PFT Intro & Spirometry Basics - Kiddo Lung Check
- Purpose: Evaluate lung function; diagnose/monitor diseases (asthma, CF). Non-invasive.
- Spirometry: Measures air volume & flow during forced exhalation.
- Key Parameters:
- FVC (Forced Vital Capacity): Total air forcefully exhaled after max inspiration.
- FEV1 (Forced Expiratory Volume in 1st sec).
- $FEV_1/FVC$ Ratio: Normal > 0.8. Differentiates patterns.
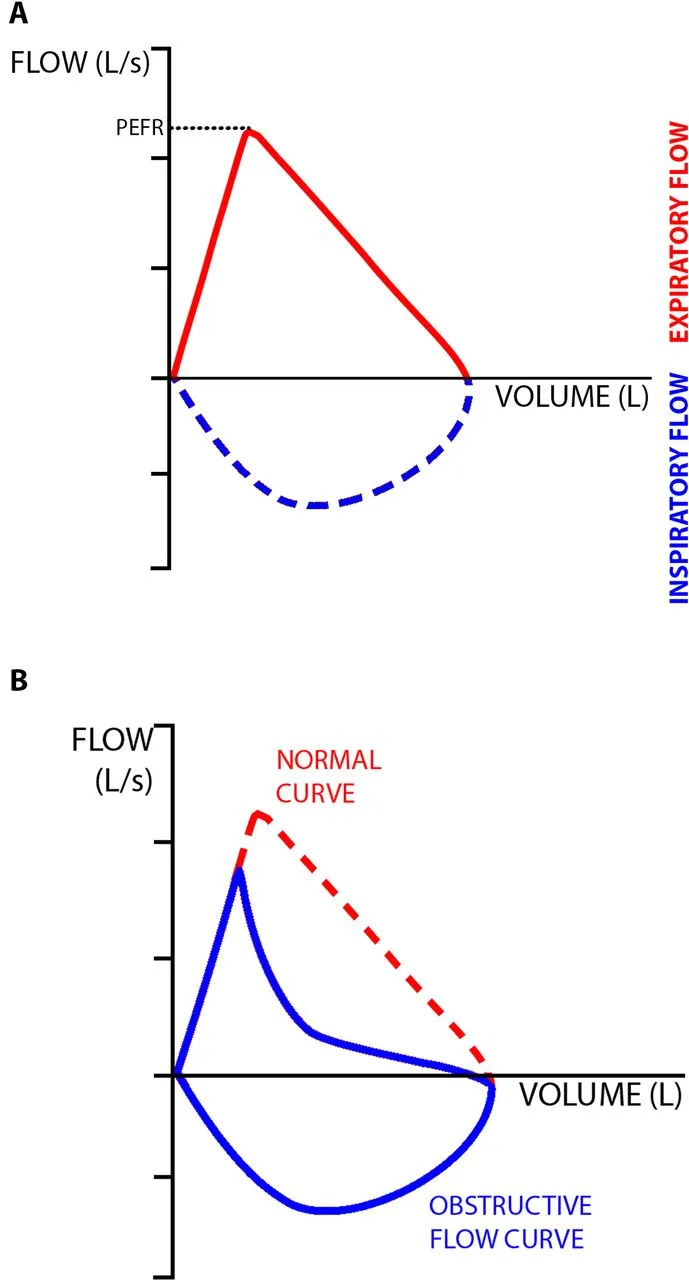
- PEFR (Peak Expiratory Flow Rate): Max flow rate.
- Indications: Asthma, CF, neuromuscular disease, pre-op.
- Interpretation:
- 📌 Obstructive: ↓$FEV_1/FVC$ (e.g., Asthma). "Can't get air Out".
- 📌 Restrictive: ↓FVC, normal/↑$FEV_1/FVC$ (e.g., Fibrosis). "Reduced lung volumes".
- Key Parameters:
⭐ Cooperation is key: most children can perform reliable spirometry by age 5-6 years.
Spirometry Interpretation & Patterns - Airflow Clues
Key parameters: $FEV_1$ (Forced Expiratory Volume in 1s), $FVC$ (Forced Vital Capacity), $FEV_1/FVC$ ratio, $FEF_{25-75%}$ (Forced Expiratory Flow 25-75%).
- Obstructive Pattern:
- $FEV_1$: ↓↓
- $FVC$: N or ↓
- $FEV_1/FVC$: < 0.7 (Key indicator)
- $FEF_{25-75%}$: ↓↓ (Small airway disease)
- Flow-Volume Loop: Concave/'scooped-out' expiratory limb.
- Restrictive Pattern:
- $FEV_1$: ↓
- $FVC$: ↓↓
- $FEV_1/FVC$: N or ↑ (typically >0.7)
- $FEF_{25-75%}$: N or ↓ (proportionate to $FVC$)
- Flow-Volume Loop: Shrunken, "witch's hat" appearance; preserved shape but smaller. Peak flow ↓.
- Mixed Pattern:
- $FEV_1$: ↓↓
- $FVC$: ↓↓
- $FEV_1/FVC$: < 0.7
- Flow-Volume Loop: Features of both obstructive and restrictive.
⭐ A 'scooped-out' appearance on the expiratory limb of the flow-volume loop is characteristic of obstructive lung disease.
Lung Volumes & Bronchodilator Response - Puff & Proof
- Total Lung Capacity (TLC): Max air lungs hold. $TLC = VC + RV$.
- Vital Capacity (VC): Max air exhaled after deepest breath. $VC = TV + IRV + ERV$.
- Residual Volume (RV): Air left post-max exhalation. Measured by Helium dilution/Plethysmography. $\uparrow$ in obstruction.
- Functional Residual Capacity (FRC): Air after normal exhalation. $FRC = ERV + RV$. Resting lung volume.
- Tidal Volume (TV): Air per normal breath.
- Inspiratory/Expiratory Reserve Volume (IRV/ERV): Extra air inhaled/exhaled beyond TV.
Bronchodilator Response (BDR):
- Assesses airway reversibility, crucial for asthma diagnosis.
- Procedure: Baseline spirometry $\rightarrow$ Inhaled short-acting $\beta2$-agonist (SABA) $\rightarrow$ Repeat spirometry after 10-20 min.
- Positive Response (Children):
- $\uparrow$ FEV1 by >12% from pre-bronchodilator value.
- 📌 Puff & Proof: Puff SABA, see Proof of reversibility.
⭐ A post-bronchodilator increase in FEV1 by >12% signifies significant reversibility in children.
Special PFTs & Clinical Links - Tiny Lung Detectives
- FeNO (Fractional exhaled Nitric Oxide):
- Eosinophilic airway inflammation marker.
- Predicts ICS response.
⭐ Elevated FeNO (e.g., >20 ppb in children) suggests eosinophilic airway inflammation and predicts ICS responsiveness.
- Impulse Oscillometry (IOS):
- Measures airway resistance/reactance.
- Minimal cooperation; for young kids.
- Detects peripheral airway obstruction.
- Multiple Breath Washout (MBW):
- Measures Lung Clearance Index (LCI).
- Detects ventilation inhomogeneity.
- Sensitive for early CF lung disease.
- CPET (Cardiopulmonary Exercise Test):
- Assesses exercise limitation (cardiac/pulmonary).
- Measures $V_{ ext{O}_2}$ max.
- Clinical Links:
- Asthma: FeNO, IOS.
- CF: LCI (MBW).
- EIB: Exercise challenge with PFTs.
High‑Yield Points - ⚡ Biggest Takeaways
- Spirometry assesses airflow obstruction (e.g., asthma) and restriction (e.g., neuromuscular disease).
- FEV1/FVC ratio < 0.7 or < 5th percentile indicates obstruction.
- Reduced FVC with a normal or increased FEV1/FVC ratio suggests restriction.
- Bronchodilator reversibility (↑ FEV1 by > 12% and 200 mL) confirms asthma.
- Peak Expiratory Flow Rate (PEFR) is useful for monitoring asthma severity and response to treatment.
- Lung volumes (e.g., TLC, RV) help differentiate restrictive patterns and assess air trapping.
- Diffusion capacity (DLCO) is ↓ in interstitial lung diseases and pulmonary vascular disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

