Etiopathogenesis & Spectrum - Tiny Invader, Big Trouble
- Etiology: Mycobacterium tuberculosis (MTB), an acid-fast, obligate aerobic bacillus.
- Transmission: Primarily airborne via droplet nuclei from adults with sputum-positive pulmonary TB (PTB). Ingestion of unpasteurized milk (bovine TB) is rare.
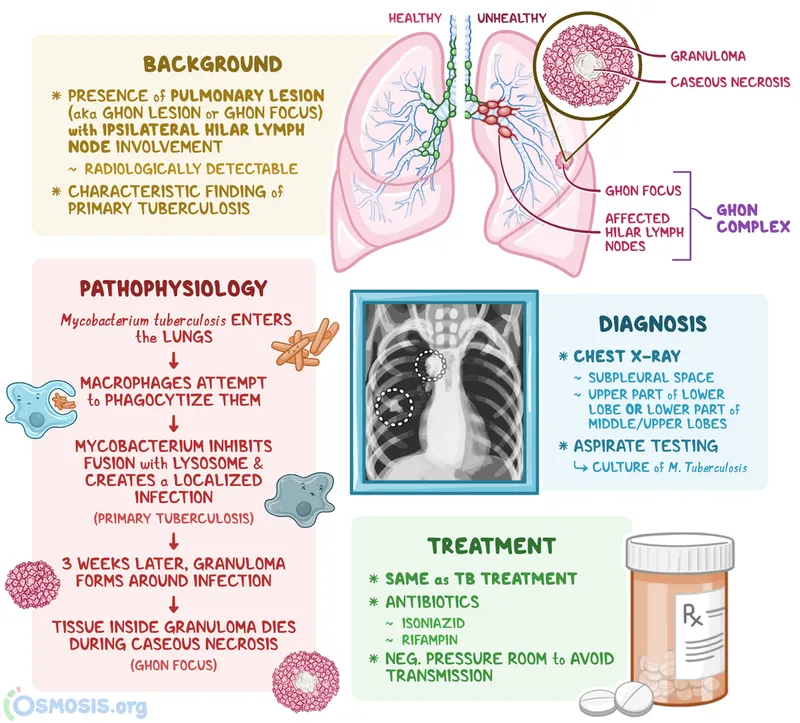
- Pathogenesis: Inhalation → alveolar macrophage engulfment → lymphatic spread → Ghon focus (lung lesion) + regional lymphadenitis = Primary Complex.
- Spectrum:
- TB Infection (latent): Positive TST/IGRA, no symptoms, normal CXR.
- TB Disease: Symptomatic, abnormal CXR/findings.
- Pulmonary TB: Primary complex, progressive primary disease, miliary TB.
- Extrapulmonary TB (EPTB): Lymph node TB (most common EPTB), CNS TB, bone/joint TB.
⭐ Children, especially < 5 years, are more prone to disseminated forms (miliary TB, TBM) and rapid progression from infection to disease compared to adults due to immature immunity.
Clinical Clues & Red Flags - Spotting Sneaky Bug
- Persistent Cough: >2-3 weeks (cardinal symptom), often non-productive.
- Prolonged Unexplained Fever: >1 week, often low-grade, evening rise.
- Weight Loss/Failure to Thrive: Documented growth faltering.
- Fatigue/Lethargy: Reduced playfulness, easy tiredness.
- Contact Hx: Exposure to adult TB case = ⚠️ MAJOR RED FLAG.
- Extrapulmonary TB (EPTB) common:
- Lymphadenitis (Scrofula): Painless, matted nodes (often cervical). Most common EPTB.
- TB Meningitis (TBM): Insidious; headache, vomiting, irritability, seizures. ⚠️ High risk!
- Abdominal: Pain, distension, doughy abdomen.
- Skeletal (e.g., Pott's spine): Back pain, stiffness, deformity.
- Miliary (Disseminated): High fever, hepatosplenomegaly, respiratory distress. CXR: "millet seed".
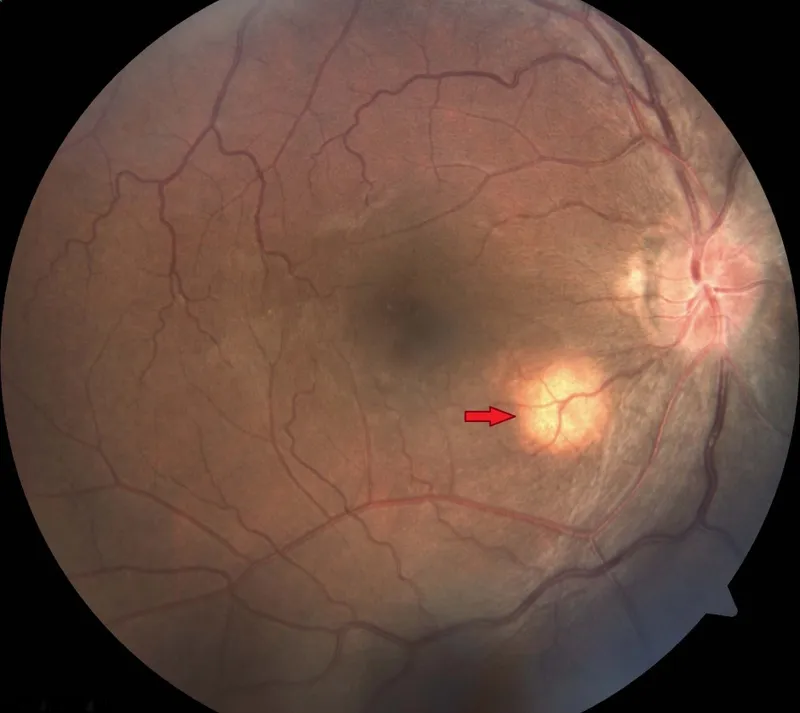
- Fundoscopy: Choroidal tubercles.
- Other Clues:
- No improvement with standard antibiotics for pneumonia.
- HIV co-infection, severe malnutrition.
- Erythema nodosum, phlyctenular conjunctivitis.
⭐ Choroidal tubercles on fundoscopy are pathognomonic for miliary TB.
Diagnostic Drill-Down - Unmasking the Culprit
- Screening:
- Tuberculin Skin Test (TST): Induration ≥10mm (BCG unimmunized/ >1yr post-BCG); ≥5mm (HIV+, immunosuppressed, close contact, severe malnutrition).
⭐ A positive TST indicates TB infection, not active disease; clinical correlation vital.
- IGRAs (Interferon-Gamma Release Assays): Preferred if BCG vaccinated.
- Tuberculin Skin Test (TST): Induration ≥10mm (BCG unimmunized/ >1yr post-BCG); ≥5mm (HIV+, immunosuppressed, close contact, severe malnutrition).
- Microbiological Confirmation:
- Specimens: Sputum (older children), Gastric aspirate/lavage (3x, young children), induced sputum.
- AFB Smear (ZN stain): Rapid, low sensitivity.
- Culture (LJ Medium): Gold standard, 4-8 weeks.
- NAAT (CBNAAT/GeneXpert): Rapid (<2 hrs), detects M.tb & Rif-resistance. WHO recommended 1st test for all peds TB suspects.
- Imaging:
- CXR: Hilar lymphadenopathy (commonest), Ghon complex, consolidation, miliary.
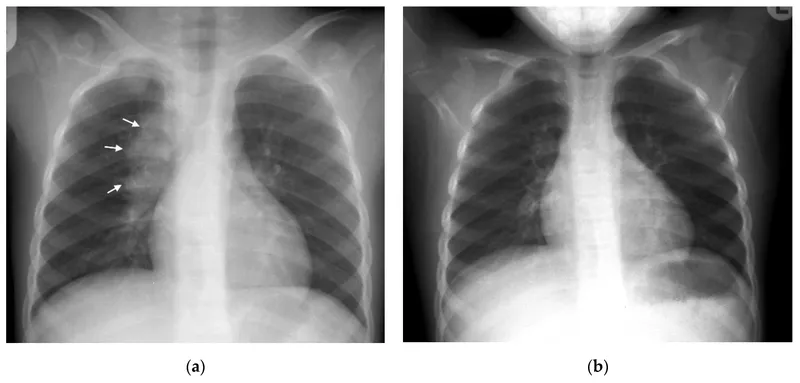
- CXR: Hilar lymphadenopathy (commonest), Ghon complex, consolidation, miliary.
Treatment & Prevention - Kicking TB Out!
- Goal: Cure, prevent death/disability, cut transmission, prevent drug resistance. DOTS essential.
Drug-Sensitive TB (DS-TB): Daily Fixed-Dose Combinations (FDCs).
- New Cases:
- Intensive Phase (IP): 2 months HRZE.
- Continuation Phase (CP): 4 months HR.
- Total: 6 months. Weight-band dosing.
- Severe forms (TBM, miliary): Longer CP (10 months HR), corticosteroids.
Drug-Resistant TB (DR-TB):
- Per National TB Elimination Program (NTEP) guidelines. Longer, specialized drugs.
Prevention:
- BCG Vaccination: At birth, 0.05 mL ID (<1m) / 0.1 mL ID (≥1m), left upper arm.
- TB Preventive Treatment (TPT):
- Isoniazid (H) daily for 6 months for eligible contacts (<5 yrs, HIV+).
- Alternative: 3HP (weekly H + Rifapentine for 3 months).
- Infection Control: Cough hygiene, ventilation.
⭐ BCG vaccine primarily protects against severe disseminated TB forms (e.g., meningitis, miliary) in children.
High‑Yield Points - ⚡ Biggest Takeaways
- Mantoux test (TST): 5 TU PPD-S; ≥10mm positive (≥5mm in HIV/contacts/malnourished).
- Gastric lavage/induced sputum for diagnosis (AFB, culture, NAAT).
- Primary progressive TB is common in children <5 years.
- Miliary TB & TB meningitis (TBM) are severe forms with high mortality.
- DOTS strategy: RHZE for intensive phase (2 months), followed by RH for continuation.
- BCG vaccine protects against severe forms (TBM, miliary), not primary infection.
- Contact tracing & Isoniazid prophylaxis for eligible contacts are vital.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

