Pleural Effusion - Fluid Follies
- Abnormal fluid in pleural space. Types: Transudate (systemic factors) vs. Exudate (local factors).
- Diagnosis: Thoracentesis, imaging (CXR, USG).
| Feature | Transudate | Exudate |
|---|---|---|
| Appearance | Clear | Cloudy/Bloody |
| Protein | < 3 g/dL | > 3 g/dL |
| LDH | < 200 IU/L | > 200 IU/L |
| Pleural/Serum Prot. | < $ extbf{0.5}$ | > $ extbf{0.5}$ |
| Pleural/Serum LDH | < $ extbf{0.6}$ | > $ extbf{0.6}$ |
| Pleural LDH | < $\frac{\textbf{2}}{\textbf{3}}$ ULN serum | > $\frac{\textbf{2}}{\textbf{3}}$ ULN serum |
| Causes | CCF, Cirrhosis, Nephrotic | Pneumonia, TB, Malignancy |
* Pleural Protein/Serum Protein > $\textbf{0.5}$
* Pleural LDH/Serum LDH > $\textbf{0.6}$
* Pleural LDH > $\frac{\textbf{2}}{\textbf{3}}$ ULN (serum)
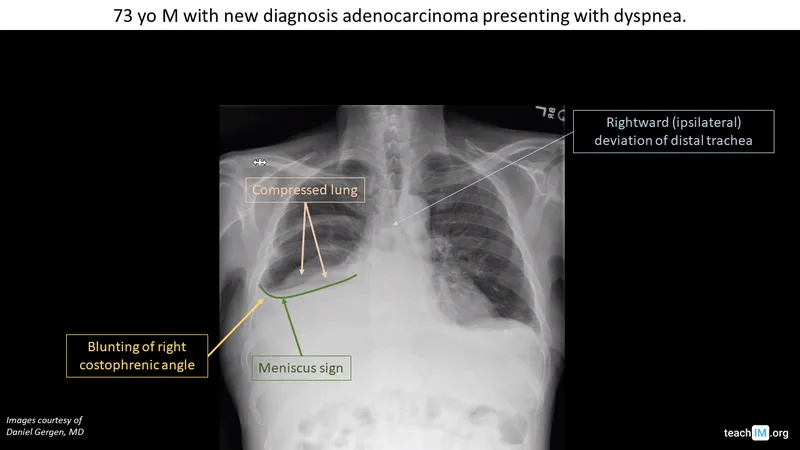
⭐ Tuberculosis is a leading cause of exudative pleural effusion in children in endemic areas like India.
Empyema Thoracis - Pus Under Pressure
Pus in pleural space, a serious complication of pneumonia.
- Etiology: S. pneumoniae (MC), S. aureus (esp. post-flu), H. influenzae.
- Stages (📌 EFO: Exudative, Fibrinopurulent, Organizing):
- 1. Exudative: Simple effusion. Fluid: pH > 7.2, Glc > 60 mg/dL, LDH < 1000 IU/L. Antibiotics alone.
- 2. Fibrinopurulent: Pus. Fluid: pH < 7.2, Glc < 40 mg/dL, LDH > 1000 IU/L, +ve Gram/culture. Drainage essential.
⭐ Surgical Indications (VATS/Decortication): Failed initial drainage, multiloculations, thick peel, bronchopleural fistula, chronic (>4-6 wks).
- 3. Organizing: Thick inelastic peel, lung trapped. Decortication often needed.
- Diagnosis: CXR (D-shape), USG (locules, guides tap), CT for complex cases. Pleural tap vital.

- Management Algorithm:
Pneumothorax - Air Scare
- Definition: Air in pleural space, leading to lung collapse.
- Types: Spontaneous (Primary - no underlying disease; Secondary - due to lung disease), Traumatic, Iatrogenic.
- Clinical Features: Sudden onset dyspnea, pleuritic chest pain, ↓ breath sounds, hyperresonant percussion note. Tension Pneumothorax: Tracheal deviation (away from affected side), hypotension, distended neck veins, severe respiratory distress. 📌 BATTS for tension: Breathlessness, Agitation, Tracheal deviation, Tachycardia, Sweating.
- Diagnosis: CXR (visceral pleural line, absent lung markings peripherally). Ultrasound (absent lung sliding - "barcode sign").

- Management Principles:
- Small Primary Spontaneous Pneumothorax (PSP) (<2-3cm rim of air, stable patient): Observation, supplemental O2.
- Large PSP (≥2-3cm rim) or symptomatic / Secondary Spontaneous Pneumothorax (SSP): Needle aspiration or chest tube (ICD) insertion.
- Recurrent / Persistent air leak / Bilateral / High-risk professions: Pleurodesis (chemical/surgical).
⭐ Tension Pneumothorax is a medical emergency! Immediate life-saving step is needle decompression (e.g., large bore cannula in 2nd intercostal space, mid-clavicular line or 4th/5th intercostal space, anterior axillary line), followed by definitive chest tube drainage.
Special Effusions - Milky & Bloody
Chylothorax (Milky Fluid)
- Patho: Lymphatic fluid (chyle) in pleura.
- Causes: Trauma (post-surgery, birth); Non-traumatic (malignancy, congenital).
- Diagnosis: Milky fluid; TG > 110 mg/dL; Chylomicrons. TG/Chol > 1. Lymphocytic.
- vs. Pseudochylothorax (chronic, ↑Cholesterol, no chylomicrons, crystals).
- Management: Conservative (NPO, TPN, MCT diet, octreotide); Drainage; Surgery (pleurodesis, duct ligation).
⭐ Most common cause of non-traumatic chylothorax in neonates is congenital lymphatic malformations.
Hemothorax (Bloody Fluid)
- Patho: Blood in pleura.
- Causes: Trauma (commonest), iatrogenic, malignancy.
- Diagnosis: Pleural fluid Hct > 50% blood Hct. CXR/CT confirms.
- Management: Tube thoracostomy. Surgery (VATS/thoracotomy) if:
- Initial drain > 1500 mL or > 20 mL/kg.
- Ongoing bleed > 200 mL/hr (2-4 hrs).
High‑Yield Points - ⚡ Biggest Takeaways
- Pleural effusion: Transudates (heart failure, nephrotic syndrome) vs. Exudates (parapneumonic, TB).
- Light's criteria help differentiate, but clinical picture is vital in children.
- Empyema (pus) requires antibiotics and chest drainage; often follows bacterial pneumonia.
- Chylothorax: milky fluid, high triglycerides; causes include surgery, congenital issues.
- Pneumothorax: air in pleural space. Tension pneumothorax is an emergency needing urgent decompression.
- Tuberculous effusion: common in endemic settings, a lymphocytic exudate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

