Pediatric Surgery Basics

On this page
🏥 Pediatric Surgery Foundations: The Miniature Precision Universe
Pediatric surgery demands a fundamental recalibration of your clinical thinking-children are not simply small adults, but metabolically turbocharged organisms with distinct anatomical vulnerabilities and disease patterns. You'll master the physiological differences that make fluid shifts catastrophic in minutes, learn to distinguish surgical emergencies from mimics through pattern recognition, and build decision algorithms that account for age-specific pathology from pyloric stenosis to intussusception. This lesson transforms you into a clinical detective who integrates rapid assessment, evidence-based diagnostics, and multidisciplinary coordination to deliver precision care when every minute and milliliter counts.
📌 Remember: SMALL - Size matters, Metabolism differs, Anatomy varies, Limited reserves, Large surface area ratio
Age-Based Surgical Categories
- Neonatal Surgery (0-28 days)
- Critical period: 85% of congenital anomalies requiring immediate intervention
- Physiological instability: Temperature regulation, fluid balance, respiratory function
- Surface area to volume ratio: 3x higher than adults
- Heat loss rate: 4x faster than adults
- Fluid turnover: 15% of body weight daily vs 2% in adults
- Infant Surgery (1 month - 2 years)
- Rapid growth phase: 200% weight increase in first year
- Developing immunity: 50% adult immunoglobulin levels at 6 months
- Infection risk: 3x higher than older children
- Wound healing: 2x faster than adults
- Pediatric Surgery (2-18 years)
- Organ maturation: Liver function reaches adult levels by age 3
- Psychological considerations: 40% develop procedure-related anxiety
| Age Group | Weight Range | Fluid Requirement | Caloric Needs | Anesthesia Risk |
|---|---|---|---|---|
| Neonate | 0.5-4 kg | 150-200 mL/kg/day | 120 kcal/kg/day | ASA 3-4 |
| Infant | 4-12 kg | 100-150 mL/kg/day | 100 kcal/kg/day | ASA 2-3 |
| Toddler | 12-20 kg | 75-100 mL/kg/day | 80 kcal/kg/day | ASA 1-2 |
| Child | 20-40 kg | 50-75 mL/kg/day | 60 kcal/kg/day | ASA 1-2 |
| Adolescent | 40-70 kg | 35-50 mL/kg/day | 40 kcal/kg/day | ASA 1-2 |
💡 Master This: Every pediatric surgical decision must account for ongoing growth and development - what works today must accommodate the child's needs for the next 15-20 years of life
Understanding these foundational scaling principles prepares you to master the unique physiological challenges that define pediatric surgical practice.
🏥 Pediatric Surgery Foundations: The Miniature Precision Universe
⚡ Physiological Powerhouse: The Metabolic Speed Machine
Cardiovascular Adaptations
- Heart Rate Variability
- Neonates: 120-160 bpm baseline, up to 220 bpm with stress
- Infants: 100-140 bpm baseline, limited stroke volume compensation
- Cardiac output depends 80% on heart rate vs 50% in adults
- Blood volume: 80 mL/kg vs 70 mL/kg in adults
- Circulating volume loss: 10% = shock, 20% = cardiovascular collapse
- Vascular Physiology
- Systemic vascular resistance: 50% lower than adults
- Blood pressure: Systolic = 80 + (2 × age in years)
- Hypotension threshold: <70 + (2 × age) mmHg
- Capillary refill: >3 seconds indicates 15% volume loss
📌 Remember: HEART - High rate dependent, Early decompensation, Age-specific normals, Rapid volume loss, Tachycardia first sign
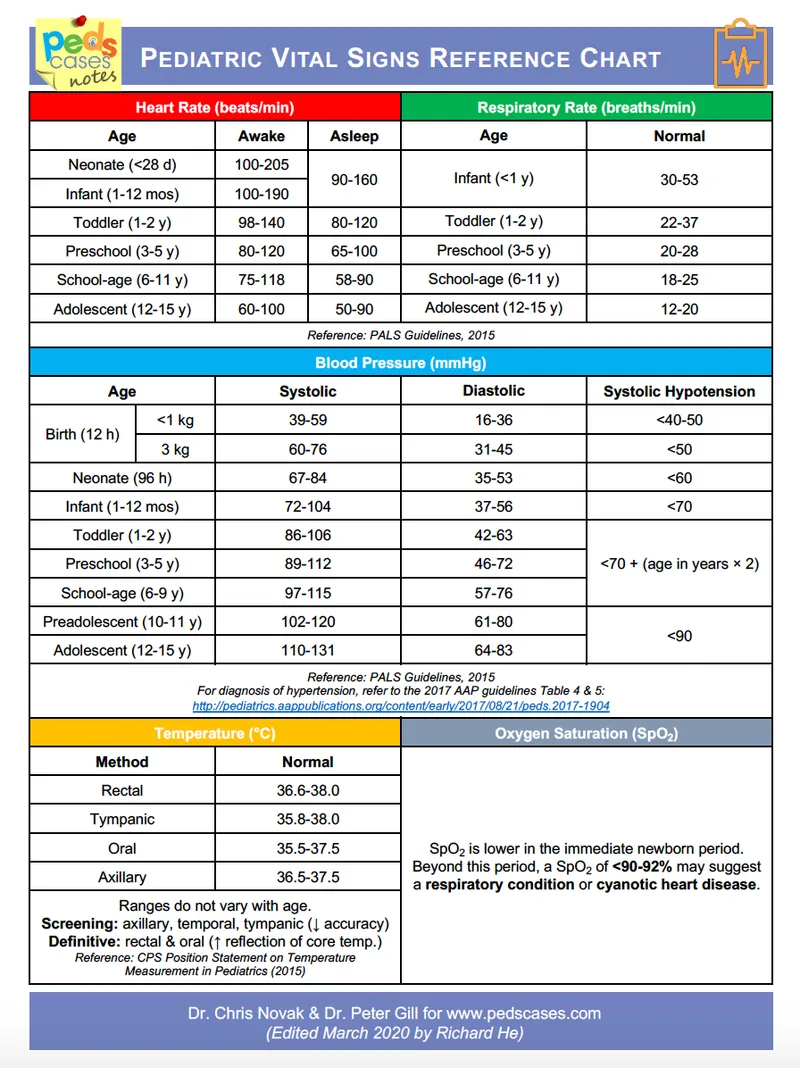
Respiratory Mechanics
- Anatomical Differences
- Larynx position: C3-C4 vs C6 in adults
- Tracheal diameter: 4mm in neonates vs 15mm in adults
- Resistance increases by 16x with 1mm of edema
- Functional residual capacity: 30 mL/kg vs 35 mL/kg in adults
- Oxygen consumption: 6-8 mL/kg/min vs 3-4 mL/kg/min in adults
- Ventilatory Patterns
- Respiratory rate: 30-60/min in neonates, 12-20/min in adolescents
- Tidal volume: 6-8 mL/kg across all ages
- Minute ventilation: 150-200 mL/kg/min vs 100 mL/kg/min in adults
- Apnea threshold: >20 seconds or with bradycardia/cyanosis
| Age Group | RR (breaths/min) | TV (mL/kg) | FRC (mL/kg) | O2 Consumption |
|---|---|---|---|---|
| Neonate | 40-60 | 6-8 | 25-30 | 6-8 mL/kg/min |
| Infant | 30-40 | 6-8 | 30-35 | 5-7 mL/kg/min |
| Toddler | 25-35 | 6-8 | 30-35 | 4-6 mL/kg/min |
| Child | 20-30 | 6-8 | 30-35 | 4-5 mL/kg/min |
| Adolescent | 15-25 | 6-8 | 30-35 | 3-4 mL/kg/min |

💡 Master This: Pediatric physiology operates with minimal reserve margins - early recognition and aggressive intervention prevent the rapid spiral from compensation to decompensation that characterizes pediatric emergencies.
These physiological principles form the foundation for understanding why pediatric surgical patients require specialized monitoring and intervention strategies.
⚡ Physiological Powerhouse: The Metabolic Speed Machine
🎯 Pattern Recognition Arsenal: The Clinical Detective Framework
Emergency Recognition Patterns
- "Can't Eat" Patterns
- Bilious vomiting in neonate = malrotation until proven otherwise
- Non-bilious vomiting + olive mass = pyloric stenosis
- Projectile vomiting: 85% sensitivity for pyloric stenosis
- Palpable olive: 60-80% of cases, 100% specific
- Ultrasound criteria: Muscle thickness >3mm, length >15mm
- "Can't Breathe" Patterns
- Respiratory distress + scaphoid abdomen = CDH
- Stridor + feeding difficulty = vascular ring/sling
- CDH incidence: 1 in 2,500 births
- Mortality rate: 20-30% overall, 50% if diagnosed postnatally
- Associated anomalies: 40% of CDH cases
📌 Remember: VOMIT - Vascular (malrotation), Obstruction (atresia), Mass (tumor), Infection (NEC), Toxic (metabolic)
Age-Specific Presentation Matrices
- Neonatal Period (0-28 days)
- Feeding intolerance: 90% of GI surgical conditions
- Respiratory distress: 75% of thoracic surgical conditions
- Immediate surgery required: CDH, EA/TEF, gastroschisis
- Urgent surgery (24-48h): Malrotation, duodenal atresia
- Elective timing: Inguinal hernia, hydrocele
- Infant Period (1-12 months)
- Intussusception peak: 6-18 months, male predominance 3:1
- Pyloric stenosis peak: 3-6 weeks, firstborn males 4:1
- Intussusception triad: Pain, mass, bloody stool (only 20% complete)
- Pyloric stenosis labs: Hypochloremic, hypokalemic alkalosis
| Condition | Peak Age | Male:Female | Key Sign | Diagnostic Test |
|---|---|---|---|---|
| Pyloric Stenosis | 3-6 weeks | 4:1 | Olive mass | Ultrasound |
| Intussusception | 6-18 months | 3:1 | Currant jelly stool | Ultrasound |
| Appendicitis | 10-15 years | 1.5:1 | McBurney tenderness | CT/Clinical |
| Malrotation | <1 year | 1:1 | Bilious vomiting | Upper GI series |
| CDH | Birth | 1:1 | Scaphoid abdomen | Chest X-ray |

💡 Master This: Pediatric surgical emergencies follow age-predictable patterns - mastering these temporal relationships enables rapid diagnosis and appropriate triage in time-sensitive conditions.
These recognition frameworks provide the foundation for systematic evaluation of pediatric surgical conditions across age groups.
🎯 Pattern Recognition Arsenal: The Clinical Detective Framework
🔬 Diagnostic Discrimination Matrix: The Evidence-Based Separator
Abdominal Pain Discrimination Framework
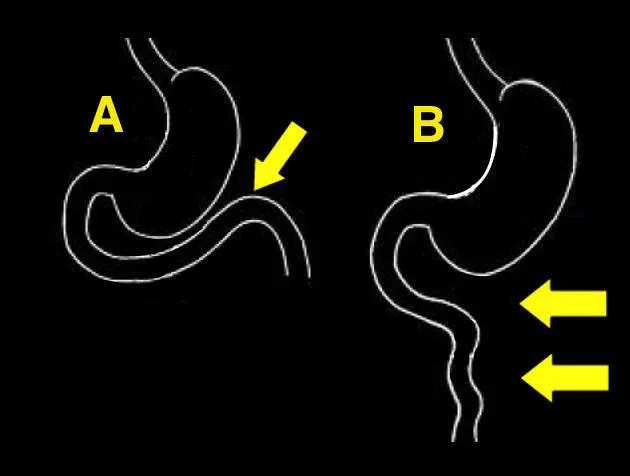
- Bilious Vomiting Differentials
- Malrotation with volvulus: Acute onset, severe pain, hemodynamic instability
- Duodenal atresia: Polyhydramnios in utero, double bubble on imaging
- Malrotation incidence: 1 in 500 births
- Volvulus risk: 75% occur in first year of life
- Mortality without surgery: 100% if complete volvulus
- Jejunoileal atresia: Multiple air-fluid levels, microcolon on contrast
- Type IIIA (apple peel): 10% of jejunal atresias
- Associated anomalies: 15% overall, 50% in apple peel type
📌 Remember: TWIST - Timing (acute vs chronic), Weight loss, Imaging findings, Stool pattern, Temperature
Respiratory Distress Discrimination
- Neonatal Respiratory Distress with Surgical Causes
- CDH: Scaphoid abdomen, heart sounds shifted, bowel sounds in chest
- EA/TEF: Excessive secretions, choking with feeds, pneumonia
- CDH mortality factors: Liver herniation (60% mortality), early presentation (40% mortality)
- EA/TEF types: Type C (85% of cases), distal TEF most common
- Associated anomalies: VACTERL in 50% of EA/TEF cases
| Condition | Chest X-ray | Abdomen | Associated Features | Mortality |
|---|---|---|---|---|
| CDH | Bowel in chest | Scaphoid | Heart shift | 20-30% |
| EA/TEF | Pneumonia | Gasless (A,B) | VACTERL | 5-10% |
| CCAM | Cystic lesions | Normal | Hydrops | 5-15% |
| Pneumothorax | Collapsed lung | Normal | Prematurity | <5% |
| RDS | Ground glass | Normal | Surfactant deficiency | 5-10% |
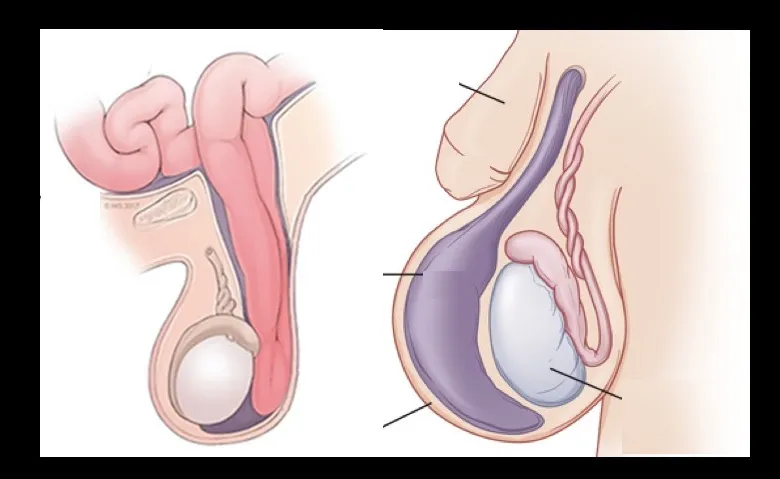
Inguinal Region Mass Discrimination
- Inguinal Hernia vs Hydrocele vs Lymphadenopathy
- Inguinal hernia: Reducible, increases with crying, silk glove sign
- Hydrocele: Transilluminates, non-reducible, fluctuant
- Hernia incidence: 1-3% of children, 30% in premature infants
- Incarceration risk: 15% in first year, 5% after age 1
- Bilateral occurrence: 10% in term infants, 50% in premature
| Feature | Inguinal Hernia | Hydrocele | Lymphadenopathy |
|---|---|---|---|
| Reducibility | Yes | No | No |
| Transillumination | No | Yes | No |
| Size variation | Yes | No | Variable |
| Age presentation | Any age | Birth-2 years | >2 years |
| Associated symptoms | Incarceration risk | None | Systemic illness |
These discrimination frameworks enable precise diagnosis in challenging pediatric surgical presentations.
🔬 Diagnostic Discrimination Matrix: The Evidence-Based Separator
⚙️ Treatment Algorithm Mastery: The Surgical Decision Engine
Surgical Timing Algorithms
- Emergency Surgery (0-6 hours)
- Malrotation with volvulus: Immediate Ladd procedure
- Gastroschisis: Immediate closure or silo placement
- Volvulus mortality: 5% if surgery within 6 hours, 25% if delayed
- Gastroschisis closure: Primary closure in 70%, staged closure in 30%
- Silo reduction: 1-2 cm daily until complete reduction
- Urgent Surgery (6-24 hours)
- Intussusception: Reduction attempt, then surgical reduction
- Incarcerated hernia: Manual reduction, then urgent repair
- Pneumatic reduction success: 85-95% in <24 hours presentation
- Surgical reduction: Required in 15% of cases
- Recurrence rate: 5-10% after non-operative reduction
📌 Remember: URGENT - Unstable vitals, Reduction failed, Gangrenous bowel, Emergent presentation, Necrosis present, Time critical
Age-Specific Surgical Approaches
- Neonatal Considerations (0-28 days)
- Minimally invasive techniques: Limited due to size constraints
- Open procedures: Preferred for complex reconstructions
- Laparoscopic feasibility: >3 kg body weight generally required
- Port size limitations: 3mm ports maximum in <5 kg infants
- CO2 insufflation: 8-12 mmHg vs 15 mmHg in adults
- Infant Adaptations (1-12 months)
- Laparoscopic appendectomy: Feasible after 6 months
- Thoracoscopic procedures: Preferred for lung lesions
- Conversion rate: 15% in <1 year, 5% in >1 year
- Operative time: 20-30% longer than open procedures
| Procedure | Age Threshold | Approach | Success Rate | Complication Rate |
|---|---|---|---|---|
| Laparoscopic Appendectomy | >6 months | MIS | 95% | 5% |
| Thoracoscopic Lobectomy | >3 months | MIS | 90% | 10% |
| Laparoscopic Fundoplication | >1 year | MIS | 85% | 15% |
| Open CDH Repair | Any age | Open | 80% | 20% |
| Laparoscopic Hernia Repair | >2 years | MIS | 95% | 3% |
- Pain Management Strategies
- Multimodal analgesia: Acetaminophen + ibuprofen + regional blocks
- Opioid-sparing techniques: Reduce by 50-70% with regional anesthesia
- Acetaminophen dosing: 15 mg/kg every 6 hours (max 75 mg/kg/day)
- Ibuprofen dosing: 10 mg/kg every 6 hours (>6 months age)
- Regional block duration: 8-12 hours for major procedures
- Nutritional Support
- Early feeding: Within 6 hours for minor procedures
- TPN initiation: After 5-7 days if enteral feeding not possible
- Caloric requirements: 120 kcal/kg/day in neonates
- Protein needs: 2.5-3 g/kg/day for growth
- Feeding advancement: 20 mL/kg/day increase if tolerated
⭐ Clinical Pearl: Enhanced Recovery After Surgery (ERAS) protocols in pediatrics reduce length of stay by 25-30% and complications by 15-20% when properly implemented
💡 Master This: Pediatric surgical algorithms must balance immediate safety with long-term growth and development - optimal timing and technique selection determine both short-term success and lifelong outcomes.
These algorithmic approaches ensure systematic, evidence-based surgical decision-making across the pediatric age spectrum.
⚙️ Treatment Algorithm Mastery: The Surgical Decision Engine
🌐 Systems Integration Hub: The Multidisciplinary Command Center
Multidisciplinary Team Architecture
- Core Surgical Team
- Pediatric surgeon: Primary decision-maker and technical expert
- Pediatric anesthesiologist: Physiological management and pain control
- Anesthesia complications: 3x higher in <1 year age group
- Airway management: Specialized equipment for <10 kg patients
- Fluid management: Strict monitoring due to limited reserves
- Specialized Support Services
- Neonatology: Critical for <37 weeks gestational age patients
- Pediatric radiology: Radiation dose optimization and specialized protocols
- CT radiation exposure: 50-75% reduction with pediatric protocols
- MRI sedation: Required in 80% of <6 years patients
- Ultrasound first: Preferred imaging for abdominal conditions
📌 Remember: TEAMS - Timing coordination, Expertise integration, Age-specific protocols, Monitoring systems, Specialized equipment
Quality Improvement Integration
- Outcome Measurement Systems
- Surgical Site Infection (SSI): Target <2% for clean procedures
- Length of Stay (LOS): Benchmarked against national databases
- NSQIP-Pediatric: Risk-adjusted outcome comparisons
- Morbidity tracking: 30-day and 1-year follow-up protocols
- Readmission rates: Target <5% for elective procedures
- Safety Protocol Implementation
- Time-out procedures: Universal for all surgical cases
- Medication reconciliation: Critical due to weight-based dosing
- Dosing errors: 10x more common in pediatric patients
- Double-check protocols: Required for all calculations
- Smart pump technology: Reduces errors by 50-70%
Technology Integration Advances
- Minimally Invasive Surgery (MIS) Evolution
- Single-port laparoscopy: Reduced scarring and improved cosmesis
- Robotic surgery: Enhanced precision for complex reconstructions
- Learning curve: 20-30 cases for proficiency
- Operative time: Initially 25% longer, equivalent after experience
- Complication rates: Similar to conventional laparoscopy
- Image-Guided Surgery
- Intraoperative ultrasound: Real-time tissue identification
- Fluorescence imaging: Perfusion assessment and anatomy delineation
- ICG fluorescence: Bowel viability assessment in 90% accuracy
- Intraoperative navigation: Reduces operative time by 15-20%
| Technology | Age Limitation | Learning Curve | Outcome Benefit | Cost Factor |
|---|---|---|---|---|
| Laparoscopy | >3 kg | 15-20 cases | Reduced LOS | 1.2x |
| Robotics | >10 kg | 25-30 cases | Enhanced precision | 2.5x |
| Fluorescence | Any age | 5-10 cases | Improved visualization | 1.5x |
| Navigation | >5 kg | 10-15 cases | Reduced complications | 1.8x |
| Single-port | >15 kg | 20-25 cases | Improved cosmesis | 1.3x |
💡 Master This: Successful pediatric surgery depends on seamless integration of specialized expertise, age-appropriate technology, and family-centered care - no single discipline can optimize outcomes independently.
These integration principles ensure comprehensive, coordinated care that addresses the unique needs of pediatric surgical patients.
🌐 Systems Integration Hub: The Multidisciplinary Command Center
🎯 Clinical Mastery Toolkit: The Rapid Reference Arsenal
Essential Clinical Thresholds
- Age-Based Vital Sign Ranges
- Heart Rate: Neonate 120-160, Infant 100-140, Child 80-120, Adolescent 60-100
- Blood Pressure: Systolic = 80 + (2 × age in years), Diastolic = 2/3 systolic
- Shock threshold: <70 + (2 × age) mmHg systolic
- Severe shock: <50 + (2 × age) mmHg systolic
- Fluid resuscitation: 20 mL/kg boluses, maximum 60 mL/kg
- Laboratory Critical Values
- Hemoglobin: Neonate >13 g/dL, Infant >10 g/dL, Child >11 g/dL
- Glucose: Neonate >45 mg/dL, Infant >60 mg/dL, Child >70 mg/dL
- Hypoglycemia risk: Higher in <2 years due to limited glycogen stores
- Fluid requirements: Maintenance = 100 mL/kg first 10 kg + 50 mL/kg next 10 kg + 20 mL/kg remaining weight
📌 Remember: VITAL - Variable by age, Immediate assessment, Trend monitoring, Action thresholds, Limit normal ranges
Emergency Decision Algorithms
- Surgical Emergency Triage
- Immediate (0-1 hour): Malrotation with volvulus, gastroschisis, CDH
- Urgent (1-6 hours): Intussusception, incarcerated hernia, appendicitis with perforation
- Malrotation mortality: <5% if <6 hours, >25% if >24 hours
- Intussusception reduction: >90% success if <24 hours presentation
- Appendicitis perforation: 15% in <5 years, 5% in >10 years
| Condition | Time Window | Success Rate | Mortality Risk | Key Decision Point |
|---|---|---|---|---|
| Malrotation | <6 hours | 95% | <5% | Bilious vomiting |
| Intussusception | <24 hours | 90% | <1% | Pneumatic reduction |
| Gastroschisis | <2 hours | 85% | 5-10% | Primary vs staged |
| CDH | <6 hours | 70% | 20-30% | Stabilization first |
| Appendicitis | <12 hours | 95% | <2% | Perforation risk |
- ABCDE Pediatric Modification
- Airway: Size = (age + 16)/4 for ETT, uncuffed <8 years
- Breathing: Rate 30-60 neonate, 12-20 adolescent
- Chest rise: Adequate if bilateral and symmetric
- Oxygen saturation: >95% target, >92% acceptable
- Work of breathing: Retractions, nasal flaring, grunting
- Circulation Assessment
- Pulse quality: Central vs peripheral comparison
- Capillary refill: <2 seconds normal, >3 seconds concerning
- Blood pressure: Last parameter to change in pediatric shock
- Urine output: >1 mL/kg/hour adequate perfusion
- Mental status: Early indicator of cerebral perfusion
⭐ Clinical Pearl: "The Pediatric Triangle" - Appearance (mental status), Work of breathing, Circulation (skin color/perfusion) provides rapid assessment in <30 seconds
💡 Master This: Pediatric surgical emergencies require immediate pattern recognition and systematic response - memorizing these frameworks enables life-saving decisions in critical moments when every second counts.
These rapid reference tools provide the essential knowledge base for confident pediatric surgical practice and emergency management.
🎯 Clinical Mastery Toolkit: The Rapid Reference Arsenal
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























