Shock Basics - Defining the Crisis
- Definition: Critical syndrome of systemic hypoperfusion resulting in decreased oxygen delivery (DO₂) to tissues, leading to cellular hypoxia, metabolic derangements, and end-organ dysfunction.
- Pathophysiological Hallmarks:
- Imbalance between DO₂ and oxygen consumption (VO₂).
- Shift to anaerobic metabolism → ↑ Lactic acid ($pH < \textbf{7.35}$, serum lactate $> extbf{2}$ mmol/L).
- Cellular edema, lysosomal leakage, cell death.
- Inflammatory mediator release.
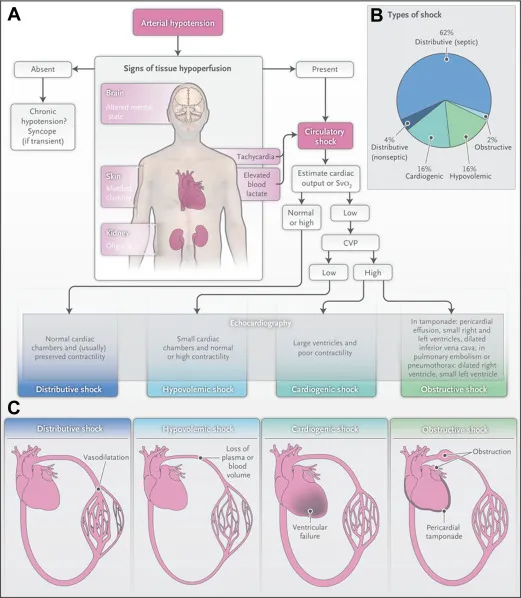
- Main Types & Core Problem:
Type Core Physiological Problem Hypovolemic ↓ Preload (critical reduction in intravascular volume) Cardiogenic ↓ Contractility (myocardial pump failure) Distributive ↓ SVR (pathological vasodilation, maldistribution) Obstructive Obstruction to cardiac filling or emptying
⭐ Most common type of shock in children is hypovolemic shock, often due to gastroenteritis.
Recognizing Shock - Spotting the Signals
- Key indicators (Think 📌 TACHY plus more):
- Tachycardia: Earliest sign.
- Altered Mental Status: Irritable, lethargic.
- Cool, clammy, pale, mottled skin.
- Hypotension: LATE sign! Don't wait.
- Prolonged CapillarY Refill Time (CRT >2s).
- Also watch for:
- Weak peripheral pulses (bounding in early warm septic shock).
- Oliguria (<1 mL/kg/hr).
- Tachypnea.
- Shock Stages:
- Compensated: BP normal (mechanisms active). Vital organs perfused. Signs: Tachycardia, cool extremities, delayed CRT.
- Decompensated (Hypotensive): BP drops (mechanisms fail). Organ damage likely. Signs: Hypotension, worsening mental status, poor central pulses.
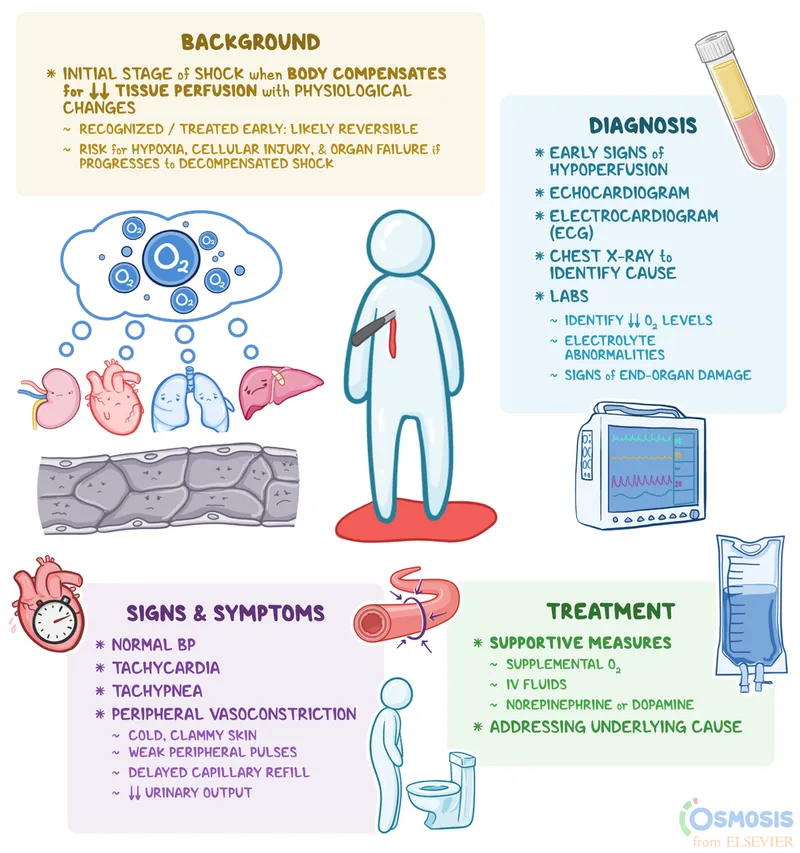
- ⭐
Hypotension is a late and ominous sign of shock in pediatric patients; rely on other perfusion indicators.
Shock Management - Rapid Rescue
- ABCDE approach: Prioritize Airway, Breathing, Circulation.
- Administer high-flow Oxygen. Secure IV/IO access (IO if IV >90s or 2 attempts).
- Fluid Resuscitation (Isotonic crystalloids NS/RL):
- Initial: 20 mL/kg bolus over 5-20 mins (faster if severe).
- Reassess; repeat up to 40-60 mL/kg if shock persists.
- Cardiogenic shock: Cautious 5-10 mL/kg over 10-20 mins.
- 📌 O-FISH: Oxygen, Fluids, Inotropes, Specific treatment, Hypoglycemia/Hypothermia correction.
- Vasopressors (Adrenaline, Noradrenaline) if fluid-refractory.
- Monitor vitals, CRT, urine output, sensorium. Correct metabolic issues.
⭐ The 'Golden Hour' in shock management emphasizes rapid IV/IO access and initiation of fluid resuscitation within the first hour of recognition.
Specific Shocks - Tailored Takedowns
- Hypovolemic: Isotonic crystalloids (20 ml/kg bolus); PRBCs for hemorrhage.
- Septic: 📌 BEAT IT: Blood cultures, Early antibiotics (within 1 hour), Access, Titrate fluids (crystalloids), Inotropes (norepinephrine/dopamine), Target MAP.
- Cardiogenic: Cautious fluids; Inotropes (dobutamine, milrinone); Diuretics; Vasodilators.
- Anaphylactic: IM Epinephrine (0.01 mg/kg 1:1000, max 0.3-0.5mg); Antihistamines; Corticosteroids; IV fluids.
- Obstructive: Treat cause: Needle decompression (tension pneumothorax); Pericardiocentesis (tamponade); PGE1 (ductal-dependent lesions).

⭐ In suspected septic shock, broad-spectrum antibiotics should be administered within 1 hour of recognition to improve outcomes significantly.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypotension is a LATE sign in pediatric shock; tachycardia and poor perfusion (e.g., capillary refill >2s, cool extremities) are early.
- Most common type: Hypovolemic shock, typically due to gastroenteritis or hemorrhage.
- Initial fluid resuscitation: 20 mL/kg isotonic crystalloid (NS or RL) bolus over 5-10 minutes; repeat as needed.
- Septic shock: Requires prompt antibiotics (within 1 hour), fluid resuscitation, and vasopressors (e.g., epinephrine for cold shock, norepinephrine for warm shock).
- Anaphylactic shock: Intramuscular (IM) epinephrine is the first-line, life-saving treatment.
- Cardiogenic shock: Characterized by pulmonary edema/hepatomegaly; administer fluids cautiously (5-10 mL/kg over 10-20 min) and use inotropes.
- Recognize compensated shock (normal BP, signs of organ dysfunction) to intervene before decompensated shock (hypotension) occurs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

