Mercury 101 - Element Exposed
Key forms of Mercury ($Hg$) with their sources and properties:
| Form | Symbol(s) | Key Sources | Key Properties |
|---|---|---|---|
| Elemental | $Hg^0$ | Thermometers, dental amalgams, batteries, industrial. | Volatile liquid; Inhalation main route. |
| Inorganic | $Hg^{2+}$ | Industrial, cosmetics (skin creams), some traditional medicines (e.g., Rasa Shastra). | Poor GI absorption; Skin absorption possible; Nephrotoxic. |
| Organic | $CH_3Hg^+$ (Methyl-Hg), $C_2H_5Hg^+$ (Ethyl-Hg) | Methyl-Hg: Fish (bioaccumulation). Ethyl-Hg: Thimerosal (vaccines - past concern). | Lipid soluble; Good GI absorption; Neurotoxic; Crosses BBB & placenta. |
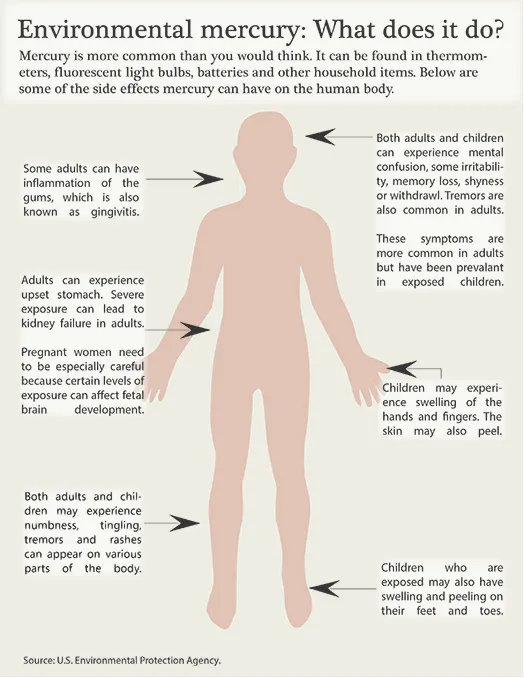
Body Invader - Toxic Trail
- Absorption:
- Elemental ($Hg^0$): Primarily via inhalation (efficient).
- Inorganic ($Hg^{2+}$) & Organic ($MeHg$): Gastrointestinal tract.
- Distribution: Systemic; readily crosses blood-brain and placental barriers.
- Targets: Brain (CNS), kidneys.
- Accumulates: Placenta, breast milk ($MeHg$).
- Metabolism:
- $Hg^0$ oxidized to $Hg^{2+}$ in blood/tissues.
- $MeHg$ slowly demethylated to inorganic $Hg^{2+}$.
- Excretion:
- Urine: Predominantly $Hg^0$ and $Hg^{2+}$.
- Feces: Mainly $MeHg$ and some $Hg^{2+}$.
- Hair: $MeHg$ (reflects chronic exposure).
Mechanism of Toxicity:
- High affinity for sulfhydryl (-SH) groups.
- Leads to enzyme inhibition & oxidative stress.
- Disrupts neurotransmission; damages microtubules.

⭐ Elemental mercury vapor is well-absorbed via inhalation (≈80%) and primarily targets the CNS and kidneys.
Poison's Portrait - Symptoms Spotlight
Manifestations depend on mercury form and exposure (acute/chronic).
-
Elemental ($Hg^0$ vapor)
- Acute: Pneumonitis.
- Chronic: Tremors, erethism ("Mad Hatter's").
-
Inorganic ($Hg^{2+}$ salts)
- Acute: Hemorrhagic gastroenteritis, renal (ATN).
- Chronic: Gingivostomatitis, nephropathy.
-
Organic ($CH_3Hg^+$ - Methylmercury)
- CNS: Paresthesias, ataxia, visual field constriction, hearing loss. Minamata disease.
- Children: Developmental delay.
-
Pediatric Hallmark: Acrodynia (Pink Disease)
- Chronic exposure (often inorganic $Hg$).
- Features: Painful, pink hands/feet, hypertension, photophobia, irritability, sweating.
- 📌 Mnemonic: PINK - Pain, Irritability/Insomnia, Neuropathy, K(C)ats (hypertension), Sweating/Skin changes.
⭐ Acrodynia, or Pink Disease, characterized by painful, swollen, pink hands and feet, is a distinctive feature of chronic mercury poisoning in young children.
Detect & Defend - Healing Hands
- Diagnosis:
- History of exposure (dietary, environmental, occupational).
- Lab tests:
- Blood mercury: Acute/recent high exposure (concern > 5-10 µg/L).
- 24-hr urine mercury: Best for inorganic/elemental mercury.
- Hair mercury: Chronic organic (esp. methylmercury) exposure.
- Neuropsychological testing: Assess cognitive, motor, behavioral effects.
- Management:
- Crucial first step: Stop further exposure.
- Supportive care: Maintain vital functions, hydration, nutrition.
- Decontamination: E.g., activated charcoal for recent significant ingestion.
- Chelation Therapy:
- Agents: Succimer (DMSA), Dimercaprol (BAL), DMPS.
- Indications: Symptomatic patients, very high mercury levels. Note side effects.
⭐ Succimer (DMSA) is the preferred oral chelating agent for pediatric mercury poisoning, particularly for inorganic and elemental forms.
- Prevention:
- Avoid high-mercury fish (shark, swordfish).
- Proper disposal of mercury-containing items (thermometers, batteries).
- Awareness campaigns. Maternal counseling on safe fish consumption.
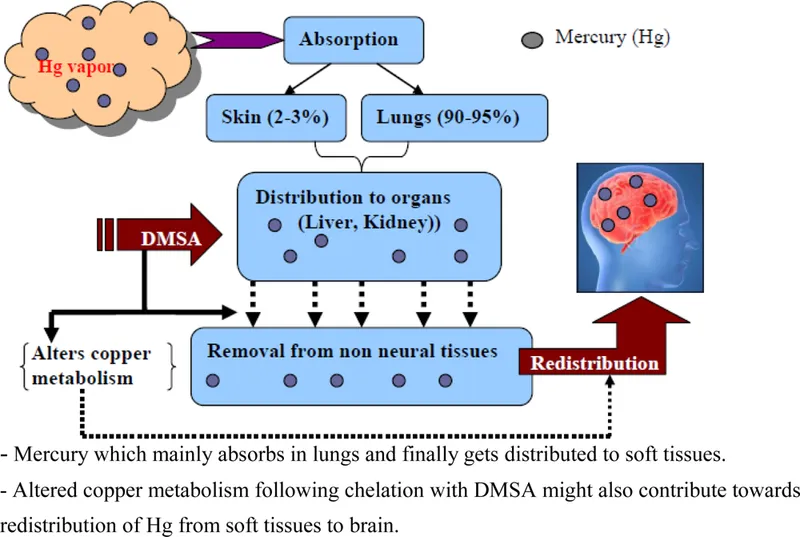 , Dimercaprol (BAL), DMPS - with indications, contraindications, and key side effects)
, Dimercaprol (BAL), DMPS - with indications, contraindications, and key side effects)
High‑Yield Points - ⚡ Biggest Takeaways
- Methylmercury from fish consumption is a potent neurotoxin, especially impacting the developing brain.
- Minamata disease (severe methylmercury poisoning) features cerebellar ataxia, dysarthria, and visual field constriction.
- Acrodynia (Pink Disease): hypersensitivity to inorganic mercury causing painful, pink extremities, rash, and photophobia/irritability.
- Diagnosis: Blood and urine mercury levels are key; hair analysis for chronic methylmercury.
- Treatment: Chelation therapy (DMSA, DMPS) and immediate removal from exposure source.
- Elemental mercury (e.g., broken thermometers) primarily causes respiratory distress and neurological symptoms if inhaled.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

