Histiocytosis Syndromes: Overview - Cell Chaos Crew
- Group of rare disorders: characterized by ↑ proliferation & accumulation of histiocytes (macrophages or dendritic cells).
- Classification based on cell lineage:
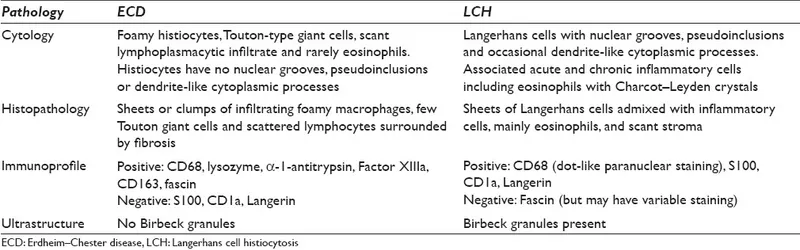
- Langerhans Cell Histiocytosis (LCH): CD1a+, S100+, Langerin (CD207)+. Most common.
- Non-Langerhans Cell Histiocytoses (Non-LCH): e.g., Juvenile Xanthogranuloma (JXG), Rosai-Dorfman disease.
- Malignant Histiocytoses.
⭐ Birbeck granules (tennis-racket appearance on Electron Microscopy) are pathognomonic for Langerhans Cell Histiocytosis (LCH).
Histiocytosis Syndromes: LCH - Bone's Bizarre Battle
- Langerhans Cell Histiocytosis (LCH): Clonal proliferation of Langerhans cells, characterized by Birbeck granules (tennis-racket appearance on Electron Microscopy).
- Immunophenotype: CD1a+, S100+, Langerin (CD207)+.
- Commonly associated with BRAF V600E mutation (~50%).
- Clinical Forms:
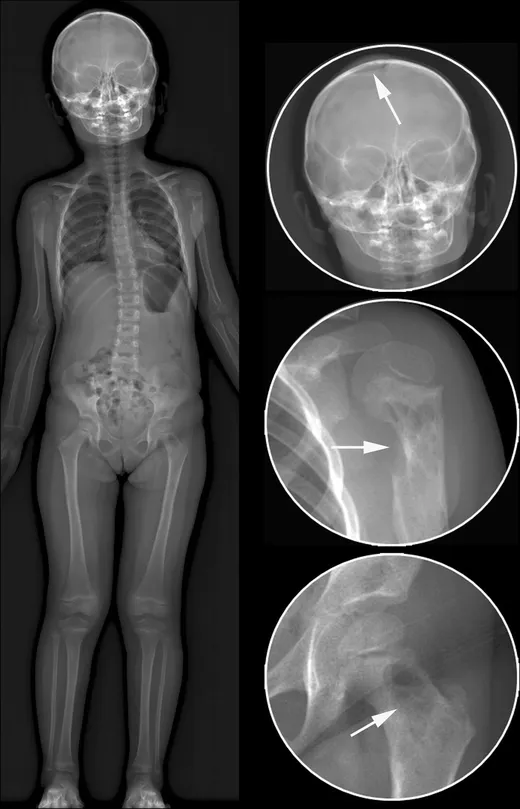
- Unifocal (Eosinophilic Granuloma): Solitary, lytic bone lesion (skull, femur); may affect skin, lung. Best prognosis.
- Multifocal Unisystem (Hand-Schüller-Christian Disease): Classic triad: lytic bone lesions (skull), diabetes insipidus, exophthalmos. (📌 HAnd: Skull lesions, DI, Exophthalmos).
- Multifocal Multisystem (Letterer-Siwe Disease): Aggressive; infants < 2 years. Features: skin rash (seborrheic-like), hepatosplenomegaly, lymphadenopathy, fever, cytopenias. Poorest prognosis.
- Treatment: Varies by extent; observation, curettage, steroids, chemotherapy (e.g., vinblastine, prednisone).
⭐ Birbeck granules, appearing as tennis-racket shaped intracytoplasmic organelles on electron microscopy, are pathognomonic for Langerhans Cell Histiocytosis (LCH).
Histiocytosis Syndromes: HLH - Cytokine Storm Troopers
HLH: Life-threatening hyperinflammation. Uncontrolled lymphocyte/macrophage activation → cytokine storm (↑IFN-γ, TNF-α). Due to impaired NK/CD8+ T cell function.
- Types:
- Primary (Familial): Genetic (e.g., PRF1, UNC13D, STX11)
- Secondary: Infections (EBV, CMV), malignancy (lymphoma), autoimmune (SLE, JIA).
- Diagnosis (HLH-2004, ≥5/8 criteria):
- Fever ≥38.5°C
- Splenomegaly
- Cytopenias (≥2 lines): Hb <9 g/dL, Platelets <100x10⁹/L, Neutrophils <1.0x10⁹/L
- Hypertriglyceridemia (fasting, ≥3 mmol/L) OR Hypofibrinogenemia (≤1.5 g/L)
- Hemophagocytosis (bone marrow/spleen/lymph nodes)
- ↓/absent NK cell activity
- Ferritin ≥500 µg/L
- Soluble CD25 (sIL-2R) ≥2400 U/mL
- Treatment: Suppress inflammation (steroids, etoposide, cyclosporine A), treat underlying cause. Hematopoietic Stem Cell Transplant (HSCT) for familial/refractory cases.
⭐ Markedly elevated ferritin (often >10,000 µg/L) is a highly characteristic, though not solely diagnostic, finding in HLH supporting rapid investigation and intervention.
Histiocytosis Syndromes: Non-LCH Rarities - Rare Cell Rebels
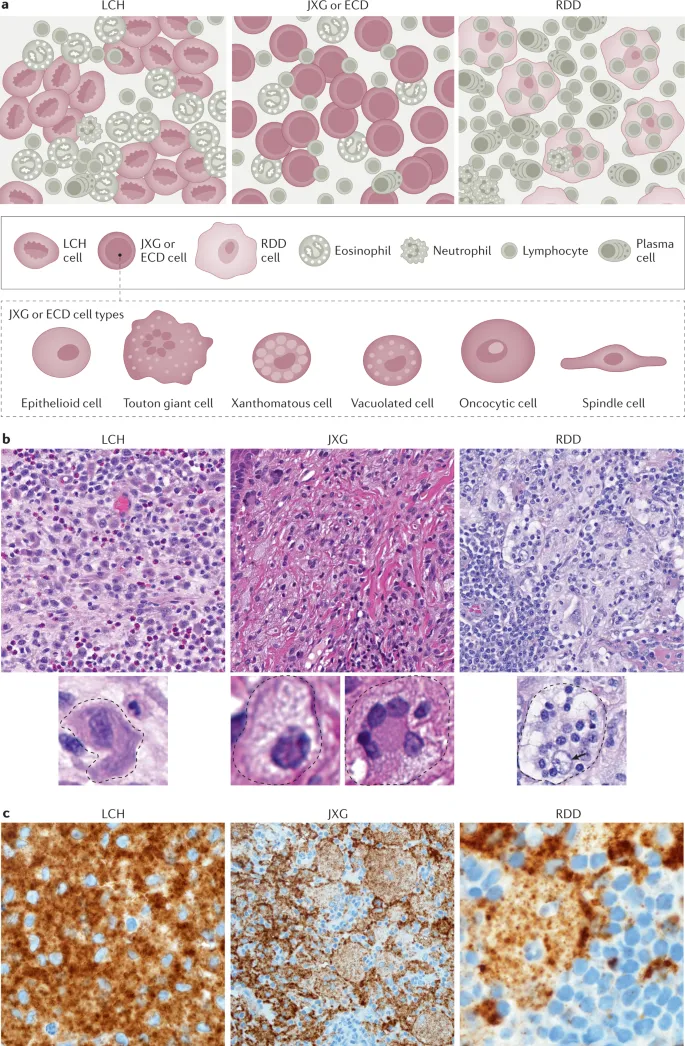
- Juvenile Xanthogranuloma (JXG)
- Benign; commonest non-LCH.
- Skin: Yellow-brown papules/nodules.
- Micro: Touton giant cells.
- Usually spontaneous regression.
- Rosai-Dorfman Disease (RDD) (Sinus Histiocytosis with Massive Lymphadenopathy)
- Painless, massive cervical lymphadenopathy.
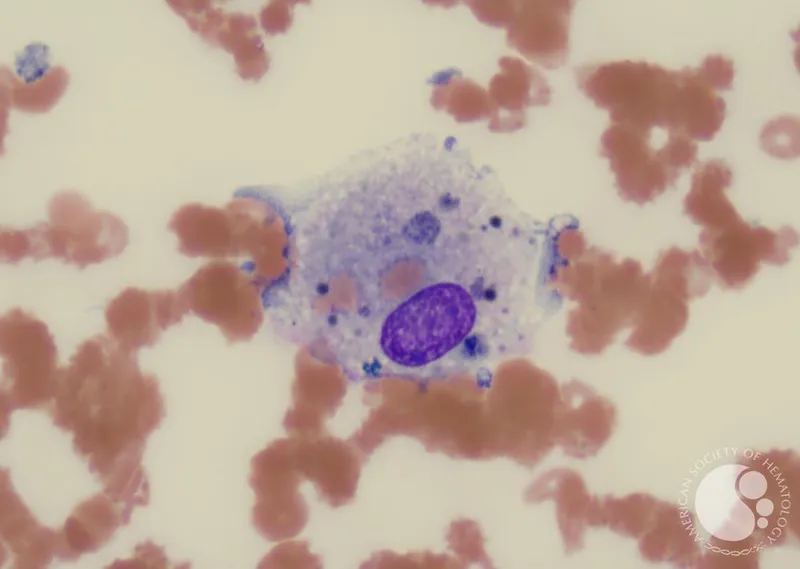
- Micro: Emperipolesis (lymphocytes within histiocytes).
- Markers: S100+, CD68+, CD1a-.
- Erdheim-Chester Disease (ECD)
- Rare, multi-systemic; older adults.
- Symmetric osteosclerosis of long bones (painful).
- BRAF V600E mutation common.
⭐ Rosai-Dorfman Disease is characterized by emperipolesis - the presence of intact lymphocytes within the cytoplasm of S100-positive histiocytes an important diagnostic feature for MCQs.
High‑Yield Points - ⚡ Biggest Takeaways
- LCH: Characterized by Birbeck granules (tennis-racket) on EM; CD1a & S100 positive.
- Most common LCH site: bone (skull); presents with lytic lesions.
- Hand-Schüller-Christian triad: lytic bone lesions, diabetes insipidus, exophthalmos.
- BRAF V600E mutation is common in LCH.
- HLH: Life-threatening cytokine storm; features include fever, splenomegaly, cytopenias.
- Key HLH diagnostic markers: ↑ ferritin, ↑ sCD25, ↓ NK cell activity, hypertriglyceridemia.
- HLH can be primary (genetic) or secondary (e.g., infections, malignancy).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

