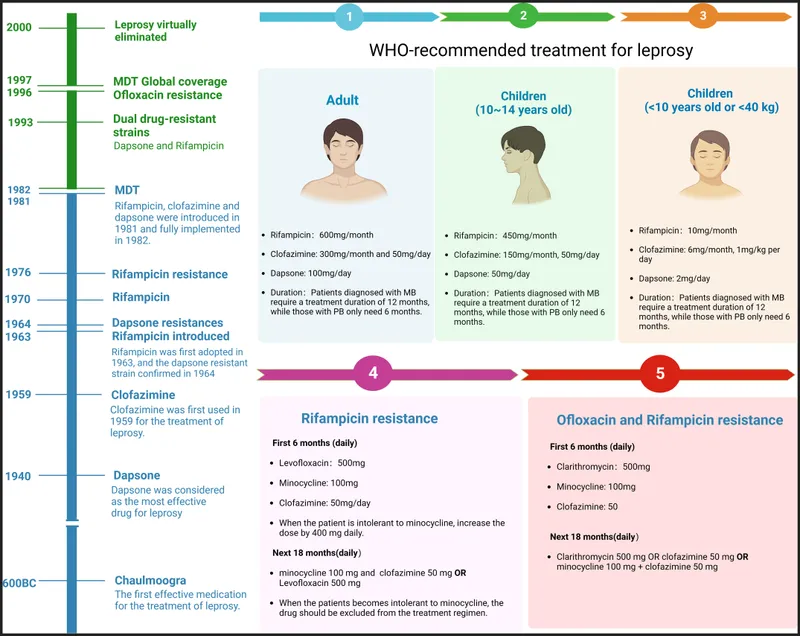
- Multidrug Therapy (MDT) - WHO Regimens:
- Paucibacillary (PB): 2 drugs (Rifampicin + Dapsone) for 6 months.
- Multibacillary (MB): 3 drugs (Rifampicin + Dapsone + Clofazimine) for 12 months.
- Lepra Reactions & Management:
- Type 1 (Reversal Reaction): Corticosteroids.
- Type 2 (Erythema Nodosum Leprosum - ENL): Thalidomide (⚠️ teratogenic), Corticosteroids, Clofazimine.
⭐ Dapsone hypersensitivity syndrome (DHS): severe reaction (2-8 weeks post-start), fever, rash, systemic involvement.
TB Drug Regimens & Special Populations - TB Treatment Tactics
- Standard Regimen (New, Drug-Sensitive):
- Intensive Phase (IP): 2 months HRZE.
- Continuation Phase (CP): 4 months HRE (or HR).
- Special Populations - Key Adjustments:
- Pregnancy: Avoid Streptomycin (fetal ototoxicity). HRZE safe. Add Pyridoxine (B6).
- HIV Co-infection: Rifabutin preferred with PIs/NNRTIs to ↓interactions.
- Renal Impairment: Modify Ethambutol, Pyrazinamide, Streptomycin doses.
- Drug-Resistant TB (DR-TB): Requires specialized, longer regimens (e.g., Bedaquiline, Linezolid, Pretomanid).
⭐ In pregnancy, Streptomycin is contraindicated (fetal ototoxicity). Standard HRZE is safe; always supplement Isoniazid with Pyridoxine (B6) to prevent neuropathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Rifampicin: RNA polymerase inhibitor; orange-red body fluids; potent CYP450 inducer.
- Isoniazid (INH): Mycolic acid synthesis inhibitor; peripheral neuropathy (prevent with B6), hepatotoxicity.
- Pyrazinamide (PZA): Active in acidic pH (macrophages); hyperuricemia, hepatotoxicity.
- Ethambutol: Optic neuritis (red-green color blindness); check visual acuity.
- Streptomycin: Aminoglycoside; ototoxicity, nephrotoxicity; contraindicated in pregnancy.
- MDR-TB: Resistance to at least Isoniazid and Rifampicin.
- Leprosy drugs: Dapsone (G6PD hemolysis), Clofazimine (pigmentation), Rifampicin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

