Classification - Fungal Foes & Drug Classes
Antifungal agents are classified by their mechanism of action, targeting unique fungal structures: cell membrane (ergosterol, squalene), cell wall (β-glucan), nucleic acids, or mitotic spindle (microtubules).
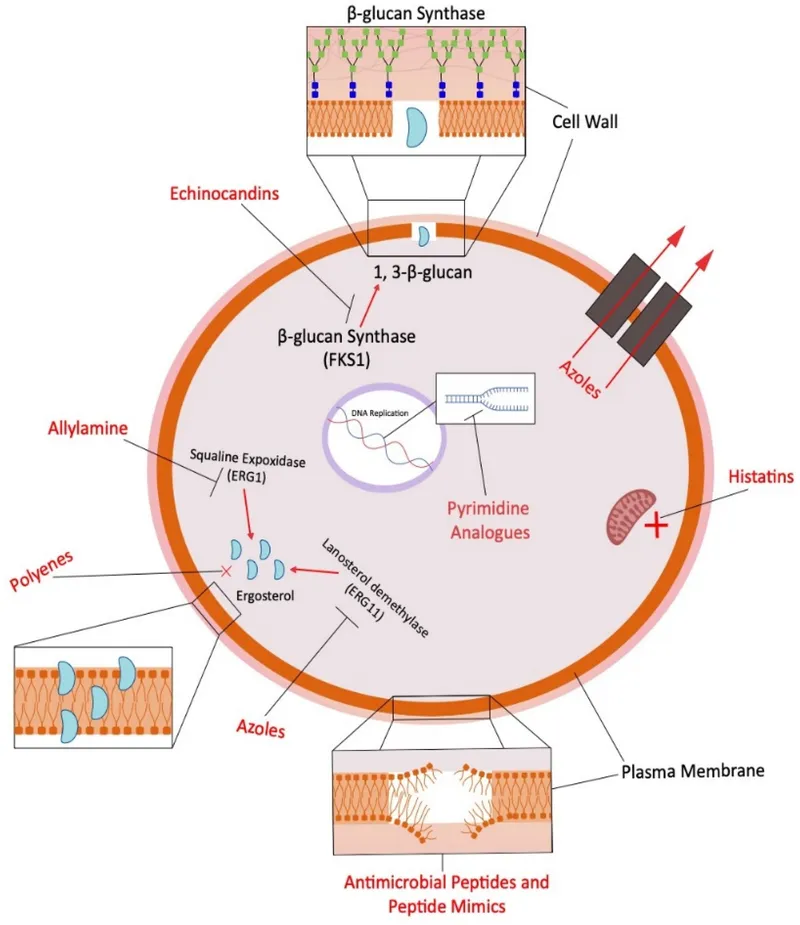
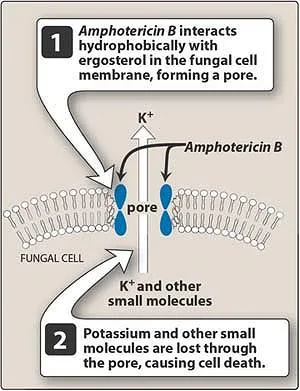
⭐ Amphotericin B: Binds ergosterol in fungal membranes, forming pores causing leakage & cell death. Broad spectrum; monitor for nephrotoxicity.
Polyenes - Ampho the Terrible & Co.
- Mechanism: Binds ergosterol (fungal membrane) → forms pores → K⁺/Mg²⁺ leakage → cell death.
- Spectrum: Broad: Candida, Aspergillus, Cryptococcus, endemic mycoses (e.g., Histoplasma).
- PK: IV only; poor CNS penetration.
- Toxicities: 📌 Ampho-terrible!
- Nephrotoxicity (dose-limiting; RTA). Monitor renal function.
- Infusion reactions (fever, chills, rigors - "shake and bake").
- Anemia (↓ erythropoietin).
- Electrolyte loss: ↓K⁺, ↓Mg²⁺.
- Liposomal Preps (LAmB): ↓ Nephrotoxicity & infusion reactions. Preferred if renal issues.
⭐ Conventional Amphotericin B deoxycholate requires a test dose due to potential anaphylactoid reactions.
Azoles - The "-azole" Armada
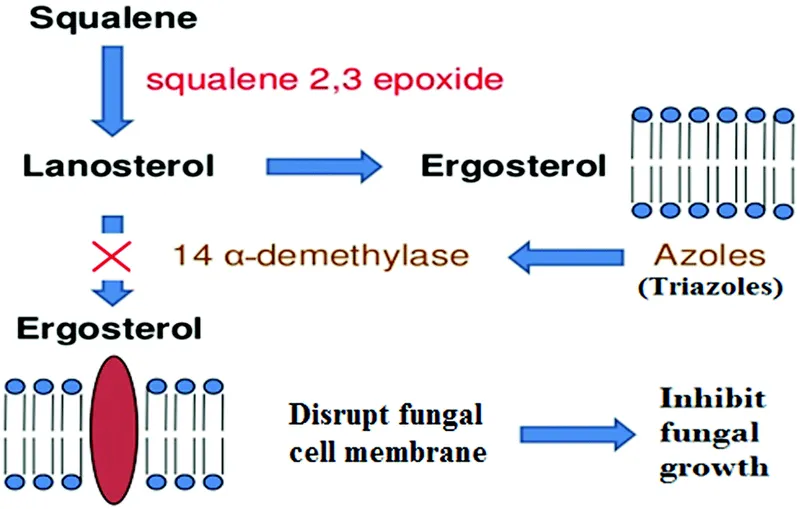
- Mechanism: Inhibit fungal 14-alpha-demethylase → ↓ergosterol synthesis.
- Types: Imidazoles (e.g., Ketoconazole); Triazoles (e.g., Fluconazole, Voriconazole, Itraconazole, Posaconazole).
- Interactions: Many are potent CYP450 inhibitors.
- Toxicities: Hepatotoxicity (class effect); QT prolongation (some, e.g., Voriconazole).
- Key Triazoles Comparison:
Azole Key Spectrum Key Notes Fluconazole Candida, Cryptococcus Good CSF; Few DDIs; Renal excretion Itraconazole Aspergillus, Histoplasma, Blastomyces Potent CYP3A4 inh; CHF risk; Needs acid Voriconazole Aspergillus (DOC), C. krusei/glabrata Visual issues; Photosensitivity; Good CSF Posaconazole Broadest: Zygomycetes, Aspergillus, Candida Prophylaxis; Needs high-fat meal
⭐ Voriconazole: Drug of Choice (DOC) for invasive Aspergillosis; Therapeutic Drug Monitoring (TDM) recommended.
📌 All Zoles Often Lead to Elevated SG enzymes (Hepatotoxicity).
Echinocandins - Glucan Wall Wreckers
- Mechanism: Potently inhibit $β-(1,3)$-D-glucan synthase, disrupting fungal cell wall integrity. 📌 "Glucan Wall Wreckers".
- Spectrum: Fungicidal against most Candida spp. (incl. azole-resistant); fungistatic against Aspergillus spp.
- No activity: Cryptococcus neoformans, Zygomycetes (e.g., Mucor).
- PK: IV administration only. Favorable safety profile; few significant drug interactions (minimal CYP450).
- Agents: Caspofungin, Micafungin, Anidulafungin.
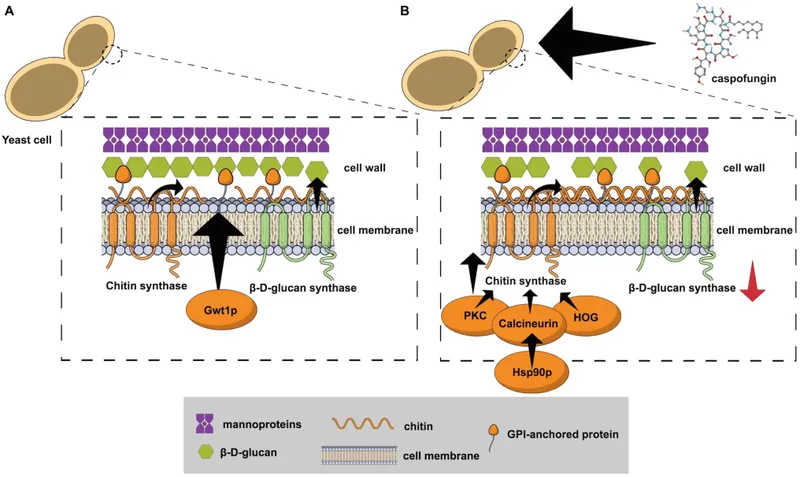
⭐ Echinocandins are often first-line for empiric therapy of invasive candidiasis in critically ill patients, especially if azole resistance is suspected.
Other Antifungals - The Unique Crew
- Flucytosine (5-FC)
- MOA: Converted by fungal enzymes to $5-Fluorouracil$ ($5-FU$), which inhibits thymidylate synthase → ↓ DNA & RNA synthesis.
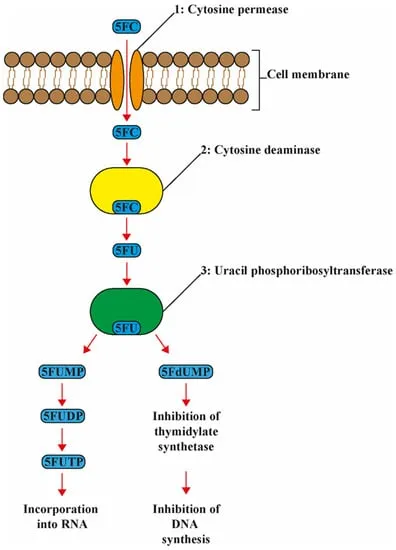
- Use: Synergy with Amphotericin B for cryptococcal meningitis.
- Toxicity: Bone marrow suppression (dose-related).
- MOA: Converted by fungal enzymes to $5-Fluorouracil$ ($5-FU$), which inhibits thymidylate synthase → ↓ DNA & RNA synthesis.
- Griseofulvin
- MOA: Disrupts fungal mitotic spindle by interacting with microtubules.
- Use: Dermatophytoses (tinea capitis, corporis). 📌 "Greasy" for skin/hair/nails.
- DDI: Induces CYP450 → ↓ warfarin efficacy.
- Terbinafine
- MOA: Inhibits squalene epoxidase → ↓ ergosterol synthesis & ↑ toxic squalene.
- Use: Dermatophytoses, onychomycosis (excellent nail penetration).
- Toxicity: GI distress, hepatotoxicity (monitor LFTs).
⭐ Terbinafine is fungicidal and accumulates in keratinized tissues like skin, hair, and nails, making it highly effective for superficial infections there.
High‑Yield Points - ⚡ Biggest Takeaways
- Amphotericin B: Broadest spectrum; nephrotoxicity is dose-limiting. Liposomal forms reduce toxicity.
- Azoles: Inhibit ergosterol synthesis (14-α-demethylase). Significant drug interactions (CYP450 inhibition).
- Voriconazole: DOC for invasive Aspergillosis. Causes visual disturbances and photosensitivity.
- Echinocandins: Inhibit β-(1,3)-D-glucan synthesis (cell wall). Effective against Candida and Aspergillus.
- Terbinafine: Accumulates in keratin. For dermatophytoses/onychomycosis. Inhibits squalene epoxidase.
- Flucytosine: Converted to 5-FU; synergistic with Ampho B. Risk of bone marrow suppression.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

