EA/TEF: Intro & Embryology - Tube Trouble Tales
- Definition: Esophageal Atresia (EA) refers to a congenitally interrupted esophagus (blind pouch). Tracheoesophageal Fistula (TEF) is an abnormal connection between the trachea and esophagus.
- Incidence: Occurs in approximately 1 in 3000-5000 live births.
- Embryology - The "Tube" Defect:
- Results from defective lateral septation of the embryonic foregut into the esophagus and trachea.
- Critical period: 4th-6th week of gestation.
- Failure of tracheoesophageal folds to fuse correctly.
- Associated Anomalies: Common (~50% of cases).
- 📌 VACTERL association is key: Vertebral defects, Anal atresia, Cardiac defects, Tracheo-Esophageal fistula, Renal anomalies, Limb abnormalities.
- 📌 VACTERL association is key: Vertebral defects, Anal atresia, Cardiac defects, Tracheo-Esophageal fistula, Renal anomalies, Limb abnormalities.
⭐ Maternal polyhydramnios is a common prenatal indicator, seen in nearly two-thirds of EA cases due to impaired fetal swallowing of amniotic fluid.
EA/TEF: Classification - Alphabet Soup Anatomy
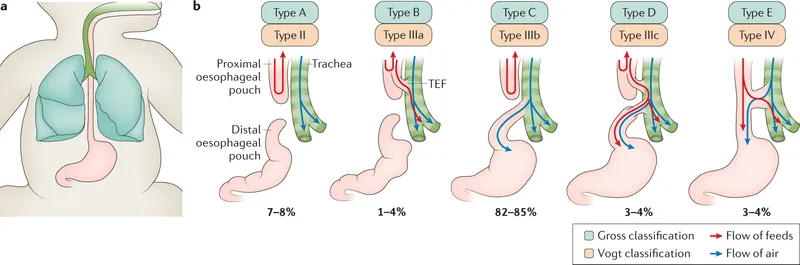
Anatomical variations are classified using the Gross system:

| Type | Description (Anatomy) | Frequency (%) | Gas in GI |
|---|---|---|---|
| A | Esophageal Atresia (EA) without fistula (pure atresia) | 5-8 | No |
| B | EA with proximal Tracheoesophageal Fistula (TEF) | <1 | No |
| C | EA with distal TEF | ~85-90 | Yes |
| D | EA with both proximal and distal TEF | <1 | Yes |
| E | TEF without EA (H-type fistula) | 4 | Yes |
⭐ Gross Type C (atresia with distal fistula) is the most common type (~85-90%), crucial for predicting initial X-ray findings (gas in bowel).
EA/TEF: Clinical Presentation & Diagnosis - Spotting the Signs
- Clinical Clues:
- Excessive frothy saliva, drooling (sialorrhea) - often earliest sign.
- 📌 3 C's: Coughing, Choking, Cyanosis, especially with feeds.
- Respiratory distress, potential aspiration.
- Abdominal distension (if distal TEF present, air in stomach).
- Maternal polyhydramnios (significant antenatal clue).
- Diagnostic Confirmation:
- Inability to pass NG/OG tube beyond 10-12 cm.
- X-ray (Chest & Abdomen, AP view):
- Coiled NG tube in blind upper esophageal pouch.
- Distal gas (air in stomach/bowel): Confirms distal TEF (e.g., Type C).
- Gasless abdomen: Suggests pure EA or EA with proximal TEF.
⭐ The pathognomonic sign is the inability to pass an orogastric tube into the stomach, confirmed by X-ray showing the tube coiled in the upper esophageal pouch.
EA/TEF: Management & Complications - Mending the Gap
- Pre-operative Stabilization:
- NPO, continuous upper pouch suction (Replogle tube).
- Position: Head up (30-45°) to prevent aspiration.
- IV fluids, broad-spectrum antibiotics. Screen for VACTERL.
- Surgical Correction (Definitive):
- Primary repair: Thoracotomy/thoracoscopy for TEF ligation & end-to-end esophageal anastomosis.
- Staged repair for long gaps (>3-4 cm) or unstable neonate: Gastrostomy, delayed repair.
- Post-operative Care:
- Ventilatory support prn, chest drain.
- Contrast swallow study (e.g., Gastrografin) around day 5-7 before oral feeds.
- Parenteral nutrition initially.
- Complications:
- Early: Anastomotic leak (most serious), stricture, recurrent fistula, chylothorax.
- Late: GERD (nearly universal), tracheomalacia (barking cough, respiratory distress), esophageal dysmotility, dysphagia.
⭐ Tracheomalacia is a common long-term complication, presenting with a characteristic barking cough and respiratory distress, often exacerbated by crying or feeding.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common type is Gross Type C (EA with distal TEF) - 85%.
- Clinical triad: Excessive salivation/drooling, choking/coughing with feeds, respiratory distress.
- Diagnosis: Inability to pass NG tube into stomach; confirmed by X-ray (coiled tube in esophageal pouch).
- VACTERL association is common (Vertebral, Anal, Cardiac, Tracheo-Esophageal, Renal, Limb defects).
- Management: Surgical repair (ligation of TEF, primary esophageal anastomosis).
- Commonest post-op complication: Anastomotic leak (early); esophageal stricture (late).
- Antenatal polyhydramnios is a significant clue due to impaired fetal swallowing of amniotic fluid.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

