Definition & Etiology - Seizure Storm Starters
- SE Definition: Continuous seizure activity for ≥5 minutes, OR ≥2 discrete seizures without full recovery of consciousness between episodes.
- Classification:
- Convulsive (CSE) vs. Non-Convulsive (NCSE)
- Refractory SE (RSE); Super-Refractory SE (SRSE)
- Common Pediatric Etiologies (📌 FIMETT):
- Febrile SE (prolonged)
- Infections (CNS: meningitis, encephalitis)
- Metabolic (hypoglycemia, hyponatremia, hypocalcemia)
- Epilepsy (subtherapeutic AEDs, acute illness)
- Trauma (head injury)
- Toxins (e.g., isoniazid, organophosphates)
⭐ The most common identifiable cause of SE in children is prolonged febrile seizures.
Pathophysiology & Clinical Features - Brain's Electrical Riot
- Pathophysiology: Seizure termination fails (↓ GABAergic inhibition via GABA-A receptor internalization) & excitation persists (↑ NMDA receptor activity/trafficking).
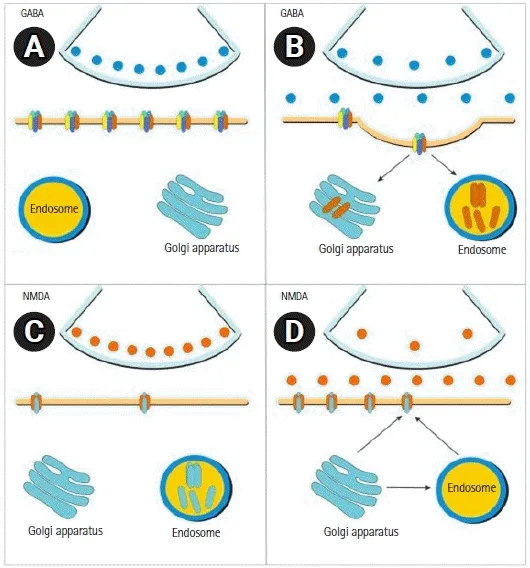
- Systemic Effects: Hyperthermia, lactic acidosis, rhabdomyolysis, hypoglycemia (early) / hyperglycemia (late), arrhythmias, BP changes.
- Clinical Features:
- CSE (Convulsive Status Epilepticus): Overt tonic-clonic, tonic, clonic, or myoclonic seizures.
- NCSE (Non-Convulsive Status Epilepticus): Subtle; altered mental status, confusion, lethargy, staring, automatisms, nystagmus. High suspicion needed; confirm with EEG.
⭐ After approximately 30 minutes of SE, GABA-A receptors decrease on the neuronal surface, making benzodiazepines less effective.
Initial Management (0-20 min) - Rapid Rescue Race
'Time is Brain'! Staged protocol.
- Stabilization (0-5 min):
- ABCs. Oxygen. IV access.
- Glucose check: if <60 mg/dL, give IV Dextrose (2-4 ml/kg D10W / 1-2 ml/kg D25W).
- Initial Therapy (5-20 min) - 1st Line BZDs:
- IV Lorazepam: 0.1 mg/kg (max 4mg), repeat once.
⭐ IV Lorazepam: preferred 1st-line; longer CNS action vs Diazepam.
- No IV: IM Midazolam 0.2 mg/kg (max 10mg).
- Others: IV Diazepam (0.15-0.2 mg/kg, max 10mg); Buccal Midazolam; Rectal Diazepam.
- IV Lorazepam: 0.1 mg/kg (max 4mg), repeat once.
- Labs: POC glucose, electrolytes, Ca, Mg, ABG, CBC, LFT, RFT, AED levels.
Second & Third Line Management - Backup Battle Plan
- Second Therapy Phase (20-40 min): If seizures persist post-2 Benzodiazepine doses.
⭐ Fosphenytoin is preferred over phenytoin for IV administration due to lower risk of local tissue injury and cardiovascular side effects.
- Third Therapy Phase (40-60 min) - Refractory SE (RSE): If seizures persist after adequate second-line agent. Requires PICU admission and continuous EEG.
- Options: Continuous Midazolam infusion, Propofol, or Pentobarbital coma. ⚠️ Phenytoin: cardiac monitoring needed. Phenobarbital: risk of respiratory depression.
RSE, SRSE & Prognosis - Stubborn Seizure Saga
- Refractory SE (RSE): Seizure persistence despite adequate initial Benzodiazepine (BZD) AND a second-line Anti-Epileptic Drug (AED).
- Super-Refractory SE (SRSE): SE lasting ≥24 hours after anesthetic therapy initiation, or recurring on anesthetic withdrawal.
- Management (RSE/SRSE): Continuous EEG monitoring. Consider: Ketamine, Lidocaine, Magnesium, Pyridoxine (infants), Immunotherapy, Ketogenic diet, Hypothermia.
- Complications: Neuronal injury, cerebral edema, epilepsy, cognitive impairment. Systemic: aspiration, respiratory failure, arrhythmias.
- Prognosis: Worse with anoxic injury/CNS infection, longer SE duration, age extremes, poor initial treatment response.
⭐ Mortality in pediatric SE can be up to 3-5%, with higher rates in RSE/SRSE and specific etiologies like anoxia or CNS infections.
High‑Yield Points - ⚡ Biggest Takeaways
- Status Epilepticus (SE): Seizure lasting > 5 minutes or recurrent seizures without full recovery between episodes.
- Prioritize ABCDE (Airway, Breathing, Circulation, Disability, Exposure); check blood glucose immediately.
- First-line therapy: IV Lorazepam is preferred; IV Diazepam or IM/buccal/intranasal Midazolam are alternatives.
- Second-line agents: IV Phenytoin/Fosphenytoin, Valproate, or Levetiracetam if seizures persist post-benzodiazepines.
- Refractory SE: Requires ICU admission, continuous EEG monitoring, and agents like Midazolam infusion or Propofol.
- Always investigate and treat the underlying cause (e.g., infection, metabolic, hypoxia, trauma).
- Key complications include hypoxia, hyperthermia, acidosis, rhabdomyolysis, and potential neuronal damage if prolonged.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

