MODS: Definition & Triggers - System Shutdown Saga
- Definition: Progressive, potentially reversible dysfunction of two or more organ systems following an acute life-threatening insult, requiring intervention to maintain homeostasis.
- Key Pediatric Triggers:
- Sepsis & Septic Shock (📌 Most Common)
- Major Trauma (e.g., head injury, polytrauma)
- Extensive Burns
- Post-Cardiac Surgery (low cardiac output states)
- Oncologic Emergencies (e.g., tumor lysis syndrome, neutropenic sepsis)
- Acute Respiratory Distress Syndrome (ARDS)
- Severe Hypoperfusion States
⭐ Sepsis remains the leading cause of MODS in pediatric intensive care units (PICUs).
 oka
oka
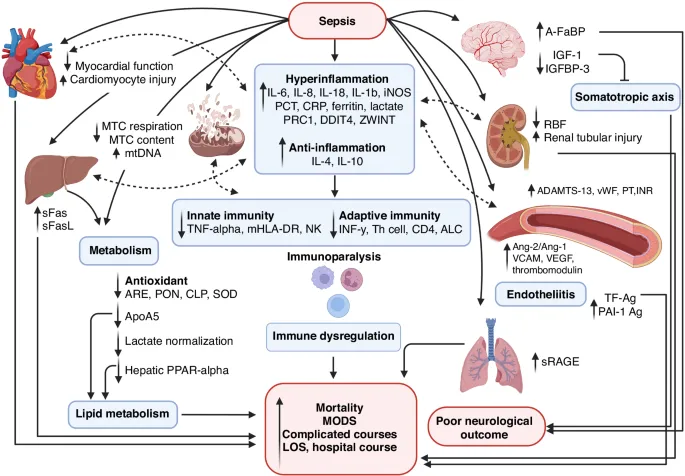
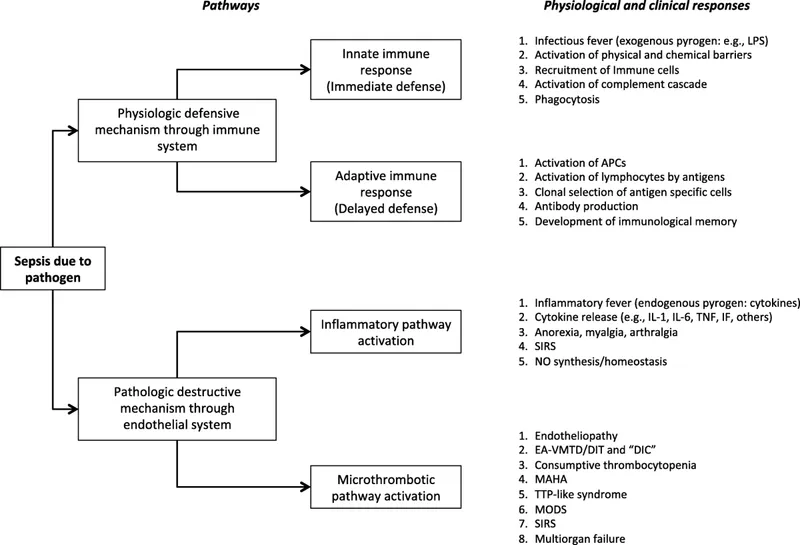
MODS: Pathophysiology - Inflammatory Mayhem
The development of MODS involves a complex, dysregulated host response:
- Uncontrolled Inflammation (SIRS/CARS): Imbalance between pro-inflammatory (SIRS) and anti-inflammatory (CARS) responses fuels systemic damage.
- Endothelial Dysfunction: Leads to ↑vascular permeability, edema, and impaired blood flow regulation.
- Microcirculatory Failure: ↓Oxygen delivery and utilization at the tissue level, despite adequate systemic hemodynamics.
- Mitochondrial Dysfunction: Cellular energy crisis; cells cannot use oxygen effectively, leading to ↓ATP.
- Coagulopathy: Systemic activation of coagulation, potentially leading to disseminated intravascular coagulation (DIC)-like states.
- Immune Paralysis (PICS): Persistent Inflammation, Immunosuppression, and Catabolism Syndrome marks a late phase of profound immunosuppression.
⭐ The "second hit" phenomenon, where a primed system overreacts to a subsequent insult, is crucial in MODS progression.
MODS: Organ Manifestations - System Failures
MODS involves the progressive, sequential failure of multiple organ systems. Key clinical manifestations include:
- Lungs (Respiratory): Pediatric Acute Respiratory Distress Syndrome (pARDS).
- Criteria: $P_aO_2/F_iO_2$ ratio ≤300.
- Markers: Hypoxemia.
- Cardiovascular (CV): Shock.
- Criteria: Hypotension, need for vasopressor support.
- Markers: ↑Lactate.
- Renal: Acute Kidney Injury (AKI).
- Criteria: pRIFLE or KDIGO criteria.
- Markers: ↑Serum creatinine, ↓Urine output.
- Hepatic: Liver dysfunction.
- Markers: ↑Bilirubin, ↑Transaminases, Coagulopathy (↑INR).
- Central Nervous System (CNS): Encephalopathy.
- Markers: Altered Glasgow Coma Scale (GCS).
- Hematologic: Coagulopathy.
- Criteria: Thrombocytopenia, Disseminated Intravascular Coagulation (DIC).
- Markers: ↓Platelets, ↑D-dimer, ↓Fibrinogen.
- Gastrointestinal (GI): Dysfunction.
- Manifestations: Ileus, gut barrier dysfunction.
- Markers: Feeding intolerance.
📌 Mnemonic: Lungs, Heart, Kidneys, Liver, Brain, Blood, Gut - "Little Hippos Kiss Lovely Baby Boys Goodnight".
⭐ Acute Respiratory Distress Syndrome (ARDS) is the most common organ dysfunction in pediatric MODS.
MODS: Scoring & Management - Rescue Protocol
- Scoring Systems: Crucial for quantifying organ dysfunction and guiding therapy.
- PELOD-2 (Pediatric Logistic Organ Dysfunction-2)
- pSOFA (pediatric Sepsis-related Organ Failure Assessment)
⭐ The PELOD-2 score is a validated tool for quantifying severity and predicting mortality in pediatric MODS.
- Management Protocol - Rescue Steps:
- 1. Source Control: Identify and eliminate the trigger.
- Prompt administration of appropriate antibiotics.
- Surgical intervention for drainage or debridement if indicated.
- 2. Organ Support: Tailored to individual organ dysfunction.
- Respiratory: Lung-protective mechanical ventilation strategies.
- Cardiovascular: Vasoactive drugs (e.g., epinephrine, norepinephrine) to maintain perfusion.
- Renal: Renal Replacement Therapy (RRT) for acute kidney injury.
- Nutrition: Early enteral nutrition to support metabolic demands.
- Hematologic: Judicious use of blood products.
- 3. Consider Advanced Therapies: For refractory cases.
- ECMO (Extracorporeal Membrane Oxygenation).
- Immunomodulation (evidence remains limited).
- 1. Source Control: Identify and eliminate the trigger.
High‑Yield Points - ⚡ Biggest Takeaways
- MODS: Progressive dysfunction of ≥2 organ systems post-insult; sepsis is a primary trigger.
- Pathogenesis: Systemic inflammation (SIRS), endothelial injury, microvascular dysfunction.
- Scoring: PELOD-2 and pSOFA assess severity and predict pediatric outcomes.
- Commonly involved: Lungs (ARDS), cardiovascular (shock), renal (AKI), hepatic systems.
- Treatment: Supportive care, addressing the root cause and organ-specific support.
- Prognosis: Mortality rises sharply with the number of dysfunctional organs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

