Overview & MoA - Cycle's Hitmen
- Microbial-derived (e.g., Streptomyces). Disrupt DNA/RNA synthesis/function, halting cell cycle, inducing apoptosis.
- Key Mechanisms:
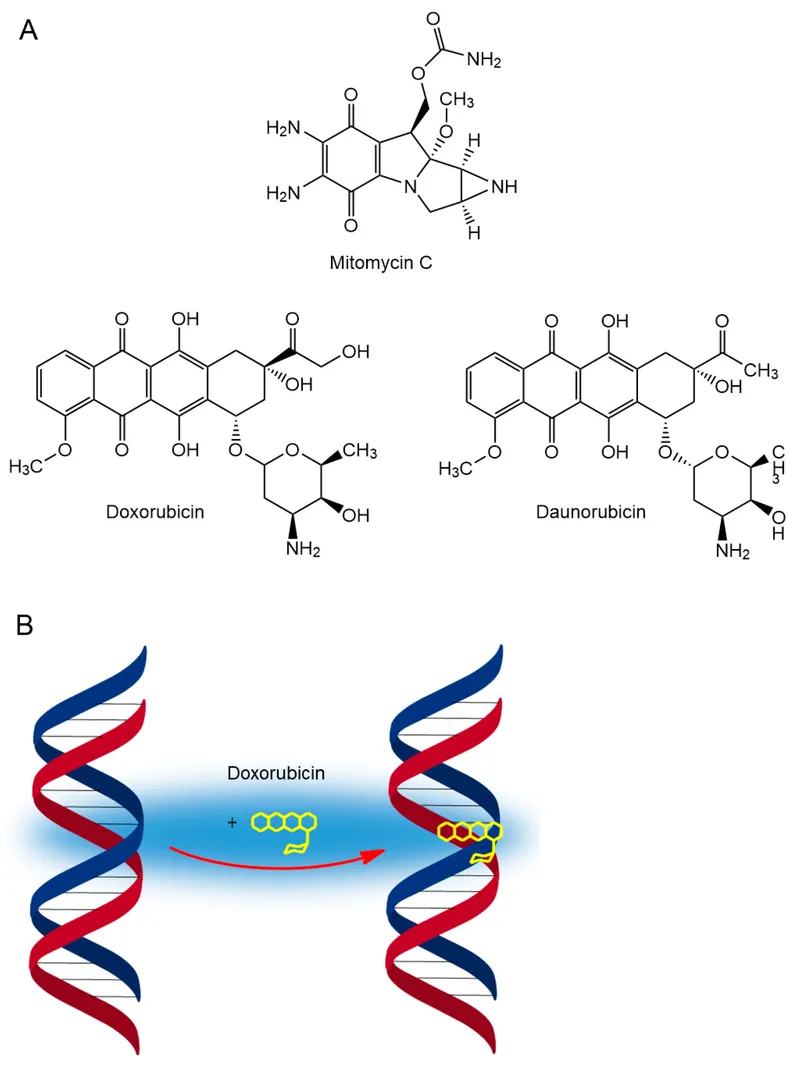
- DNA Intercalation: Wedge between DNA base pairs, distorting structure, blocking replication/transcription (e.g., Dactinomycin, Doxorubicin).
- Free Radical Generation: ROS cause DNA strand breaks (e.g., Doxorubicin, Bleomycin).
- Topoisomerase II Inhibition: Stabilize enzyme-DNA complex, preventing DNA break re-ligation (e.g., Doxorubicin, Mitoxantrone).
- DNA Alkylation: Covalently bind DNA, causing cross-links (e.g., Mitomycin C).
- DNA Strand Scission: Directly cleave DNA strands (e.g., Bleomycin, needs $Fe^{2+}$).

⭐ Doxorubicin's major dose-limiting toxicity is cardiotoxicity (free radical mediated). Dexrazoxane can be used for cardioprotection. 📌 Bleomycin: Breaks DNA, specific for G2-M phase.
Anthracyclines - Ruby Red Risks
Derived from Streptomyces peucetius var. caesius. Potent broad-spectrum agents.
- Examples: Doxorubicin, Daunorubicin, Epirubicin, Idarubicin.
- 📌 "Ruby Red" drugs: Cause red urine.
Mechanism of Action (MoA):
- Intercalates DNA → blocks DNA/RNA synthesis.
- Inhibits Topoisomerase II → DNA strand breaks.
- Generates ROS (free radicals) → cardiotoxicity.
Clinical Uses:
- Leukemias (AML), lymphomas (Hodgkin's, NHL).
- Solid tumors: Breast, ovarian, lung, sarcomas.
Key Toxicities:
- Cardiotoxicity (Dose-Limiting):
- Acute: Arrhythmias, pericarditis-myocarditis (reversible).
- Chronic: Dose-dependent DCM (irreversible).
- ROS-mediated myocyte damage.
- Monitor: LVEF (ECHO/MUGA) baseline & periodic.
- Prevention: Dexrazoxane (iron chelator).
- Myelosuppression (dose-limiting).
- Mucositis, stomatitis.
- Alopecia.
- Extravasation → tissue necrosis.
- Radiation recall.
⭐ Doxorubicin max cumulative dose: 450-550 mg/m² (Daunorubicin ~550 mg/m²) to limit irreversible heart failure. Dexrazoxane: cardioprotectant.
Bleomycin - Lung's Nemesis
- Mechanism: DNA strand scission via oxidative damage; forms complex with Fe²⁺ & O₂, generating free radicals. Cell cycle specific (G2 phase).
- Uses:
- Testicular cancers (e.g., BEP regimen)
- Hodgkin's lymphoma (e.g., ABVD regimen)
- Squamous cell carcinomas (head & neck, skin, cervix)
- Malignant pleural effusion (sclerosing agent)
- Adverse Effects:
- Pulmonary fibrosis: Dose-dependent (cumulative dose > 400 units). 📌 "BLOW-mycin" for lung toxicity.
- Skin: Hyperpigmentation (flagellate rash), hyperkeratosis.
- Mucositis, fever, allergic reactions.
- Minimal myelosuppression.
⭐ Bleomycin causes severe, potentially fatal pulmonary fibrosis, especially at cumulative doses exceeding 400 units; it is notably sparing of bone marrow.
- Key Feature: Low levels of inactivating enzyme (bleomycin hydrolase) in lungs & skin contribute to toxicity.
 oka
oka
Other Key Agents - Diverse Attackers
-
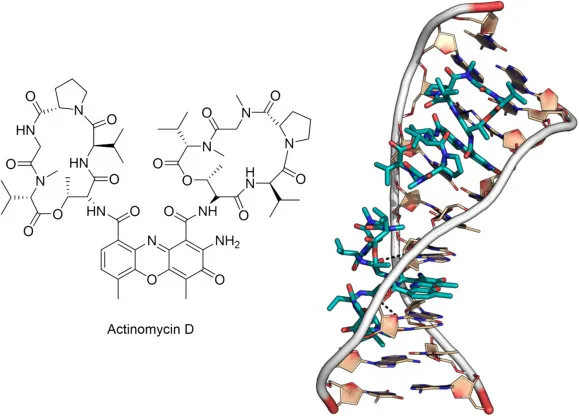
Dactinomycin (Actinomycin D)
- MoA: Intercalates between Guanine-Cytosine (G-C) base pairs in DNA; blocks DNA-dependent RNA polymerase. Halts transcription.
- Uses: Key for pediatric cancers: Wilms' tumor, Ewing's sarcoma, rhabdomyosarcoma. Also gestational choriocarcinoma. 📌 Dactinomycin: "D" for DNA; "Actino-" for Acting on kids' tumors.
- Toxicity: Severe myelosuppression, N/V, mucositis, alopecia.
⭐ Characteristic: Radiation recall phenomenon (inflammation at prior irradiated sites).
-
Mitomycin C
- MoA: Prodrug; bioreductively activated (esp. in hypoxic cells) to a bifunctional alkylating agent. Induces DNA cross-linking.
- Uses: Hypoxic solid tumors (stomach, pancreas, bladder, anal). Intravesical instillation for superficial bladder cancer.
- Toxicity: Delayed, cumulative myelosuppression (esp. thrombocytopenia). HUS (microangiopathic hemolytic anemia, thrombocytopenia, ARF). Interstitial pneumonitis.
High‑Yield Points - ⚡ Biggest Takeaways
- Anthracyclines (e.g., Doxorubicin): Dose-dependent cardiotoxicity (use Dexrazoxane), red urine.
- Bleomycin: Pulmonary fibrosis, skin changes, minimal myelosuppression. For testicular cancer, Hodgkin's.
- Dactinomycin (Actinomycin D): Key for pediatric tumors (Wilms', Ewing's, Rhabdomyosarcoma).
- Mitomycin C: Severe myelosuppression, risk of Hemolytic Uremic Syndrome (HUS).
- Plicamycin (Mithramycin): Treats hypercalcemia of malignancy; hepatotoxic.
- Anthracycline MOA: DNA intercalation, free radical formation, topoisomerase II inhibition.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

