Peds CNS Tumors: Overview - Brainy Bunch Intro
- Epidemiology:
- Most common solid tumors in children.
- 2nd most common pediatric malignancy overall (after leukemia).
- Common Locations:
- Younger children (<2 yrs): Infratentorial (posterior fossa) > Supratentorial.
- Older children/adolescents: Supratentorial predominance ↑.
- Key Predisposing Genetic Syndromes:
- Neurofibromatosis Type 1 (NF1)
- Neurofibromatosis Type 2 (NF2)
- Von Hippel-Lindau (VHL)
- Li-Fraumeni Syndrome (TP53)
- Tuberous Sclerosis Complex (TSC)

⭐ Brain tumors are the most common solid tumors in children and the second most common pediatric malignancy after leukemia.
Infratentorial Tumors - Posterior Fossa Foes
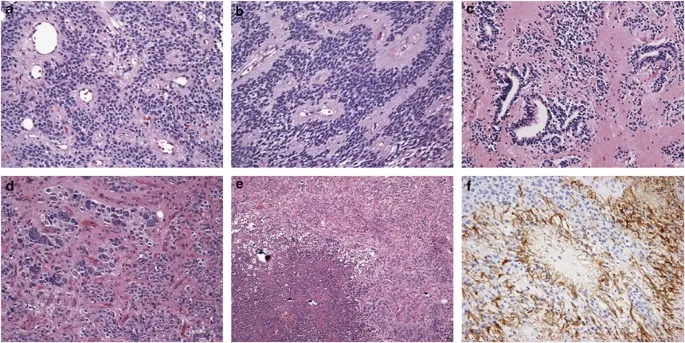
- Most common site for pediatric brain tumors. Key types:
| Tumor | Location | Key Histo | Notes |
|---|---|---|---|
| Medulloblastoma | Cerebellar vermis | Homer-Wright rosettes | MC malignant, CSF seeding, MYC amp (↓ prog) |
| Pilocytic Astro. | Cerebellum | Rosenthal fibers, GFAP+ | MC benign, cystic + mural nodule, good prog |
| Ependymoma | 4th ventricle | Perivascular pseudorosettes | Variable prog, true rosettes |
- Located in pons.
- Highly aggressive, infiltrative.
- Poor prognosis. 📌 Pons + Palsies = Poor Prognosis.
⭐ Medulloblastoma, the most common malignant pediatric brain tumor, typically arises in the cerebellar vermis and can disseminate via CSF (drop metastases), often presenting with signs of hydrocephalus.
Supratentorial Tumors - Cerebral Command Crashers
- Craniopharyngioma:
- Rathke's pouch origin.
- Suprasellar calcification, cystic ('machine oil' fluid).
- Endocrine (↓GH), visual (bitemporal hemianopsia).
⭐ Craniopharyngiomas classically show suprasellar calcification on imaging and are notorious for causing endocrine dysfunction (e.g., growth hormone deficiency) and bitemporal hemianopsia.
- Germ Cell Tumors (GCTs):
- Pineal/suprasellar location.
- Markers: ↑AFP, ↑$\beta$-hCG.
- Germinoma (common, radiosensitive), teratoma.
- Supratentorial Astrocytomas/Gliomas:
- Common pediatric brain tumors.
- Varied grades (WHO I-IV); seizures, focal deficits, ↑ICP.
- Incl. Pilocytic (optic pathway), GBM.
 oka
oka
Peds CNS Tumors: Dx & Tx - Brain Battle Plan
- Clinical Presentation:
- Raised Intracranial Pressure (ICP): Morning headache, vomiting (often projectile, unrelated to meals), papilledema, lethargy.
- Focal Neurological Deficits: Ataxia, cranial nerve palsies, seizures, endocrinopathy (e.g., diabetes insipidus, growth failure).
- Diagnosis:
- MRI with gadolinium contrast: Gold standard imaging.
- CSF cytology: For suspected leptomeningeal dissemination.
- Biopsy: Essential for histological diagnosis and grading.
- Management Principles:
- Maximal safe surgical resection.
- Radiotherapy (RT): Adjuvant; avoid/delay in children < 3 years due to neurocognitive sequelae.
- Chemotherapy: Adjuvant, neoadjuvant, or salvage; specific protocols vary by tumor type.
⭐ The 'triad' of morning headaches, vomiting (often projectile and unrelated to meals), and lethargy strongly suggests raised intracranial pressure (ICP), a common presentation of pediatric brain tumors.
High‑Yield Points - ⚡ Biggest Takeaways
- CNS tumors: most common solid tumors in children; infratentorial more frequent.
- Pilocytic astrocytoma: most common pediatric brain tumor; often cerebellar, Rosenthal fibers.
- Medulloblastoma: most common malignant; cerebellar (vermis); Homer Wright rosettes, radiosensitive.
- Craniopharyngioma: from Rathke's pouch; suprasellar calcification; visual defects.
- Ependymoma: often in 4th ventricle; causes hydrocephalus; perivascular pseudorosettes.
- Key symptoms: morning headache, vomiting, ataxia, papilledema.
- Brainstem gliomas (e.g., DIPG) have a dismal prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

