Pesticide Exposure - Chemical Culprits
- Organophosphates (OPs):
- E.g., Malathion, Parathion, Chlorpyrifos.
- Irreversible acetylcholinesterase (AChE) inhibition.
- Carbamates:
- E.g., Carbaryl, Propoxur, Aldicarb.
- Reversible AChE inhibition.
- Organochlorines (OCs):
- E.g., DDT, Endosulfan, Lindane.
- Neurotoxic: Na+/K+ channel interference, GABA antagonism. Persistent.
- Pyrethroids:
- E.g., Permethrin, Cypermethrin.
- Sodium channel modulators. Relatively low human toxicity.
⭐ Organophosphate compounds (e.g., Phorate - "Thimet", "Sulphas") are a leading cause of fatal poisoning in agricultural communities.
Pesticide Exposure - Tiny Targets
- Children uniquely vulnerable: ↑ exposure, ↓ detoxification.
- Routes: Ingestion (hand-to-mouth, diet), inhalation, dermal.
- Why vulnerable?
- ↑ Surface area to mass ratio.
- Immature metabolic pathways (liver).
- Developing nervous system.
- Higher intake per kg body weight.
- Behaviors: crawling, mouthing objects.

⭐ Chronic low-level pesticide exposure in children is linked to neurodevelopmental issues, ADHD, and lower IQ.
Pesticide Exposure - Body's Battle
- Organophosphates (OPs) & Carbamates:
- Mechanism: AChE inhibition → ↑ACh.
- Cholinergic Crisis:
- Muscarinic: 📌 DUMBELS (Diarrhea, Urination, Miosis, Bronchorrhea/Bronchospasm, Emesis, Lacrimation, Salivation).
- Nicotinic: Fasciculations, weakness, paralysis, HTN, tachycardia.
- CNS: Seizures, coma.
- Organochlorines (e.g., DDT):
- Mechanism: CNS stimulant (Na+/K+ ATPase, GABA).
- Effects: Tremors, seizures, paresthesias.
- Pyrethroids (e.g., Permethrin):
- Mechanism: Na+ channel modulation.
- Effects: Paresthesias (skin), dizziness.
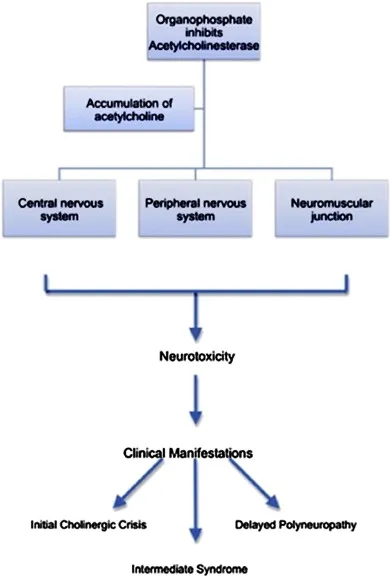
⭐ In OP poisoning, Pralidoxime (PAM) reactivates AChE (muscarinic & nicotinic effects), unlike atropine (muscarinic only). Give within 24-48 hrs.
Pesticide Exposure - Silent Sabotage
- Children: ↑ vulnerability (↑intake/kg, immature detox).
- Sources: Food, water, household, parental occupation.
- Types: Organophosphates (OPs), Carbamates, Organochlorines, Pyrethroids.
- Acute OP/Carbamate:
- Cholinergic crisis: 📌 DUMBELS (Diarrhea, Urination, Miosis, Bradycardia/Bronchospasm, Emesis, Lacrimation, Salivation).
- Dx: ↓Cholinesterase.
- Rx: Atropine, Pralidoxime (OPs).
- Chronic: Neurodevelopmental (ADHD, ↓IQ), endocrine, cancer.
- Prevention: Wash food, safe storage, IPM.
⭐ OPs & Carbamates cause cholinergic crisis by inhibiting acetylcholinesterase. Pralidoxime (PAM) is used for OP poisoning (not Carbamates) to reactivate enzyme, ideally within 24-48 hrs.
Pesticide Exposure - Spot & Stop
-
Spotting (Toxidromes):
- Organophosphates (OP) & Carbamates: Cholinergic crisis (📌 DUMBELS: Diarrhea, Urination, Miosis, Bronchospasm/Bradycardia, Emesis, Lacrimation, Salivation). Key: ↓RBC Acetylcholinesterase.
- Organochlorines (OC): CNS hyperexcitability, tremors, seizures.
- Pyrethroids: Allergic reactions (skin, respiratory), paresthesias (e.g., facial).
- Paraquat: Caustic oral/GI injury → progressive pulmonary fibrosis, renal & hepatic failure.
-
Stopping Priorities:
- ABCs: (Airway, Breathing, Circulation).
- Decontamination: Remove clothes, wash skin (soap & water). Gastric lavage (<1-2h), charcoal.
- Antidotes:
- OP: Atropine (muscarinic) + Pralidoxime (PAM, AChE reactivator, 24-48h).
- Carbamates: Atropine. (PAM generally not indicated).
- OC: Diazepam for seizures.
- Paraquat: Supportive; antioxidants (NAC), early hemoperfusion.
-
Prevention: Safe handling/storage, Personal Protective Equipment (PPE).
⭐ In Organophosphate poisoning, "aging" refers to the irreversible binding of the phosphate to cholinesterase; Pralidoxime must be given before this occurs, typically within 24-48 hours, to be effective.
High‑Yield Points - ⚡ Biggest Takeaways
- Organophosphates (OPs) & carbamates inhibit acetylcholinesterase (AChE), causing cholinergic crisis (DUMBELS/SLUDGE).
- Key features: Miosis, bradycardia, muscle fasciculations/weakness, seizures.
- Children are highly vulnerable due to greater exposure and immature detoxification.
- Treatment: Decontamination, atropine (muscarinic antagonist), pralidoxime (PAM) for OPs (crucial early).
- Chronic exposure is linked to neurodevelopmental problems (e.g., ADHD).
- Pyrethroids cause paresthesias, allergic reactions; manage symptomatically.
- ↓ RBC AChE levels confirm OP/carbamate poisoning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

