Definitions & Classifications - Defining the Deficit
- Malnutrition: Nutritional imbalance (deficiency/excess) impacting growth, body function, or clinical outcome.
- Failure to Thrive (FTT): Suboptimal weight gain/growth in children.
- Weight < 3rd-5th percentile.
- Weight crosses 2+ major percentiles downwards.
- Weight-for-Length (WFL) < 5th percentile.
- Key Anthropometric Indices (Z-scores):
- Weight-for-Age (WFA): Underweight (acute & chronic).
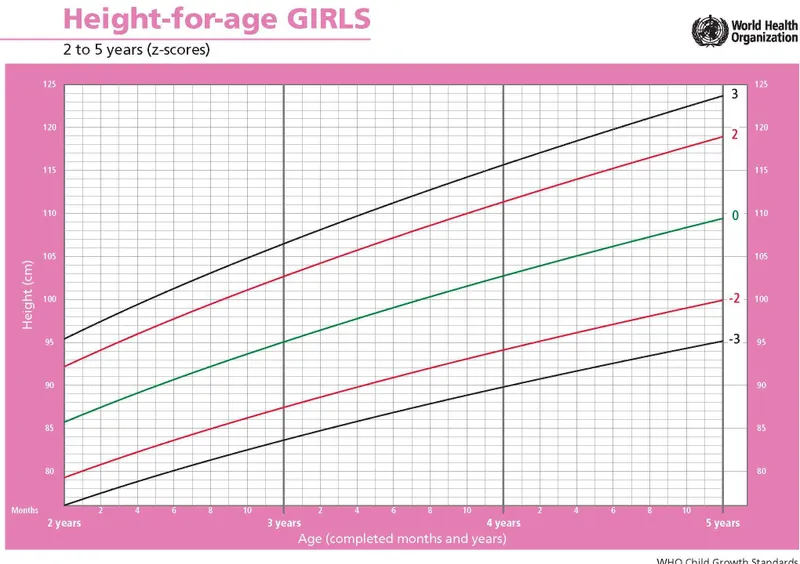
- Height-for-Age (HFA): Stunting (chronic).
- Weight-for-Height/Length (WFH/L): Wasting (acute).
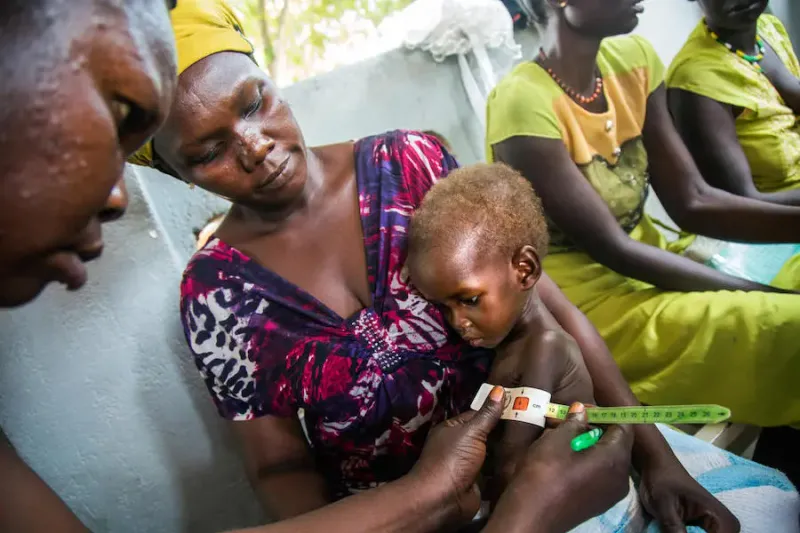
- Mid-Upper Arm Circumference (MUAC): Acute malnutrition; predictor of mortality.
- Classification by Severity (WHO, 6-59 months for MUAC):
- Moderate Acute Malnutrition (MAM): WHZ -2 to -2.9 SD; MUAC 11.5-12.4 cm.
- Severe Acute Malnutrition (SAM): Defined by criteria below.
⭐ WHO criteria for SAM: WHZ < -3 SD, MUAC < 11.5 cm (6-59 months), OR bilateral pitting edema.
Etiology & Clinical Picture - Roots & Red Flags
- Etiology:
- Inadequate Intake: Poverty, poor feeding, anorexia, oral motor issues.
- Impaired Absorption/Utilization: Malabsorption (celiac, CF), chronic diarrhea, IEMs.
- Increased Needs: Chronic infections (TB, HIV), CHD, malignancy.
- Clinical Red Flags (FTT/Malnutrition):
- Weight < 3rd percentile or ↓ 2 major centiles.
- Weight for height < -2 SD (wasting); Height for age < -2 SD (stunting).
- MUAC < 11.5 cm (SAM).
- Types & Features:
- Marasmus: Severe wasting, "old man" face, irritable, no edema.
- Kwashiorkor: Edema, moon facies, apathy, skin (flaky paint), hair (flag sign). 📌 FLAME: Fatty Liver, Anemia/Apathy, Malabsorption/Moon facies, Edema/Electrolyte imbalance.
- Marasmic-Kwashiorkor: Mixed.
⭐ Flag sign (alternating bands of light and dark hair) is characteristic of Kwashiorkor due to fluctuating protein intake.
Assessment & Management - Measure & Mend
- Assessment:
- Anthropometry:
- SAM: WFH/L < -3SD; MUAC < 11.5 cm (6-59m); Bilateral pitting edema.
- MAM: WFH/L -3SD to < -2SD; MUAC 11.5 to < 12.5 cm.
- Clinical: Dehydration (Appetite test), infection signs, micronutrient deficiencies.
- FTT: Detailed history (dietary, medical, social), feeding observation.
- Anthropometry:
- Management (WHO 10 Steps for SAM):
- Stabilization Phase (Days 1-7):
- 1-5: Treat/Prevent Hypoglycemia, Hypothermia, Dehydration (ReSoMal), Electrolyte imbalance, Infections.
- 6: Cautious Feeding: F-75 (~75 kcal/100ml). NO iron initially.
- Rehabilitation Phase (Weeks 2-6):
- 7: Catch-up Growth: F-100 (~100 kcal/100ml) or RUTF.
- 8: Micronutrients (Start iron).
- 9: Sensory stimulation & emotional support.
- 10: Prepare for discharge & follow-up.
- Stabilization Phase (Days 1-7):
⭐ In SAM management, oral rehydration with ReSoMal is preferred over standard WHO ORS due to lower sodium (~45 mmol/L) and higher potassium (~40 mmol/L) content.
Complications & Prevention - Dodge & Defend
- Complications:
- Infections: Pneumonia, sepsis, gastroenteritis (↓ immunity).
- Electrolyte imbalance: Hypokalemia, hypophosphatemia, hypomagnesemia.
- Hypothermia, hypoglycemia.
- Severe anemia (Fe, B12, folate def.).
- Impaired organ function (cardiac, renal).
- Long-term neurodevelopmental delay.
- ⭐ > Refeeding syndrome in severely malnourished children is characterized by severe hypophosphatemia (key electrolyte), hypokalemia, and hypomagnesemia, typically occurring 3-5 days after starting refeeding.
- Prevention:
- Maternal nutrition & ANC.
- Exclusive breastfeeding (first 6 months); continued with complementary feeds.
- Complementary feeding: Timely, Adequate, Safe, Appropriate (TASA) from 6 months.
- Regular growth monitoring (Wt, Ht, MUAC).
- Full immunization.
- Micronutrient supplementation: Vit A, Iron-Folic Acid (IFA), Zinc.
- Hygiene & sanitation (WASH).
- Govt. programs: ICDS, POSHAN Abhiyaan.
High‑Yield Points - ⚡ Biggest Takeaways
- Failure to Thrive (FTT): weight < 3rd-5th percentile or crossing two major centiles down.
- Marasmus: severe wasting (Wt/Ht < -3 SD), alert but irritable, no edema.
- Kwashiorkor: edema is key, with dermatosis (flaky paint), hair changes, apathy.
- MUAC < 11.5 cm indicates Severe Acute Malnutrition (SAM) in children 6-59 months.
- Refeeding syndrome risk: monitor electrolytes (K, PO4, Mg) during initial therapy.
- SAM: stabilize with F-75 (low protein, low osmolarity), then F-100 for catch-up growth.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

