Intro & MOA - Mighty Microbe Mincers
- Potent bactericidal antibiotics.
- Spectrum: Primarily aerobic Gram-negative bacilli.
- Mechanism of Action (MOA):
- Irreversibly bind to the bacterial 30S ribosomal subunit.
- Interfere with protein synthesis:
- Block initiation complex formation.
- Cause mRNA misreading, leading to abnormal protein insertion.
- Block translocation of peptidyl-tRNA.
- Exhibit concentration-dependent killing (↑ conc. = ↑ killing rate).
- Long Post-Antibiotic Effect (PAE).
- Oxygen-dependent uptake (ineffective against anaerobes).
- 📌 Examples: Gentamicin, Neomycin, Amikacin, Tobramycin, Streptomycin (GNATS).
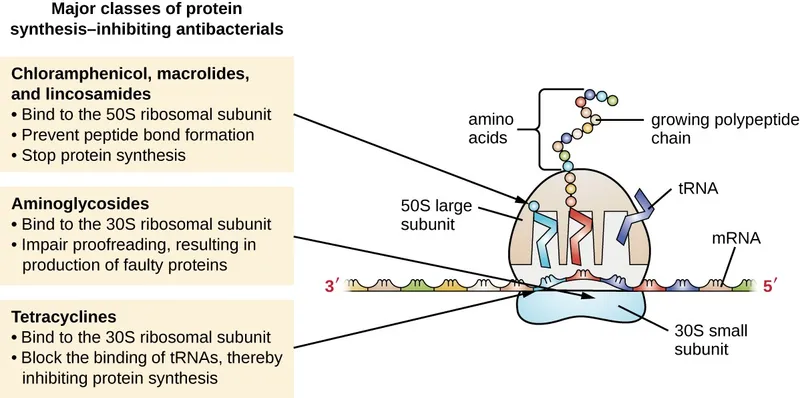
⭐ Aminoglycosides cause misreading of mRNA and block translocation, leading to bactericidal action primarily against aerobic Gram-negative bacteria.
PK/PD Properties - Journey & Jolt
- Pharmacokinetics (Journey - ADME):
- Absorption: Poor oral (highly polar); IV/IM administration.
- Distribution: Accumulates in renal cortex & inner ear (⚠️ nephro/ototoxicity risk).
- Metabolism: Negligible.
- Excretion: Renal, via glomerular filtration (unchanged). Adjust dose in renal failure.
- Pharmacodynamics (Jolt - Effects):
- Killing: Concentration-Dependent Killing (CDK) - higher $C_{max}$ = faster kill.
- Duration: Significant Post-Antibiotic Effect (PAE) - suppression post-MIC drop.
- Dosing Rationale:
- Once-Daily Dosing (ODD) preferred:
- Maximizes CDK with high peaks.
- Utilizes PAE for sustained effect.
- Minimizes toxicity (drug-free interval for washout from kidney/ear).
- Once-Daily Dosing (ODD) preferred:
⭐ Once-daily dosing regimens leverage concentration-dependent killing and post-antibiotic effect to maximize efficacy and minimize nephrotoxicity.
Clinical Uses & Spectrum - Germ Warfare Gurus
-
Core Spectrum: Serious aerobic Gram-negative bacilli infections (Pseudomonas aeruginosa, E. coli, Klebsiella).
-
Synergy: With β-lactams/Vancomycin for Gram-positive endocarditis (Enterococcus, Staphylococcus).
-
Specific Pathogen Coverage:
Aminoglycoside Key Indications Streptomycin Tuberculosis (TB), Plague, Tularemia Gentamicin Plague, Tularemia, Serious Gram-negative sepsis Amikacin TB (MDR), Gentamicin-resistant Gram-negatives Neomycin Bowel sterilization (oral), Topical infections Tobramycin Pseudomonas aeruginosa infections (esp. lungs)
⭐ Aminoglycosides are crucial in combination therapy with cell wall synthesis inhibitors (like penicillin or vancomycin) for synergistic bactericidal activity against certain Gram-positive cocci, especially in endocarditis.
Adverse Effects - Toxic Trio Alert
📌 NNN: Nephrotoxic, Neurotoxic (ototoxic), Neuromuscular blockade.
- Nephrotoxicity:
- Reversible acute tubular necrosis (ATN).
- Monitor: Serum creatinine, BUN. Ensure hydration.
- Ototoxicity:
- Irreversible auditory (cochlear: hearing loss, tinnitus) & vestibular (vertigo, ataxia) damage.
- Dose-related. Monitor audiometry in high-risk/long therapy.
- Neuromuscular Blockade:
- Rare; risk of respiratory paralysis.
- Risk factors: Myasthenia gravis, rapid IV infusion, concurrent neuromuscular blockers, hypocalcemia.
- Treatment: IV Calcium gluconate or neostigmine.
⭐ Ototoxicity from aminoglycosides can be irreversible and may manifest as hearing loss (cochlear damage) or vertigo/ataxia (vestibular damage).
Resistance & Interactions - Defense Breachers
- Resistance Mechanisms:
- Enzymatic modification (acetylation, phosphorylation, adenylation) - most common.
- Impaired entry.
- Altered ribosomal binding.
- Key Interactions & Cautions:
- Loop diuretics: ↑ ototoxicity.
- Vancomycin/Amphotericin B: ↑ nephrotoxicity.
- Neuromuscular blockers: ↑ blockade.
- Pregnancy: Category D. ⚠️
⭐ Most common resistance: enzymatic drug inactivation by bacterial enzymes.
High‑Yield Points - ⚡ Biggest Takeaways
- Bactericidal; irreversibly bind 30S ribosome, inhibiting protein synthesis.
- Spectrum: Aerobic Gram-negative bacilli (e.g., Pseudomonas); synergistic with β-lactams.
- Major toxicities: Nephrotoxicity (reversible ATN), Ototoxicity (irreversible; cochlear & vestibular), Neuromuscular blockade.
- Administered IV/IM (poor oral absorption); exhibit significant post-antibiotic effect.
- Resistance: Primarily via enzymatic modification (acetylation, phosphorylation).
- Therapeutic Drug Monitoring (TDM) essential due to narrow therapeutic index.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

